Articles
- Page Path
- HOME > Osong Public Health Res Perspect > Volume 12(5); 2021 > Article
-
Original Article
Effects of activities of daily living-based dual-task training on upper extremity function, cognitive function, and quality of life in stroke patients -
Hee-Su An1
 , Deok-Ju Kim2
, Deok-Ju Kim2
-
Osong Public Health and Research Perspectives 2021;12(5):304-313.
DOI: https://doi.org/10.24171/j.phrp.2021.0177
Published online: September 13, 2021
1Department of Occupational Therapy, Hana General Hospital, Cheongju, Korea
2Department of Occupational Therapy, College of Health and Medical Sciences, Cheongju University, Cheongju, Korea
- Corresponding author: Deok-Ju Kim Department of Occupational Therapy, College of Health and Medical Sciences, Cheongju University, 298 Daeseong-ro, Cheongwon-gu, Cheongju 28503, Korea E-mail: dj7407@hanmail.net
- This paper was written by revising and supplementing the first author’s master’s thesis.
© 2021 Korea Disease Control and Prevention Agency
This is an open access article under the CC BY-NC-ND license (http://creativecommons.org/licenses/by-nc-nd/4.0/).
Abstract
-
Objectives
- The aim of this study was to investigate the effect of daily living dual-task training focused on improving attention and executive function of the upper extremities, cognitive function, and quality of life in stroke patients.
-
Methods
- We included 30 stroke patients who were hospitalized between July 2020 and October 2020. They were divided into experimental and control groups through randomization. The experimental group performed 20 minutes of dual-task training and received 10 minutes of conventional occupational therapy, while the control group performed 20 minutes of single-task training and received 10 minutes of conventional occupational therapy. Both groups underwent their respective rehabilitation for 30 minutes per session, 5 times per week for 5 weeks.
-
Results
- Both groups showed significant improvements in upper extremity function, cognitive function, and quality of life; the experimental group showed higher results for all items. A significant between-group difference was observed in the magnitude of the changes.
-
Conclusion
- In stroke patients, dual-task training that combined attention and executive function with daily living activities was found to be meaningful, as it encouraged active participation and motivation. This study is expected to be used as a foundation for future interventions for stroke patients.
- Stroke is a cerebrovascular disease in which a blood vessel supplying the brain is ruptured or blocked, resulting in complex dysfunction and neurological function impairment following brain damage [1,2]. The type and level of the disorder are determined based on the area and extent of brain damage [2]. Common major dysfunctions after stroke include motor disorders, upper extremity dysfunction, cognitive disorders, emotional disorders, and speech disorders [3,4]. In particular, upper extremity dysfunction and cognitive impairment cause many difficulties in achieving successful rehabilitation [5].
- In the field of occupational therapy, improving the function of the injured upper extremities has been regarded as one of the most important goals, as impaired upper extremity function limits independent performance in daily life [6–8]. Among stroke patients, 16% to 30% show deficits in cognitive functions such as orientation, attention, memory, language ability, executive function, and spatiotemporal cognition within 1 year [9]. Stroke patients with cognitive impairment experience difficulties in processing meaningful stimuli from the environment, making it difficult for them to self-structure and organize their environment [10]. Specifically, impaired attention and executive function have been reported as factors that negatively affect the patient’s return to society, in addition to resulting in serious deterioration of the ability to perform daily activities, such as academic tasks and leisure activities [11].
- Attention is the ability to elicit an efficient behavioral response by accepting and selecting external stimuli from the surrounding environment [12,13]. Attention constitutes the first step of the brain’s information processing process; thus, problems in maintaining proper attention result in difficulty in the execution of other cognitive functions [14,15]. Executive function is a comprehensive concept that integrates processes related to purposeful and goal-directed behavior, and it involves initiation, planning, sequencing, control and suppression of impulses, thinking flexibility, problem-solving, abstract thinking, organization, and social judgment [16–18]. The frontal lobe of the brain is responsible for executive function. In particular, neural networks in the prefrontal cortex are involved in learning, which plays an essential role in recovery and rehabilitation after brain injury. These networks are, therefore, the main target for effective rehabilitation [19,20]. If executive function is impaired, the ability to perform complex daily life activities decreases, negatively affecting social communication and thereby reducing social participation [21,22].
