Previous issues
- Page Path
- HOME > Articles and issues > Previous issues
Editorial
- Now is the time to consider measures against next wave of COVID-19
- Jong-Koo Lee
- Osong Public Health Res Perspect. 2021;12(6):343-345. Published online December 28, 2021
- DOI: https://doi.org/10.24171/j.phrp.2021.0338
- 3,561 View
- 71 Download
Review Article
- Social determinants of adherence to COVID-19 preventive guidelines: a comprehensive review
- Zahra Jorjoran Shushtari, Yahya Salimi, Sina Ahmadi, Nader Rajabi-Gilan, Marzieh Shirazikhah, Akbar Biglarian, Ali Almasi, Mohammad Ali Mohammadi Gharehghani
- Osong Public Health Res Perspect. 2021;12(6):346-360. Published online December 21, 2021
- DOI: https://doi.org/10.24171/j.phrp.2021.0180
- 7,437 View
- 161 Download
- 19 Web of Science
- 20 Crossref
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material 
- Adherence to coronavirus disease 2019 (COVID-19) preventive guidelines (ACPG) is an important strategy to control the COVID-19 pandemic effectively. The present study aimed to identify and summarize the social determinants of ACPG among the general population. A comprehensive review was performed from December 2019 to February 2021 through searching electronic databases. Two independent reviewers assessed and selected relevant studies. Next, the characteristics and main findings of the included studies were summarized. Finally, the World Health Organization’s conceptual framework of social determinants of health was used to synthesize the identified social determinants of ACPG. Forty-one of 453 retrieved articles met the inclusion criteria. The study results showed different patterns of ACPG among various communities. Furthermore, 84 social determinants were identified and categorized into structural and intermediary determinants. ACPG is a set of complex behaviors associated with different individual sociodemographic and behavioral characteristics; living and working conditions; COVID-19 knowledge, attitudes, and risk perceptions; exposure to sources and information level; leisure activities; social support; trust; social norms; psychosocial well-being; socio-economic position; and the socio-economic and political context. Interventions to promote ACPG among the general population should consider the identified social determinants of ACPG.
-
Citations
Citations to this article as recorded by- ISO 50001 based energy management system: a bibliometric perspective
Marlina Pandin, Sik Sumaedi, Aris Yaman, Meilinda Ayundyahrini, Nina Konitat Supriatna, Nurry Widya Hesty
International Journal of Energy Sector Management.2024;[Epub] CrossRef - Impact of long COVID-19 on posttraumatic stress disorder as modified by health literacy: an observational study in Vietnam
Han Thi Vo, Tien Duc Dao, Tuyen Van Duong, Tan Thanh Nguyen, Binh Nhu Do, Tinh Xuan Do, Khue Minh Pham, Vinh Hai Vu, Linh Van Pham, Lien Thi Hong Nguyen, Lan Thi Huong Le, Hoang Cong Nguyen, Nga Hoang Dang, Trung Huu Nguyen, Anh The Nguyen, Hoan Van Nguye
Osong Public Health and Research Perspectives.2024; 15(1): 33. CrossRef - Cognitive predictors of COVID-19 mitigation behaviors in vaccinated and unvaccinated general population members
Anna Hudson, Peter A. Hall, Sara C. Hitchman, Gang Meng, Geoffrey T. Fong
Vaccine.2023; 41(27): 4019. CrossRef - Utilisation of rehabilitation due to mental disorders during the SARS-CoV-2 pandemic: a difference-in-differences analysis
Matthias Bethge, David Fauser, Pia Zollmann, Marco Streibelt
BMC Psychiatry.2023;[Epub] CrossRef - Perceptions about COVID-19 preventive measures among Ghanaian women
