Articles
- Page Path
- HOME > Osong Public Health Res Perspect > Volume 12(4); 2021 > Article
-
Original Article
Behavioral therapy and pharmacotherapy for relapse prevention in abstinent smokers: a rapid review and meta-analysis for the Korea Preventive Service Task Force -
Naae Lee1
 , Eon Sook Lee2
, Eon Sook Lee2 , Jae Moon Yun3
, Jae Moon Yun3 , Cheol Min Lee4
, Cheol Min Lee4 , Seung-Won Oh4
, Seung-Won Oh4 , Younglee Choi5
, Younglee Choi5 , Belong Cho3
, Belong Cho3
-
Osong Public Health and Research Perspectives 2021;12(4):244-253.
DOI: https://doi.org/10.24171/j.phrp.2021.0017
Published online: May 27, 2021
1Department of Public Health Science, Graduate School of Public Health, Seoul National University, Seoul, Korea
2Department of Family Medicine, Ilsan Paik Hospital, Inje University College of Medicine, Goyang, Korea
3Department of Family Medicine, Seoul National University Hospital, Seoul, Korea
4Department of Family Medicine, Healthcare System Gangnam Center, Seoul National University Hospital, Seoul, Korea
5Biomedical Research Institute, Seoul National University Hospital, Seoul, Korea
- Corresponding author: Belong Cho Department of Family Medicine, Seoul National University Hospital, 101 Daehak-ro, Jongno-gu, Seoul 03080, Korea E-mail: belong@snu.ac.kr
- Naae Lee and Eon Sook Lee contributed equally as co-first authors.
© 2021 Korea Disease Control and Prevention Agency
This is an open access article under the CC BY-NC-ND license (http://creativecommons.org/licenses/by-nc-nd/4.0/).
- 5,909 Views
- 93 Download
- 1 Crossref
Abstract
-
Objectives
- This study aimed to assess the effectiveness of relapse prevention interventions involving behavioral and pharmacological treatment among abstinent smokers.
-
Methods
- This rapid review was conducted using MEDLINE, Cochrane CENTRAL, CINAHL, Embase, KMbase, and KoreaMed to identify studies published until June 20, 2020. The participants were abstinent smokers who quit smoking on their own, due to pregnancy, hospitalization, or by participating in a smoking cessation program. We found a systematic review that fit the objective of this study and included 81 randomized controlled trials (RCTs). Studies that did not present information on smoking cessation status, had no control group, or used reward-based interventions were excluded. Random effect and fixed effect meta-analyses were used to estimate the relative risk (RR) and 95% confidence interval (CI). In subgroup analyses, differences between subgroups were verified based on the participant setting, characteristics, intervention type, and intensity.
-
Results
- Following screening, 44 RCTs were included in the meta-analysis. The review reported no differences in the success rate of relapse prevention between the behavioral interventions. Pharmacotherapy interventions showed higher success rates (RR, 1.15; 95% CI, 1.05−1.26; I2=40.71%), depending on prior abstinence duration and the drug type.
-
Conclusion
- The results indicated that pharmacotherapy has a significant effect on preventing relapse among abstinent smokers.
- Smoking is one of the major global causes of morbidity and mortality, with about half of smokers dying from smoking-related diseases [1]. Research on the health effects of smoking began in the early 1960s, and in 1964, general surgeons in the United States released a research report [2]; since then, many epidemiological studies have examined the harmful effects of tobacco. According to the World Health Organization, more than 8 million people per year die due to tobacco-related addiction [3]; among these, 7 million deaths can be directly attributed to tobacco. Smoking increases the risk of chronic diseases, such as chronic obstructive pulmonary disease, hypertension, cardiovascular diseases, and susceptibility to cancer [4,5]. The health effects of smoking contribute to the burden of disease nationally and globally, especially in developing countries [6].