- The objective of rehabilitation treatment is to allow stroke patients to live independent daily lives by recovering maximum residual function after injury [23]. Thus, if rehabilitation programs for stroke patients include training focused on attention and executive function, more efficient improvement in performing daily life activities can be expected [24]. A variety of effective training methods for stroke patients have been suggested. In particular, dual-task training involving the simultaneous execution of cognitive tasks and motor tasks in relation to the recovery of motor control in patients with neurological impairment (e.g., stroke) has been implemented in clinical settings [25]. In dual-task training, the patient performs 2 or more complex tasks of different characteristics that frequently occur in everyday life [26,27]. The objective of dual-task training is to improve the subject’s ability to process information by performing 2 different tasks simultaneously [28]. Most daily life movements involve performing 2 motor tasks simultaneously, and performing various daily life activities involves the concurrent execution of high-level cognitive function and motor tasks [29,30]. However, despite the high frequency of dual tasks in daily life, rehabilitation of stroke patients is mainly performed under single-task conditions [31]. Because a training method that focuses on a single task does not reflect the complex activities of daily life, it has been reported that recovering fragmentary functions such as upper extremity function and balance alone does not significantly change the level at which individuals perform daily life activities [32]. Therefore, it is necessary to actively utilize dual-task training in which 2 or more different tasks are simultaneously handled in order to improve stroke patients’ performance of daily activities [28].
- Most existing studies conducted with stroke patients have involved the simultaneous performance of balance or gait training with upper extremity training or cognitive tasks, and many cases demonstrated positive effects of training [33–35]. Only a handful of studies on dual-task training have applied daily life activities and upper extremity movements together with cognitive tasks for stroke patients. Therefore, this study aimed to examine the effects of repeated dual-task training coupling daily life activities with attention and executive function on upper extremity function, cognitive function, and quality of life in stroke patients.
Introduction
- Participants
- This study was conducted among 30 subjects who met the selection criteria among patients who were hospitalized after being diagnosed with stroke based on magnetic resonance imaging or computed tomography scans taken at the H hospital in Cheongju between July 2020 and October 2020. The specific inclusion criteria were as follows: (1) those with disease onset within the past 6 months, (2) those who scored at least 20 points on the Korean version of the Mini-Mental State Examination (K-MMSE) and were able to follow the researcher’s instructions, (3) those in Brunnstrom Recovery Stage (BRS) 3 or higher, and (4) those who had no issues in communication or problems with vision or hearing and could follow instructions.
- Protocol
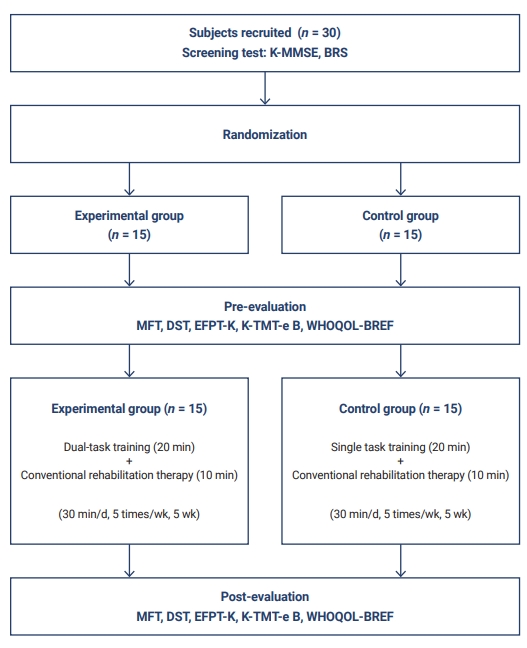
- The study period was from July 2020 to October 2020. The 30 subjects who met the inclusion criteria were randomized into experimental and control groups. The experimental group performed dual tasks for 20 minutes in the treatment room and received 10 minutes of conventional occupational therapy for a total of 30 minutes per session, 5 times a week for 5 weeks. The control group performed a single task for 20 minutes and received 10 minutes of conventional occupational therapy, for a total of 30 minutes per session, 5 times a week for 5 weeks. The dual tasks combined attention or executive function with daily life activities, whereas the single tasks consisted of sensory stimulation training on the paralyzed side, upper extremity muscle strength training, cognitive and perceptual training, and fine hand movement using tools. Occupational therapists with more than 4 years of experience conducted the evaluation (pre-assessment, intervention, and post-assessment, in sequential order). The design of this study is presented in Figure 1.