Frank Kyei-Arthur, Martin Wiredu Agyekum, Grace Frempong Afrifa-Anane, Reuben Tete Larbi, Peter Kisaakye, Dario Ummarino
PLOS ONE.2023; 18(4): e0284362. CrossRef - Cognitive and Emotional Motivation to Explain Infection-Prevention Behaviors with Social Support as a Mediator During the COVID-19 Pandemic: A Nationwide Cross-Sectional Study in Korea
Myonghwa Park, Keunyeob Oh, Hyungjun Kim, Xing Fan, Thi-Thanh-Thnh Giap, Rhayun Song
Patient Preference and Adherence.2023; Volume 17: 1063. CrossRef - Factors Influencing COVID-19 Prevention Behavior: A Community-based Cross-sectional Study
Ernawaty Ernawaty, Nabilla Belqys Dherindri
Open Access Macedonian Journal of Medical Sciences.2023; 11(E): 191. CrossRef - The Impact of the COVID-19 Pandemic on Outcomes in Acute Pancreatitis: A Propensity Score Matched Study Comparing before and during the Pandemic
Patricia Mihaela Rădulescu, Elena Irina Căluianu, Emil Tiberius Traşcă, Dorin Mercuţ, Ion Georgescu, Eugen Florin Georgescu, Eleonora Daniela Ciupeanu-Călugăru, Maria Filoftea Mercuţ, Răzvan Mercuţ, Vlad Padureanu, Costin Teodor Streba, Cristina Călăraşu,
Diagnostics.2023; 13(14): 2446. CrossRef - COVID-19 in social networks: unravelling its impact on youth risk perception, motivations and protective behaviours during the initial stages of the pandemic
Marta Anson, Ksenia Eritsyan
International Journal of Adolescence and Youth.2023;[Epub] CrossRef - Bi-directional associations between mask usage and beliefs about reasons for masking before and after the downgrading of the legal status of COVID-19 in Japan: A longitudinal study
Michio Murakami
International Journal of Disaster Risk Reduction.2023; 97: 104072. CrossRef - Geoepidemiological perspective on COVID-19 pandemic review, an insight into the global impact
Alexandre Vallée
Frontiers in Public Health.2023;[Epub] CrossRef - The Effect of COVID-19 Pandemic on Using CTS and MRI in Iran: Evidence from an Interrupted Time Series Analysis
Monireh Mahmood Pour-Azari, Nasim Badiee, Ali Kazemi Karyani, Shahin Soltani, Satar Rezaei
Journal of Health Reports and Technology.2023;[Epub] CrossRef - Association between social isolation and loneliness with COVID-19 vaccine uptake in Japan: a nationwide cross-sectional internet survey
Tomohiko Ukai, Takahiro Tabuchi
BMJ Open.2023; 13(11): e073008. CrossRef - Exploration of factors associated with mask-wearing and hand disinfection in Japan after the coronavirus disease outbreak: A longitudinal study
Michio Murakami, Mei Yamagata, Asako Miura
International Journal of Disaster Risk Reduction.2023; 98: 104107. CrossRef - Social Determinants of Adherence to COVID-19 Preventive Guidelines in Iran: A Qualitative Study
Sina Ahmadi, Zahra Jorjoran Shushtari, Marzieh Shirazikhah, Akbar Biglarian, Seyed Fahim Irandoost, Toktam Paykani, Ali Almasi, Nader Rajabi-Gilan, Nafiul Mehedi, Yahya Salimi
INQUIRY: The Journal of Health Care Organization, .2022; 59: 004695802210841. CrossRef - Determinants of observing health protocols related to preventing COVID-19 in adult women: A qualitative study in Iran
Javad Yoosefi Lebni, Saeede Pavee, Mandana Saki, Arash Ziapour, Ahmad Ahmadi, Mehdi Khezeli
Frontiers in Public Health.2022;[Epub] CrossRef - Adherence to Coronavirus Disease 2019 Preventive Measures in a Representative Sample of the Population of the Canton of Vaud, Switzerland
Audrey Butty, Nolwenn Bühler, Jérôme Pasquier, Julien Dupraz, Vincent Faivre, Sandrine Estoppey, Cloé Rawlinson, Semira Gonseth Nusslé, Murielle Bochud, Valérie D’Acremont
International Journal of Public Health.2022;[Epub] CrossRef - Quarantine preparedness – the missing factor in COVID-19 behaviour change? Qualitative insights from Australia