- According to Statistics Korea, since 2010, the percentage of smokers who have attempted to quit smoking for more than 24 hours in the last year has been steadily increasing, reaching 52.7% in 2018 [7]. According to the findings of the European Network for Smoking and Tobacco Prevention, the relapse rate of smokers who quit smoking unaided tends to increase over time. A study reported complete abstinence rates among abstinent smokers of 19% at 4 weeks after quitting, 10% at 6 months, and 5% at 1 year [8]. Many smokers attempt to quit smoking with a desire to improve their health; however, they are unsuccessful due to severe nicotine withdrawal symptoms [9]. Nicotine dependence has been found to be a strong predictor of the success of smoking cessation [10]. Therefore, the process of abstinence requires multiple attempts, instead of a single trial [11], and it may occur after different durations of cessation attempts [12].
- In this study, relapse refers to the phenomenon of recurrence of smoking amidst the process of attempting to quit smoking. During the smoking cessation process, behavioral changes are observed in people who try to quit smoking, which gradually leads to relapse after a period of abstinence [8]. Several interventions can help smokers continue on their path of smoking cessation. Behavioral therapies, such as cognitive-behavioral therapy, and pharmacological approaches are relapse interventions that help abstainers continue on their path of smoking cessation [13]. However, the success rate of abstinence decreases steadily over time due to relapses [14]. In addition, randomized controlled trials (RCTs) have reported mixed findings concerning the efficacy and long-term success of relapse prevention for smoking cessation [15].
- In this study, we aimed to conduct an updated rapid review and meta-analysis of these RCT studies to examine the effectiveness of relapse prevention interventions in behavioral and pharmacological treatment among abstinent smokers who successfully quit smoking. This review provides updated evidence, including additional studies from another recent review. This study aims to provide sufficient evidence to recommend appropriate relapse prevention interventions for smoking cessation to the Korea Preventive Service Task Force (KPSTF).
Introduction
- A rapid review of behavioral therapy and pharmacotherapy for relapse prevention was conducted using the KPSTF’s rapid review method to examine available evidence within a limited timeline [16]. The study protocol was approved by the KPSTF.
- Search Strategy
- We searched the following electronic international databases: MEDLINE, Cochrane Central Register of Controlled Trials (CENTRAL), Embase, and the Cumulative Index to Nursing and Allied Health Literature (CINAHL). Additionally, domestic databases included KoreaMed and KMbase. The search terms included “relapse prevention,” “recurrence,” “smoking cessation,” “smoke,” “tobacco,” and other relevant terms. As per the process of a rapid review, a systematic review (SR) or meta-analysis of the RCTs was explored initially. If we found an SR that could answer the key questions and aligned well with our inclusion and exclusion criteria, then we selected the most recent published SR fitting those criteria. Additional search strategies employed are provided in the supplementary files (Methods S1). There was no restriction on the publication year, and the most recent search date was June 19, 2020. The studies selected for this review were published in Korean and English.
- Inclusion and Exclusion Criteria (PICO)
- Studies conducting randomized controlled clinical trials were included in this review, while those with a follow-up period of less than 6 months were excluded.
- The participants of the included studies were abstinent smokers, who voluntarily quit smoking (unassisted abstainers) or who quit smoking due to pregnancy, hospitalization, or by participating in a smoking cessation program (assisted abstainers). Abstinent smokers were defined as individuals who did not smoke at all within at least 24 hours. Participants who did not provide smoking cessation status at entry, who served in the military, or who did not report success at quitting smoking within 24 hours before entry were excluded.
- Regarding the intervention, RCTs employing behavioral support and extended use of smoking cessation medication intended to prevent relapse were included. Among the included studies, pharmacological intervention studies for smoking cessation used placebos for the control groups, while behavioral intervention studies for smoking cessation used no intervention, regular care, or minimal interventions for the control groups. Intervention studies with reward-based incentives were excluded.
- Outcome Measure
- The primary outcome was the prolonged or point abstinence rate at 6 months or more of follow-up from RCTs. For trials that reported multiple follow-up studies, we chose the longest follow-up duration for the primary outcome. Biochemical tests involving the exhaled carbon monoxide level or cotinine level in saliva or urine and self-report were employed to verify continuing abstinence. The secondary outcome was the prolonged or point abstinence rate at less than 6 months of follow-up when that was reported.