- Outcome Measurements
- The Manual Function Test (MFT) is widely used for the measurement of upper extremity function and motor ability in the early-stage rehabilitation of stroke patients [36]. Measurements are made on both the paralyzed and the non-paralyzed sides, with a total of 8 items in the areas of upper extremity movement (4 items), grip strength (2 items), and finger manipulation (2 items). For each sub-test that can be performed, a score of 1 is assigned up to a total of 32 points, and 0 is assigned for sub-tests that could not be performed. The MFT score is calculated by converting the initial score out of 32 points to a score out of 100 by multiplying it by 3.125. The test-retest concordance was 0.99 for the paralyzed side and 0.83 for the non-paralyzed side [37,38].
- The Digit Span Test (DST) consists of the DST-Forward and DST-Backward. The DST-Forward starts with 3 digits to repeat with 1 additional digit to memorize at each stage, for a total of 9 digits to memorize and repeat at the last stage. A higher number of digits indicates a higher level of attention. In the DST-Backward, the test is conducted in the same manner for scoring, and a higher number of digits indicates better working memory. The reliability was found to be 0.72 for the DST-Forward and 0.57 for the DST-Backward [39].
- Executive Function Performance Test Korean version (EFPT-K) evaluates executive function and instrumental daily life performance by measuring the degree of impairment of executive function, individual competence in independent function, and the level of assistance to complete tasks. For each task, points are given for elements of executive function such as initiation, preparation, ordering, judgment and safety, and termination, and each element is given a minimum of 0 points and a maximum of 5 points. The total score is scored from 0 to 100 points, and a lower score indicates a higher level of independence. The inter-tester reliability was 0.91 and the internal consistency was found to be high (0.94) [40].
- To measure the improvement in the speed of cognitive processing, the Korean version of the Trail Making Test for the Elderly B (K-TMT-e B) was conducted. Cognitive processing and executive function are measured through visual concept tracking and visual movement tracking. There are 2 types of the test (type A and B); however, only type B, which reflects attention movement and retrograde suppression, was used to determine cognitive processing speed. The instructions for the test are to connect items composed of numbers and alphabetical letters in alternating order. The frequency and type of errors are not separately recorded, but the instructions state that the test should be stopped if it takes more than 5 minutes [26,27]. The test-retest reliability of the K-TMT-e B was found to be relatively high (0.89) [41].
- Quality of life was measured using the World Health Organization Quality of Life-BREF (WHOQOL-BREF). The WHOQOL-BREF is divided into 4 subscales (physical health, psychology, social relations, and environment) and consists of a total of 26 items. It is measured on a 5-point scale (1 to 5 points), and higher scores indicate higher quality of life. The test-retest reliability ranged from 0.43 to 0.73, and the value of Cronbach’s alpha, which indicates the degree of internal consistency, was found to be 0.89 [42].
- Intervention
- The dual-task training used in this study was designed based on previous studies [43,44] that examined training for attention and daily life activities for stroke patients, as well as the study by Park et al. [45], which conducted interventions for executive function in stroke patients. Attention training consisted of continuous subtraction, simple addition or subtraction, counting the numbers 1 to 20 forward or backward in order, reading words backwards, and a simple word game of coming up with a word that starts with the last letter of the previous word. Daily living-based activities included climbing the stairs, making tea or coffee, folding tops or bottoms, buttoning and unbuttoning, and moving beans. The activities for executive function consisted of presenting a virtual situation, explaining the order of wearing clothes, describing a daily routine, making a shopping list, and talking about categorization types. The activities of executive function were composed of items related to daily life activities. Because executive function is a high-level cognitive domain, it can cause confusion in patients with brain damage when performing the dual task of applying items that require higher-order thinking and daily life activities together. Therefore, for example, when “buttoning and unbuttoning” is performed as a daily activity, the corresponding item of the executive function would be “explaining the order of wearing clothes.” Dual-task training was conducted by combining the aforementioned executive function and daily life activities (Table 1, Table S1).
- Statistical Analysis
- The statistical analysis was conducted using IBM SPSS ver. 24.0 (IBM Corp., Armonk, NY, USA). The normality of the distribution of data across the study subjects was determined using the Shapiro-Wilk test, and if normality could not be established, a nonparametric analysis was conducted. Among general characteristics, sex, stroke type, and the paralyzed side were analyzed using the chi-square and Mann-Whitney U-tests to test the homogeneity of the subjects before the intervention. Changes after the intervention within the experimental and the control groups were analyzed using the Wilcoxon signed rank test, whereas between-group differences before and after the intervention were analyzed using the Mann-Whitney U-test. The statistical significance level for all data was set to 0.05.