Angela Davis, Stephanie Munari, Joseph Doyle, Brett Sutton, Allen Cheng, Margaret Hellard, Lisa Gibbs
BMC Public Health.2022;[Epub] CrossRef - The impact of COVID-19 pandemic on hospital admissions for nine diseases in Iran: insight from an interrupted time series analysis
Sina Ahmadi, Ali Kazemi-Karyani, Nasim Badiee, Sarah Byford, Ali Mohammadi, Bakhtiar Piroozi, Satar Rezaei
Cost Effectiveness and Resource Allocation.2022;[Epub] CrossRef - Psychosocial Determinants of Hand Hygiene, Facemask Wearing, and Physical Distancing During the COVID-19 Pandemic: A Systematic Review and Meta-analysis
Wei Liang, Yanping Duan, Feifei Li, Ryan E Rhodes, Xiang Wang, Dehiwala Liyanage Ishanka Harshani Kusum Peiris, Lin Zhou, Borui Shang, Yide Yang, Julien S Baker, Jiao Jiao, Wei Han
Annals of Behavioral Medicine.2022; 56(11): 1174. CrossRef
- ISO 50001 based energy management system: a bibliometric perspective
Original Articles
- Factors influencing acceptance of the COVID-19 vaccine in Malaysia: a web-based survey
- June Fei Wen Lau, Yuan Liang Woon, Chin Tho Leong, Hoon Shien Teh
- Osong Public Health Res Perspect. 2021;12(6):361-373. Published online November 25, 2021
- DOI: https://doi.org/10.24171/j.phrp.2021.0085
- 13,415 View
- 513 Download
- 12 Web of Science
- 11 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Objectives
The coronavirus disease 2019 (COVID-19) pandemic has set a precedent for the fastest-produced vaccine as a result of global collaboration and outreach. This study explored Malaysians’ acceptance of the COVID-19 vaccine and its associated factors.
Methods
A cross-sectional anonymous web-based survey was disseminated to Malaysian adults aged ≥18 years old via social media platforms between July 10, 2020 and August 31, 2020.
Results
In the analysis of 4,164 complete responses, 93.2% of participants indicated that they would accept the COVID-19 vaccine if it was offered for free by the Malaysian government. The median out-of-pocket cost that participants were willing to pay for a COVID-19 vaccine was Malaysian ringgit (MYR) 100 (interquartile range [IQR], 100) if it was readily available and MYR 150 (IQR, 200) if the supply was limited. Respondents with a low likelihood of vaccine hesitancy had 13 times higher odds of accepting the COVID-19 vaccine (95% confidence interval [CI], 8.69 to 19.13). High perceived risk and severity were also associated with willingness to be vaccinated, with adjusted odds ratios of 2.22 (95% CI, 1.44 to 3.41) and 2.76 (95% CI, 1.87 to 4.09), respectively. Age and ethnicity were the only independent demographic characteristics that predicted vaccine uptake.
Conclusion
Public health strategies targeting perceived risk, perceived susceptibility and vaccine hesitancy could be effective in enhancing vaccine uptake. -
Citations
Citations to this article as recorded by- Awareness, knowledge, disease prevention practices, and immunization attitude of hepatitis E virus among food handlers in Klang Valley, Malaysia
Sakshaleni Rajendiran, Wong Li Ping, Yuvaneswary Veloo, Syahidiah Syed Abu Thahir
Human Vaccines & Immunotherapeutics.2024;[Epub] CrossRef - COVID-19 vaccine uptake and its determinants among teenagers and their parents in Zhejiang, China: An online cross-sectional study
Yu Huang, Qingqing Wu, Shuiyang Xu, Xiang Zhao, Lei Wang, Qiaohong Lv, Suxian Wu, Xuehai Zhang
Asian Pacific Journal of Tropical Medicine.2023; 16(4): 176. CrossRef - Factors influencing parents’ hesitancy to vaccinate their children aged 5–11 years old against COVID-19: results from a cross-sectional study in Malaysia