- Data Collection and Processing
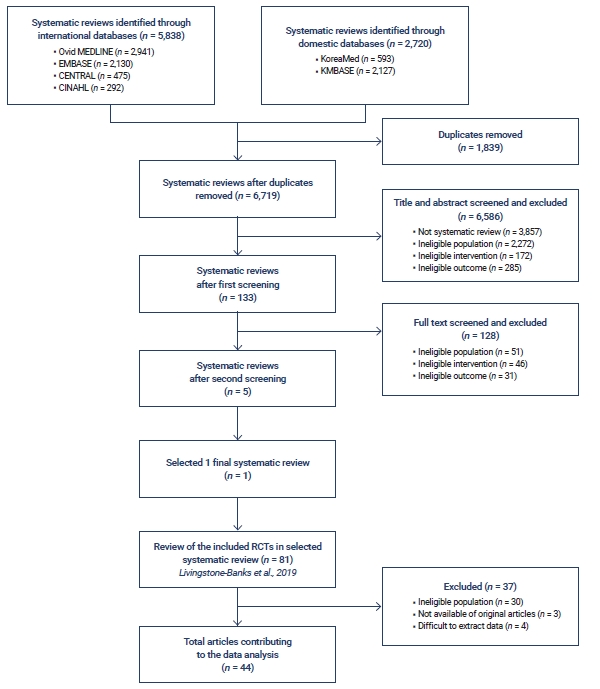
- While selecting the studies for the rapid review, 2 reviewers identified potentially eligible studies for inclusion. First, the titles were screened, followed by the selection of the abstract and the full text of the articles for the review. SRs were screened by checking the inclusion and exclusion criteria before selecting relevant studies. Two reviewers cross-checked independently, and a third reviewer checked the selected articles and all of them reached a consensus. In order to prevent bias, the findings of all studies were carefully reviewed, and any duplicated research was excluded (Figure 1).
- After finding the final SR for our study, 2 reviewers cross-checked the included RCTs to verify that they matched the inclusion and exclusion criteria. After selecting the studies, the following data from each RCT were identified: year of publication, author, intervention type, country, setting, number of participants, and abstinence verification method.
- Quality Assessment
- A Measurement Tool to Assess Systematic Reviews (AMSTAR) helps develop and evaluate SRs; moreover, it helps users focus on their methodological quality [17]. It comprises 11 items with 4 types of responses: “yes,” “no,” “can’t answer,” or “not applicable.” The instrument incorporates the study design, characteristics, and data extraction, literature search including the gray literature, a combination of study results, publication bias, and conflict of interest. AMSTAR quality scores range from 0 to 11, where scores of 0 to 3 indicate low quality, 4 to 7 moderate quality, and 8 to 11 high quality. Finally, 5 SRs were selected; of which 2 that scored a higher rating and a recent Cochrane review published in 2019 were finally selected.
- The study of Livingstone-Banks et al. [14], which was published in the Cochrane Library in October 2019 and aimed to assess relapse prevention interventions among recent quitters who relapsed to smoking, was used for this analysis. Studies until May 2019 using randomized or quasi-RCTs with a minimum of 6 months of follow-up from the quitting date were systematically reviewed.
- Statistical Analysis
- In the meta-analysis, statistical heterogeneity was tested by a graphical representation of study data through the forest plots and the Higgins I2 test statistic. The Higgins I2 test statistic indicates the proportion of variation between the sample estimates; an I2 value ≥50% indicates significant heterogeneity [18]. The Mantel-Haenszel method, which applies a fixed-effect model, is suitable when the number of studies is small. The DerSimonian and Laird method, which uses a random-effects model, has been used for a long time and measures overall effect estimates more accurately even with larger heterogeneity [19]. Considering the characteristics of studies and the statistical tests, a fixed-effects model was used when I2 <50% and a random-effects model was used when I2 >50%.