Materials and Methods
Manual Function Test
The Digit Span Test
Executive Function Performance Test Korean version
Korean version of the Trail Making Test for the Elderly B
World Health Organization Quality of Life-BREF
- General Characteristics of Research Subjects
- The general characteristics of the subjects who participated in the study are presented in Table 2. There were 8 male (53.3%) and 7 female patients (46.7%) in the experimental group, and 7 male (46.7%) and 8 female patients (53.3%) in the control group. The mean age was 65.20±12.17 years in the experimental group and 65.27±12.73 years in the control group. The right and left sides were paralyzed in 6 (40.0%) and 9 patients (60.0%), respectively, in the experimental group, and the right side was paralyzed in 7 patients (46.7%) and the left side was paralyzed in 8 (53.3%) in the control group. The mean duration of disease was 4.07±0.88 months in the experimental group and 4.20±0.77 months in the control group. There were no significant differences in sex, age, the paralyzed side, disease duration, K-MMSE scores, and BRS between the 2 groups (p>0.05).
- Comparison of the MFT Results Before and After the Intervention
- Table 3 shows the post-intervention changes in upper extremity function in the experimental and the control groups. MFT measures both the affected and unaffected sides, but in this study, only the affected side was measured and reflected in the results. In the experimental group, all of the MFT items showed statistically significant improvements after the intervention (p<0.05, p<0.01). Similarly, the control group showed statistically significant improvements in all items after the intervention (p<0.05, p<0.01). Significant differences between the 2 groups were found in the changes in upper extremity function for all items, excluding the item for upper extremity movement (p<0.05).
- Comparison of the DST, EFPT-K, and K-TMT-e B Results Before and After the Intervention
- The results for changes in cognitive function before and after the intervention in the experimental and control groups are presented in Table 4. The experimental group showed statistically significant improvements in both the DST-Forward and DST-Backward after the intervention (p<0.01). The control group also showed significant improvements in all items after the intervention (p<0.05, p<0.01). Statistically significant improvements were seen for all items in the EFPT-K in both the experimental and the control groups (p<0.01). For the K-TMT-e B, there was a statistically significant reduction in the time taken for completion after the intervention in both the experimental and the control groups (p<0.01). On the cognitive function assessment, the experimental group showed slightly higher scores than the control group for all of the items, and there was a significant difference when the changes between the groups were compared (p<0.01).
- Comparison of the WHOQOL-BREF Results Before and After the Intervention
- Table 5 shows the results for changes in the WHOQOL-BREF quality of life scale after the intervention for the experimental and the control groups. Statistically significant improvements were found for all items in both the experimental and the control groups after the intervention (p<0.01), and there was a significant difference in the change in the quality of life between the 2 groups (p<0.01).
Results
- Dual-task training involves performing 2 or more complex tasks with different characteristics that frequently occur in daily life. The training requires performing 1 additional task while performing 1 basic task, or performing 2 or more tasks simultaneously [26,27]. To carry out functional movements in daily life, it is necessary to be able to perform multiple tasks at once [46–48]. According to previous studies on stroke, dual-task training was more effective in improving the subject's information processing ability than performing only 1 task at a time for the same amount of time [28]. However, most studies have used upper extremity functions together for balance and gait training, or have dealt with cognitive tasks for balance and gait training [30,31,33,34]. Therefore, in this study, we devised a dual task in which a cognitive task including attention and executive function was combined with daily living-based activities, and the effect of this activity on stroke patients was investigated. Dual-task activities were generated based on previous studies [43–45]. In each session, dual-task training appropriately integrated attention and executive function tasks with daily living activities.
- The results revealed that both the experimental group, which performed daily life-based dual-task training, and the control group, which performed single-task training, showed improvements in upper extremity function after the intervention. A study by Kim et al. [49], investigated the effects of a dual task in which the experimental group moved the upper extremity of the paralyzed side while standing, and the results showed improvement in upper extremity function on the paralyzed side. In a study by Jang et al. [50], significant improvements were observed in functional movement of the upper extremity after performing tasks in dual-task and single-task groups, suggesting that upper extremity function can be improved with single-task training and conventional occupational therapy. Similarly, the improvement in upper extremity function in both groups of this study may have been due to the activities that heavily involved the upper extremity, such as sensory stimulation of the affected side and upper extremity movement using the affected side, in the daily life-based single and dual tasks.