Roy Rillera Marzo, Ritankar Chakraborty, Shean Yih Soh, Hui Zhu Thew, Collins Chong, Ching Sin Siau, Khairuddin Bin Abdul Wahab, Indang Ariati Binti Ariffin, Shekhar Chauhan, Ken Brackstone, Bijaya Kumar Padhi, Petra Heidler
Frontiers in Public Health.2023;[Epub] CrossRef - A survey on Malaysian’s acceptance and perceptions towards COVID-19 booster dose
Suresh Rajakumar, Noorasyikin Shamsuddin, Mohammed Abdullah Alshawsh, Sutha Rajakumar, Hasniza Zaman Huri
Saudi Pharmaceutical Journal.2023; 31(11): 101797. CrossRef - Cross-sectional assessment of predictors for COVID-19 vaccine uptake: an online survey in Greece
Petros Galanis, Irene Vraka, Olga Siskou, Olympia Konstantakopoulou, Aglaia Katsiroumpa, Ioannis Moisoglou, Daphne Kaitelidou
Vacunas.2022; 23: S60. CrossRef - Key predictors of COVID-19 vaccine hesitancy in Malaysia: An integrated framework
Jason Wei Jian Ng, Santha Vaithilingam, Mahendhiran Nair, Li-Ann Hwang, Kamarul Imran Musa, Anat Gesser-Edelsburg
PLOS ONE.2022; 17(5): e0268926. CrossRef - Intention to receive a COVID-19 vaccine booster dose and associated factors in Malaysia
Li Ping Wong, Haridah Alias, Yan-Li Siaw, Mustakiza Muslimin, Lee Lee Lai, Yulan Lin, Zhijian Hu
Human Vaccines & Immunotherapeutics.2022;[Epub] CrossRef - Determinants of COVID-19 vaccine acceptance in Ethiopia: A systematic review and meta-analysis
Ayenew Mose, Abebaw Wasie, Solomon Shitu, Kassahun Haile, Abebe Timerga, Tamirat Melis, Tadesse Sahle, Amare Zewdie, Dong Keon Yon
PLOS ONE.2022; 17(6): e0269273. CrossRef - When do persuasive messages on vaccine safety steer COVID-19 vaccine acceptance and recommendations? Behavioural insights from a randomised controlled experiment in Malaysia
Nicholas Yee Liang Hing, Yuan Liang Woon, Yew Kong Lee, Hyung Joon Kim, Nurhyikmah M Lothfi, Elizabeth Wong, Komathi Perialathan, Nor Haryati Ahmad Sanusi, Affendi Isa, Chin Tho Leong, Joan Costa-Font
BMJ Global Health.2022; 7(7): e009250. CrossRef - COVID-19 vaccine acceptance rate and its predictors in Ethiopia: A systematic review and meta-analysis
Getaneh Mulualem Belay, Tewodros Getaneh Alemu, Masresha Asmare Techane, Chalachew Adugna Wubneh, Nega Tezera Assimamaw, Tadesse Tarik Tamir, Addis Bilal Muhye, Destaye Guadie Kassie, Amare Wondim, Bewuketu Terefe, Bethlehem Tigabu Tarekegn, Mohammed Seid
Human Vaccines & Immunotherapeutics.2022;[Epub] CrossRef - Cross-sectional assessment of predictors for COVID-19 vaccine uptake: an online survey in Greece
Petros Galanis, Irene Vraka, Olga Siskou, Olympia Konstantakopoulou, Aglaia Katsiroumpa, Ioannis Moisoglou, Daphne Kaitelidou
Vacunas (English Edition).2022; 23: S60. CrossRef
- Awareness, knowledge, disease prevention practices, and immunization attitude of hepatitis E virus among food handlers in Klang Valley, Malaysia
- Prevalence and correlates of highly caffeinated beverage consumption among Korean adolescents
- Ho-Kyung Kwak, Jaesin Sa, Siyoung Choe, Jean-Philippe Chaput, Joon Chung, Gayle Cummings, Jounghee Lee
- Osong Public Health Res Perspect. 2021;12(6):374-384. Published online November 23, 2021
- DOI: https://doi.org/10.24171/j.phrp.2021.0013
- 10,148 View
- 94 Download
- 1 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Objectives
The purposes of this study were to (1) examine the multi-year prevalence of highly caffeinated beverage (HCB) consumption, (2) identify sex differences in the prevalence, and (3) investigate relationships between HCB consumption and behavioral characteristics in a nationally representative sample of Korean adolescents.
Methods
Data from the Korea Youth Risk Behavior Web-based Survey (2014–2017) were analyzed.