- Publication bias was tested using a funnel plot and the Egger test, which tests the linear relationship between the effect estimate and the standard error [20]. In order to identify significant effects of relapse prevention programs based on behavioral therapy and pharmacotherapy, differences between subgroups were verified according to participants’ recruitment setting and characteristics, publication year and country, the type and intensity of intervention, the verification method of abstinence, publication bias, and reported conflict of interest, as analyzed using the Cochrane Q test. The risk of bias was analyzed using the Cochrane Collaboration’s recommended tool to check the quality of the included studies. All analyses were performed using Stata/MP ver. 16.1 (StataCorp., College Station, TX, USA).
Materials and Methods
- Search Results
- A total of 44 RCTs met the inclusion and exclusion criteria of the present study. Overall, 5,838 SRs were retrieved from 4 international databases; 4,630 of these were retained after removing duplicate studies by matching the title with the author. A total of 128 relevant studies were selected by screening the title and abstract, and 1 SR was eventually chosen. For the rapid review process, among the 81 RCTs in the selected SR, 44 RCTs were finally included in the meta-analysis. Figure 1 depicts the literature flow, and an attached supplementary file provides detailed information about the included studies (Table S1).
- Effects of the Behavioral Therapy Intervention
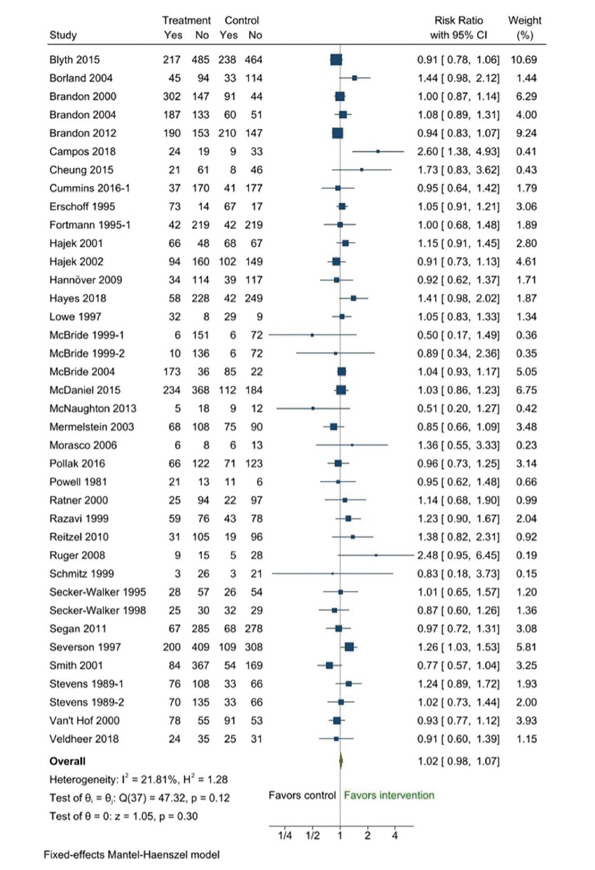
- Out of the 44 RCTs, 36 with relapse prevention interventions involving behavioral therapy were included; with 4 RCTs evaluating the effects of multiple behavioral therapy interventions. The 38 behavioral interventions resulted in no significant difference in the smoking cessation success rate for the intervention group over 6 months compared to the control group (relative risk [RR], 1.02; 95% confidence interval [CI], 0.98−1.07; I2=21.81%) (Table 1, Figure 2). The funnel plot and Egger test were used to identify publication bias among studies of behavioral therapy. No publication bias was observed after visually evaluating the funnel plot or according to the Egger test (p=0.18), as shown in Figure S1.
- Of the 36 RCTs with 38 intervention groups for the secondary outcome, 12 RCTs reported outcomes at less than 6 months. The success rate of smoking cessation of the intervention group was not significantly higher than that of the control group (RR, 1.04; 95% CI, 0.98−1.10; I2=23.77%). Furthermore, no publication bias was detected (p=0.29) using the Egger test.