Results
HCB consumption was higher in 2017 than 2014 (23.9% vs. 12.0%), and higher among boys than girls (17.2% vs. 13.1%). HCB drinkers were more likely to (1) be boys, (2) be overweight or obese, (3) use alcohol and tobacco, (4) consume soda at least once per week, (5) consume sweetened beverages at least once per week, (6) have seriously considered suicide during the past 12 months, and (7) have attempted suicide during the past 12 months (p<0.05 for all).
Conclusion
Effective programs to curb HCB consumption among Korean adolescents need to be established. -
Citations
Citations to this article as recorded by- Secondary School Students and Caffeine: Consumption Habits, Motivations, and Experiences
Sophie Turner, Ajmol Ali, Carol Wham, Kay Rutherfurd-Markwick
Nutrients.2023; 15(4): 1011. CrossRef
- Secondary School Students and Caffeine: Consumption Habits, Motivations, and Experiences
- Laboratory investigations of herpes simplex virus-1 and -2 clinical samples in Korea
- Eun Ju Oh, Young Sam Yuk, Jae Kyung Kim
- Osong Public Health Res Perspect. 2021;12(6):385-389. Published online December 1, 2021
- DOI: https://doi.org/10.24171/j.phrp.2021.0146
- 5,812 View
- 83 Download
-
 Abstract
Abstract
 PDF
PDF - Objectives
Herpes simplex virus (HSV) infections have been reported in 60% to 95% of the adult population worldwide, making them one of the most common infectious conditions globally. HSV-1 and HSV-2 cause severe disease in immunocompromised patients. Therefore, the aim of this study was to provide information that could be used to reduce the incidence of genital herpes caused by HSV-1 and HSV-2.
Methods
From September 2018 to December 2020, 59,381 specimens were collected from outpatients across primary and secondary hospitals in Korea who requested U2Bio (Seoul, Korea) to conduct molecular biological testing of their samples for sexually transmitted infections. In this study, the positivity rates of HSV-1 and HSV-2 were analyzed according to age, sex, and specimen type.
Results
In the age-specific analysis of HSV-1, the highest positivity rate (0.58%) was observed in patients under 19 years of age, whereas the lowest positivity rate (0.08%) was observed in patients aged over 70 years. In the age-specific analysis of HSV-2, the highest positivity rate (2.53%) was likewise observed in patients under 19 years of age.
Conclusion
Our study identified differences in the infection rates of HSV-1 and HSV-2 depending on patients’ sex and age. These differences will be useful for improving disease prevention and control measures for HSV-1 and HSV-2.
- Prevalence of plasmid-mediated AmpC β-lactamases among uropathogenic Escherichia coli isolates in southwestern Iran
- Nabi Jomehzadeh, Khadijeh Ahmadi, Zahra Rahmani
- Osong Public Health Res Perspect. 2021;12(6):390-395. Published online December 1, 2021
- DOI: https://doi.org/10.24171/j.phrp.2021.0272
- 4,968 View
- 92 Download
- 5 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF - Objectives
This study was undertaken to evaluate AmpC β-lactamase-producing Escherichia coli urine isolates and to characterize the frequency of plasmid-mediated AmpC (pAmpC)-encoding genes.
Methods
Antimicrobial susceptibility tests were performed using the disk diffusion technique. AmpC β-lactamase production was assessed with a phenotypic inhibitor-based method. The presence of 6 pAmpC-encoding cluster genes was detected by multiplex polymerase chain reaction (PCR).
Results
The proportion of antibiotic resistance of E. coli isolates ranged from 7.4% to 90.5%, and more than half (51.6%) of the total isolates were multidrug-resistant (MDR). Among the 95 E. coli isolates, 60 (63.2%) were found to be cefoxitin-resistant, but only 14 (14.7%) isolates were confirmed as AmpC β-lactamase-producers. In the PCR assay, pAmpC-encoding genes were found in 15 (15.8%) isolates, and blaDHA was the most prevalent type. However, blaFOX, blaMOX, and blaACC genes were not detected in the isolates.
Conclusion
Our findings contributed valuable information concerning antibiotic resistance, confirmatory phenotypic testing for AmpC production, and pAmpC β-lactamase gene content in E. coli isolates in southwestern Iran. The level of MDR recorded in AmpC-producing strains of this study was worrying; therefore, implementing strong infection control approaches to reduce the MDR burden is recommended. -
Citations
Citations to this article as recorded by- A review of the mechanisms that confer antibiotic resistance in pathotypes of E. coli
Sina Nasrollahian, Jay P. Graham, Mehrdad Halaji
Frontiers in Cellular and Infection Microbiology.2024;[Epub] CrossRef - Association Between Uropathogenic Escherichia coli Virulence Genes and Severity of Infection and Resistance to Antibiotics
Sofía Alejandra Fonseca-Martínez, Ruth Aralí Martínez-Vega, Ana Elvira Farfán-García, Clara Isabel González Rugeles, Libeth Yajaira Criado-Guerrero
Infection and Drug Resistance.2023; Volume 16: 3707. CrossRef - Extended-spectrum β-lactamases producing Enterobacteriaceae (ESBL-PE) prevalence in Nepal: A systematic review and meta-analysis
Christina Khadka, Manita Shyaula, Gopiram Syangtan, Shrijana Bista, Reshma Tuladhar, Anjana Singh, Dev Raj Joshi, Lok R. Pokhrel, Prabin Dawadi
Science of The Total Environment.2023; 901: 166164. CrossRef - Prevalence of Extended-Spectrum β-Lactamase-Resistant Genes in Escherichia coli Isolates from Central China during 2016–2019
Zui Wang, Qin Lu, Xiaohui Mao, Li Li, Junfeng Dou, Qigai He, Huabin Shao, Qingping Luo
Animals.2022; 12(22): 3191. CrossRef - Molecular detection and characterization of Shigella spp. harboring extended-spectrum β-lactamase genes in children with diarrhea in northwest Iran
Sahar Sabour, Amir Teimourpour, Jafar Mohammadshahi, Hadi Peeridogaheh, Roghayeh Teimourpour, Taher Azimi, Zahra Hosseinali