- Effects of Pharmacotherapy Interventions
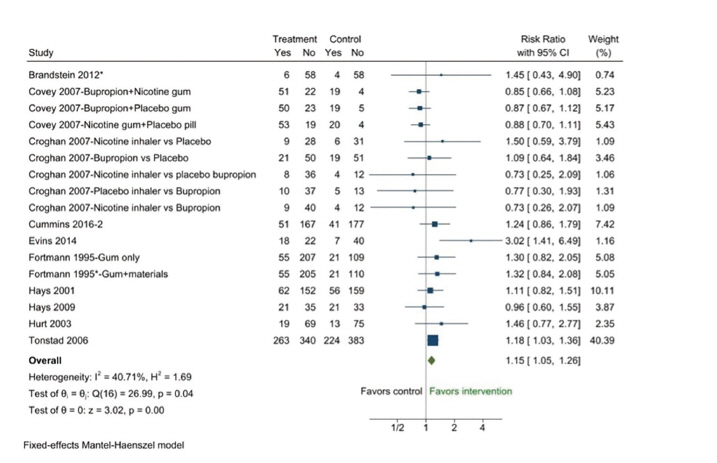
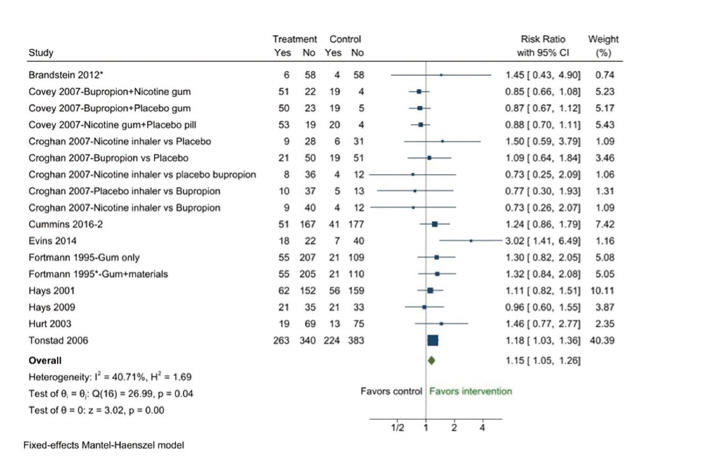
- There were 10 RCTs on relapse prevention interventions based on pharmacotherapy, with 3 RCTs evaluating the effect of multiple interventions. Seventeen pharmacotherapy intervention groups showed significant effects on the success rate of smoking cessation compared to the control groups (RR, 1.15; 95% CI, 1.05−1.26; I2=40.71%) (Table 2, Figure 3). There was no publication bias in the funnel plot (Figure S1) or in the Egger test (p=0.46).
- Among the 10 RCTs with 17 intervention groups, 7 (12 intervention groups) reported outcomes at less than 6 months as a secondary outcome. The success rate in the intervention group was significantly higher than in the control group (RR, 1.13; 95% CI, 1.02−1.25, I2=57.44%). The Egger test detected no publication bias (p=0.23).
- Risk of Bias
- A risk of bias assessment was performed on selected documents using the Cochrane Risk of Bias tool [21]. Incomplete outcome data (attrition bias), blinding of outcome assessment (detection bias), blinding participants and personnel (performance bias), allocation concealment (selection bias), and random sequence generation (selection bias) were evaluated using 3 grades: low, high, and unclear risk of bias. Of the studies evaluating behavioral therapy, 1 study was evaluated as having a high risk of bias in random sequence generation, 5 studies in allocation concealment, 2 in blinding participants and personal, and 4 in blinding of outcome assessment. Regarding incomplete outcome data, 9 studies with behavioral interventions were unclear and 1 study reporting a pharmacotherapy intervention had a high risk of bias (Figure S2).
- Subgroup Analysis
- Subgroup analyses were conducted to assess significant factors associated with the efficacy of relapse prevention interventions. Participants were divided into groups based on their characteristics: participants’ recruitment setting, whether they enrolled in the smoking cessation program, were pregnant or hospitalized, the country of study, publication year, intervention type of behavioral therapy (counseling, self-help materials, or booklets), the intensity of the intervention, prior abstinence, verification method of abstinence, publication bias, and reports of conflicts of interest. There were no statistically significant differences among the subgroups in the behavioral intervention studies.