Molecular and Cellular Pediatrics.2022;[Epub] CrossRef - Plasmid-mediated AmpC β-Lactamase gene analysis in Klebsiella Pneumoniae clinical isolates
Nabi Jomehzadeh, Khadijeh Ahmadi, Hasti Shaabaninejad, Gholamali Eslami
Biomedical and Biotechnology Research Journal (BBR.2022; 6(4): 582. CrossRef
- A review of the mechanisms that confer antibiotic resistance in pathotypes of E. coli
Brief Report
- COVID-19 vaccine safety monitoring in Republic of Korea from February 26, 2021 to October 31, 2021
- Insob Hwang, Kyeongeun Park, Tae Eun Kim, Yunhyung Kwon, Yeon-Kyeng Lee
- Osong Public Health Res Perspect. 2021;12(6):396-402. Published online December 21, 2021
- DOI: https://doi.org/10.24171/j.phrp.2021.0310
- 7,201 View
- 191 Download
- 13 Web of Science
- 11 Crossref
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material 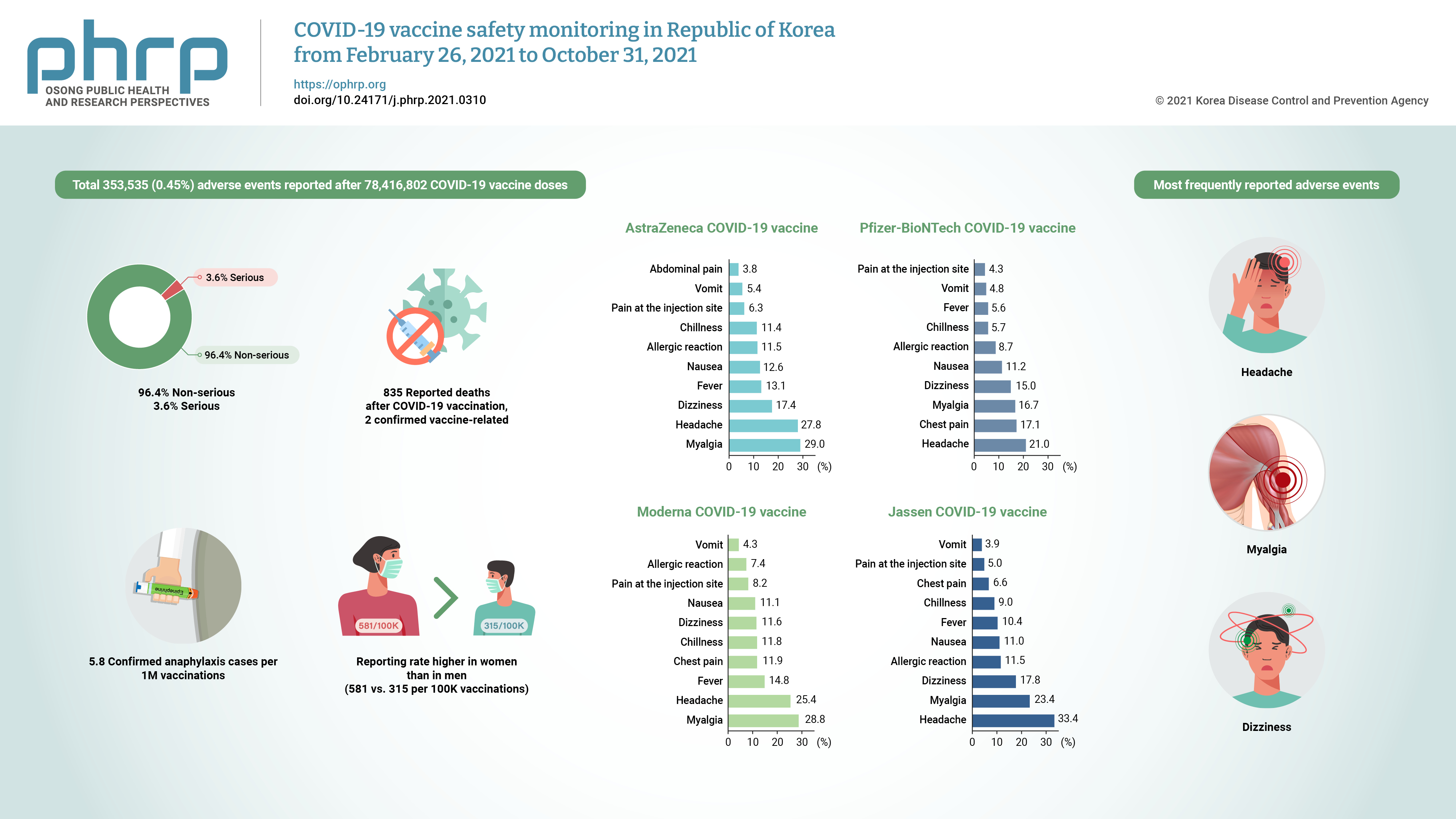
- Objectives
This study aimed to present data on reported adverse events following coronavirus disease 2019 (COVID-19) vaccination in Republic of Korea from February 26 to October 31, 2021, and to determine whether any significant patterns emerged from an analysis of the characteristics of suspected adverse event cases for each type of vaccine.
Methods
Adverse events following COVID-19 vaccination reported by medical doctors and forensic pathologists were analyzed. Cases of suspected anaphylaxis were classified using the Brighton Collaboration definition.
Results
By October 31, 2021, a total of 353,535 (0.45%) adverse events were reported after 78,416,802 COVID-19 vaccine doses. Of the adverse events, 96.4% were non-serious and 3.6% were serious. The most frequently reported adverse events were headache, myalgia, and dizziness. Of the 835 reported deaths after COVID-19 vaccination, 2 vaccine-related deaths were confirmed. Suspected anaphylaxis was confirmed in 454 cases using the Brighton Collaboration definition.