- For the pharmacotherapy interventions, subgroup analyses were conducted among the following groups based on participants’ recruitment setting, the characteristics of participants, whether they enrolled patients in the smoking cessation program or hospitalized inpatients, type of country, publication year, the intensity of the intervention, prior abstinence, verification method of abstinence, publication bias, reports of conflicts of interest, and drug type in pharmacotherapy (nicotine replacement therapy [NRT], bupropion, or varenicline). The success rate of smoking cessation varied depending on the type of drug (p=0.047); while interventions with varenicline showed a significantly higher success rate, other modes of intervention that used different drugs did not show significant differences. Therefore, we excluded studies with varenicline, and no significant results were confirmed (RR, 0.97; 95% CI, 0.97−1.23). In addition, the success rate of smoking cessation varied depending on the duration of prior abstinence (p=0.001); specifically, the success rate of smoking cessation was significantly higher when the baseline abstinence period was less than 4 weeks.
Results
- We investigated the effectiveness of the relapse prevention program for abstinent smokers based on behavioral therapy or pharmacotherapy using a rapid review to develop a recommendation. Evidence from 44 RCTs reported that relapse prevention programs using pharmacotherapy increased the success rate of smoking cessation compared to control groups who used placebos. However, we could not find any difference in the success rate of smoking cessation between the intervention groups incorporating behavioral therapy and usual care. In this study, a meta‐analysis was conducted by selecting the latest review about interventions for relapse prevention. Although several studies were excluded based on the exclusion criteria, the results from the included SR by Livingstone-Banks et al. [14] were consistent with those of this study. Our selected SR reported that the evidence does not support the use of behavioral interventions for assisted abstainers (RR, 0.98; 95% CI, 0.87−1.11) which is consistent with all previous studies. With pharmacotherapy, extended treatment helps in abstinence, but bupropion was not helpful and not enough evidence was available on NRT. Since we narrowed the scope of inclusion and exclusion criteria compared to the previous SR, we could conclude that the results were consistent.
- In this review, a significant effect of existing behavioral interventions for relapse prevention among smoking abstainers was not detected. This indicates that the behavioral interventions provided no worthwhile benefit in preventing relapse in abstainers. However, a review of behavioral interventions of relapse prevention for abstainers by Agboola et al. [22] detected more positive results than those found in the present study. Although there are some discrepancies between prior reviews and this study, the differences in conclusions are not attributable to the included studies and are instead due to decisions related to subgroups and outcomes.
- Furthermore, the results for some pharmacotherapies were more encouraging. Our study result reported that the extended use of smoking cessation drugs aided 15% of abstainers in maintaining successful smoking cessation, after 6 months of follow-up. The effect of pharmacological interventions was also observed at a shorter follow-up period, and was more prominent in abstainers at less than 4 weeks since quitting smoking. This might be a period when abstainers suffer from withdrawal symptoms. Some large and well-conducted studies illustrated the beneficial effects of varenicline in preventing relapse. However, studies on NRT or bupropion did not detect an effect on relapse prevention for abstainers. Varenicline is the most frequently prescribed medication for smoking cessation (87.9%) in the smoking cessation support services provided by the National Health Insurance Service [23]. This review provides evidence that pharmacological interventions, especially varenicline prescriptions, help abstinent smokers to continue their path of not smoking for over 6 months.
- There are several limitations of this review. Firstly, the type and intensity of the behavioral therapy interventions in each study were highly variable; therefore, these conclusions about behavior therapy cannot be considered conclusive. Future studies should include RCTs with a single type of behavioral therapy intervention to further explore our conclusions about the effects of behavioral therapy on relapse prevention. Some studies applied a single intervention, but there were also complex interventions that applied 2 or more approaches. Accordingly, various subgroup analyses were performed. However, no significant effective specific behavioral therapy could be identified. Further research is required to provide more substantial results.
- We intended to conduct a rapid SR that included RCTs conducted in Korea by searching Korean databases, but we could not find and include RCTs using Korean participants; thus, it was not possible to confirm any of these findings of relapse prevention within the Korean context. These findings are meaningful and extracted from Korean databases; however, they indicate the need for an RCT on relapse prevention among the Korean population.
- In terms of the limitations of pharmacotherapy, the subgroup analyses confirmed that the effect of pharmacotherapy depends on the drug type; however, it cannot be claimed that varenicline is the only successful drug for relapse prevention. To overcome this limitation, a subgroup analysis was conducted excluding those with varenicline, but no significant results were found. In addition, a combined program (behavioral and pharmacotherapy treatment) was reported to be more effective in smoking cessation than a single independent treatment [8]. However, in this review, no significant effects were revealed through various subgroup analyses. Moreover, it cannot be asserted that combined programs are not effective in preventing relapse, because only a small number of studies used combined programs and those studies used NRT.
Discussion
- In summary, this study confirmed that pharmacotherapy interventions improved the success rate of smoking cessation for abstainers through an analysis of 44 RCTs focusing on relapse prevention programs. To encourage and recommend effective relapse prevention programs, a sufficient number of studies with large populations and long-term follow-up assessments should be conducted using each drug for smoking cessation or combined interventions.
Conclusion
Supplementary Material
Figure S1.
Figure S2.
-
Ethics Approval
Not applicable.
-
Conflicts of Interest
The authors have no conflicts of interest to declare.
-
Funding
This article was supported by a Korea Disease Control and Prevention Agency (KDCA) research project, ‘Evidence Evaluation Center Operation Support for Community Chronic Disease Prevention and Control Project’ (Project No: B008011400150), in 2020. The content is solely the responsibility of the authors and does not necessarily represent the official views of the KDCA. We are grateful to Geumju Song for her support and guidance throughout the project.
-
Availability of Data
All data generated or analyzed during this study are included in this published article. For other data, these may be requested through the corresponding author.
-
Authors’ Contributions
Conceptualization: all authors; Data curation: NL, EL; Formal analysis: NL, EL; Investigation: all authors; Methodology: all authors; Project administration: BC; Resources: all authors; Software: all authors; Supervision: BC; Validation: all authors; Visualization: all authors; Writing–original draft: NL, EL; Writing–review & editing: all authors.
Article information

- 1. Centers for Disease Control and Prevention (CDC). Fast facts [Internet]. Atlanta: CDC; 2020 [cited 2020 Oct 27]. Available from: https://www.cdc.gov/tobacco/data_statistics/fact_sheets/fast_facts/index.htm.
- 2. Centers for Disease Control and Prevention (CDC). Smoking cessation: a report of the surgeon general [Internet]. Atlanta: CDC; 2020 [cited 2020 Oct 27]. Available from: https://www.cdc.gov/tobacco/data_statistics/sgr/2020-smoking-cessation/index.html.
- 3. World Health Organization (WHO). Tobacco [Internet]. Geneva: WHO; 2020 [cited 2020 Nov 1]. Available from: https://www.who.int/news-room/fact-sheets/detail/tobacco.
- 4. Wang R, Jiang Y, Yao C, et al. Prevalence of tobacco related chronic diseases and its role in smoking cessation among smokers in a rural area of Shanghai, China: a cross sectional study. BMC Public Health 2019;19:753. ArticlePubMedPMC
- 5. Jacob L, Freyn M, Kalder M, et al. Impact of tobacco smoking on the risk of developing 25 different cancers in the UK: a retrospective study of 422,010 patients followed for up to 30 years. Oncotarget 2018;9:17420−9.ArticlePubMedPMC
- 6. GBD 2015 Tobacco Collaborators. Smoking prevalence and attributable disease burden in 195 countries and territories, 1990-2015: a systematic analysis from the Global Burden of Disease Study 2015. Lancet 2017;389:1885−906.PubMedPMC
- 7. Statistics Korea. 2018 National Health Statistics [Internet]. Daejeon: Statistics Korea; 2019 [cited 2020 Oct 30]. Available from: https://www.index.go.kr/potal/main/EachDtlPageDetail.do?idx_cd=2771.