Conclusion
The commonly reported symptoms were similar to those described in clinical trials. Most reported adverse events were non-serious, and the reporting rate of adverse events following COVID-19 vaccination was higher in women than in men (581 vs. 315 per 100,000 vaccinations). Confirmed anaphylaxis was reported in 5.8 cases per 1,000,000 vaccinations. -
Citations
Citations to this article as recorded by- A Nationwide Survey of mRNA COVID-19 Vaccinee’s Experiences on Adverse Events and Its Associated Factors
Dongwon Yoon, Ha-Lim Jeon, Yunha Noh, Young June Choe, Seung-Ah Choe, Jaehun Jung, Ju-Young Shin
Journal of Korean Medical Science.2023;[Epub] CrossRef - Temporal association between the age-specific incidence of Guillain-Barré syndrome and SARS-CoV-2 vaccination in Republic of Korea: a nationwide time-series correlation study
Hyunju Lee, Donghyok Kwon, Seoncheol Park, Seung Ri Park, Darda Chung, Jongmok Ha
Osong Public Health and Research Perspectives.2023; 14(3): 224. CrossRef - Safety monitoring of COVID-19 vaccines: February 26, 2021, To June 4, 2022, Republic of Korea
Yeon-Kyeng Lee, Yunhyung Kwon, Yesul Heo, Eun Kyoung Kim, Seung Yun Kim, Hoon Cho, Seontae Kim, Mijeong Ko, Dosang Lim, Soon-Young Seo, Enhi Cho
Clinical and Experimental Pediatrics.2023; 66(10): 415. CrossRef - Allergic Reactions to COVID-19 Vaccines: Risk Factors, Frequency, Mechanisms and Management
Nicoletta Luxi, Alexia Giovanazzi, Alessandra Arcolaci, Patrizia Bonadonna, Maria Angiola Crivellaro, Paola Maria Cutroneo, Carmen Ferrajolo, Fabiana Furci, Lucia Guidolin, Ugo Moretti, Elisa Olivieri, Giuliana Petrelli, Giovanna Zanoni, Gianenrico Senna,
BioDrugs.2022; 36(4): 443. CrossRef - Safety monitoring of COVID-19 vaccination among adolescents aged 12 to 17 years old in the Republic of Korea
Seontae Kim, Insob Hwang, Mijeong Ko, Yunhyung Kwon, Yeon-Kyeng Lee
Osong Public Health and Research Perspectives.2022; 13(3): 230. CrossRef - Incidence and Characteristics of Adverse Events after COVID-19 Vaccination in a Population-Based Programme
Laura Bonzano, Olivera Djuric, Pamela Mancuso, Lidia Fares, Raffaele Brancaccio, Marta Ottone, Eufemia Bisaccia, Massimo Vicentini, Alessia Cocconcelli, Alfonso Motolese, Rostyslav Boyko, Paolo Giorgi Rossi, Alberico Motolese
Vaccines.2022; 10(7): 1111. CrossRef - Global Predictors of COVID-19 Vaccine Hesitancy: A Systematic Review
Carla Pires
Vaccines.2022; 10(8): 1349. CrossRef - Anaphylaxis and Related Events Following COVID‐19 Vaccination: A Systematic Review
Pradipta Paul, Emmad Janjua, Mai AlSubaie, Vinutha Ramadorai, Beshr Mushannen, Ahamed Lazim Vattoth, Wafa Khan, Khalifa Bshesh, Areej Nauman, Ibrahim Mohammed, Imane Bouhali, Mohammed Khalid, Dalia Zakaria
The Journal of Clinical Pharmacology.2022; 62(11): 1335. CrossRef - Adverse events of the Pfizer-BioNTech COVID-19 vaccine in Korean children and adolescents aged 5 to 17 years
Seontae Kim, Yeseul Heo, Soon-Young Seo, Do Sang Lim, Enhi Cho, Yeon-Kyeng Lee
Osong Public Health and Research Perspectives.2022; 13(5): 382. CrossRef - COVID-19 Vaccination in Korea: Past, Present, and the Way Forward
Eliel Nham, Joon Young Song, Ji Yun Noh, Hee Jin Cheong, Woo Joo Kim
Journal of Korean Medical Science.2022;[Epub] CrossRef - Self-reported adverse events after 2 doses of COVID-19 vaccine in Korea
Yunhyung Kwon, Insob Hwang, Mijeong Ko, Hyungjun Kim, Seontae Kim, Soon-Young Seo, Enhi Cho, Yeon-Kyeng Lee
Epidemiology and Health.2022; 45: e2023006. CrossRef
- A Nationwide Survey of mRNA COVID-19 Vaccinee’s Experiences on Adverse Events and Its Associated Factors





 First
First Prev
Prev