- 8. European Network for Smoking and Tobacco Prevention. 2018 Guidelines for treating tobacco dependence [Internet]. 4th ed. Brussels: European Publishing; 2018 [cited 2020 Nov 15]. Available from: http://elearning-ensp.eu/mod/page/view.php?id=532.
- 9. Komiyama M, Takahashi Y, Tateno H, et al. Support for patients who have difficulty quitting smoking: a review. Intern Med 2019;58:317−20.ArticlePubMed
- 10. Lee CW, Kahende J. Factors associated with successful smoking cessation in the United States, 2000. Am J Public Health 2007;97:1503−9.ArticlePubMedPMC
- 11. McDermott MS, Marteau TM, Hollands GJ, et al. Change in anxiety following successful and unsuccessful attempts at smoking cessation: cohort study. Br J Psychiatry 2013;202:62−7.ArticlePubMed
- 12. Caponnetto P, Keller E, Bruno CM, et al. Handling relapse in smoking cessation: strategies and recommendations. Intern Emerg Med 2013;8:7−12.ArticlePubMed
- 13. Heckman BW, Cummings KM, Kasza KA, et al. Effectiveness of switching smoking-cessation medications following relapse. Am J Prev Med 2017;53:e63−70.ArticlePubMedPMC
- 14. Livingstone-Banks J, Norris E, Hartmann-Boyce J, et al. Relapse prevention interventions for smoking cessation. Cochrane Database Syst Rev 2019;2019:CD003999. ArticlePubMed
- 15. Durcan MJ, White J, Jorenby DE, et al. Impact of prior nicotine replacement therapy on smoking cessation efficacy. Am J Health Behav 2002;26:213−20.ArticlePubMed
- 16. Kim S, Shin S, Seo H, et al. KPSTF Guidance for undertaking rapid systematic review. Seoul: Korea Preventive Services Task Forces; 2017.
- 17. Shea BJ, Hamel C, Wells GA, et al. AMSTAR is a reliable and valid measurement tool to assess the methodological quality of systematic reviews. J Clin Epidemiol 2009;62:1013−20.ArticlePubMed
- 18. Sedgwick P. Meta-analyses: what is heterogeneity? BMJ 2015;350:h1435. ArticlePubMed
- 19. Kontopantelis E, Springate DA, Reeves D. A re-analysis of the Cochrane Library data: the dangers of unobserved heterogeneity in meta-analyses. PLoS One 2013;8:e69930.ArticlePubMedPMC
- 20. Egger M, Davey Smith G, Schneider M, et al. Bias in meta-analysis detected by a simple, graphical test. BMJ 1997;315:629−34.ArticlePubMedPMC
- 21. Higgins JP, Altman DG, Gotzsche PC, et al. The Cochrane Collaboration's tool for assessing risk of bias in randomised trials. BMJ 2011;343:d5928. ArticlePubMedPMC
- 22. Agboola S, McNeill A, Coleman T, et al. A systematic review of the effectiveness of smoking relapse prevention interventions for abstinent smokers. Addiction 2010;105:1362−80.ArticlePubMed
- 23. Lee C, Cho JM, Kim KJ, et al. Association of satisfactory smoking cessation support services and treatment administered with successful quitting of smoking in Korea. J Korean Soc Res Nicotine Tob 2019;10:62−71.Article
References
Figure & Data
References
Citations

- A Survey of the Clinical Practice of Korean Medicine for Smoking Cessation in Public Health Centers: A Web-Based Survey of Public Health Doctors of Korean Medicine
Gyoungeun Park, Jeong-Hyun Moon, Eun-Jung Kim, Byung-Kwan Seo, Yong-Hyeon Baek, Won-Suk Sung
Perspectives on Integrative Medicine.2024; 3(1): 45. CrossRef


 PubReader
PubReader ePub Link
ePub Link Cite
Cite