- When changes in cognitive function after the intervention in the experimental and the control groups were examined, significant improvements were observed for both groups in the DST, which assessed attention, the EFPT-K, which tested executive function, and the K-TMT-e B. However, an analysis of between-group differences showed that the change was significantly greater in the experimental group than in the control group. Kim and Kim [51] conducted concurrent motor tasks, such as ball throwing, clapping, and elastic bands, with cognitive tasks, including matching picture cards, finding vocabulary, and calculations in the experimental group, and showed a significant improvement in executive function compared to the control group, which performed single motor or cognitive tasks; this was consistent with the results of the present study. The results of the K-TMT-e B test used in this study showed a statistically significant reduction in the time taken for completion in the experimental group compared to the control group. The study by Mirelman et al. [52] reported that cognitive processing speed improved when motor function improved, while Han [44] reported an improvement in high-dimensional cognitive function as a result of activation of the cerebral cortex during dual-task training involving cognitive tasks. In this study, daily life activity training was consistently performed in addition to cognitive tasks that focused on attention and executive function, and the improved motor function is thought to have exerted a positive effect on cognitive processing speed. This combination of daily living and cognitive activities could have had a greater effect on the improvement of cognitive function in the experimental group.
- When changes in the quality of life in the experimental and the control groups were examined, both the experimental group, which performed dual tasks, and the control group, which performed single tasks and received conventional occupational therapy, showed significant improvements in quality of life. In a study by Meester et al. [53], the experimental group was asked to perform dual tasks in which cognitive tasks were carried out or daily life activities were explained while on the treadmill, and the control group was asked to perform a single task on the treadmill. When quality of life was measured, both groups showed an improvement in confidence in their quality of life, but the quality of life in the experimental group was significantly higher. Similarly, in this study, the magnitude of the improvement after the intervention was significantly higher in the experimental group than in the control group. This seems to suggest that dual tasks have a greater effect on quality of life in stroke patients than single tasks, which is in line with the results of previous studies.
- Although we were able to demonstrate that dual-task training involving daily living activities with a focus on attention and executive function can have positive effects on upper extremity function, cognitive function, and the quality of life in stroke patients, there are several limitations of this study. First, the results are difficult to generalize as there was only a small number of subjects. Second, the dual tasks could not be presented in accordance with individual competency. Third, follow-up tests were not performed, which could have identified continuing effects of the intervention. To supplement these limitations, additional research should be conducted with more subjects and with a comparison of the effects between the groups based on the individual competency of the subjects, as the impact of dual-task training may vary depending on individual competency [54]. Despite these limitations, this study has clinical significance in that executive function training was implemented in addition to attention in the cognitive function tasks, and that the study elicited active participation and motivation from the subjects since the daily living activities consisted of familiar activities.
Discussion
- This study demonstrated that dual-task training that focused on attention and executive function combined with daily living activities had a positive effect on upper extremity function, cognitive function, and the quality of life in stroke patients. This dual-task training represents a new method to help stroke patients return to their daily routines, and it is expected to be used as a foundation for the treatment of stroke patients in the future.
Conclusion
-
Ethics Approval
This study was approved by the Institutional Review Board (IRB) from the Cheongju University (IRB No: 1041107-202006-HR-031-01). Written informed consent was obtained from the subject before the intervention.
-
Conflicts of Interest
The authors have no conflicts of interest to declare.
-
Funding
None.
-
Availability of Data
The datasets are not publicly available but are available from the corresponding author upon reasonable request.
-
Additional Contributions
The authors would like to express their appreciation to all the participants and their families for their cooperation and participation in this study.
Article information
Supplementary Material
Flow chart of the study.
| Variable |
Intervention with groups |
Difference between groups |
|||||
|---|---|---|---|---|---|---|---|
| Before (mean±SD) | After (mean±SD) | Z | p | Mean±SD | Z | p | |
| Upper extremity training | |||||||
| EG | 14.40±1.35 | 15.53±0.74 | –2.724 | 0.006** | 1.13±1.18 | –0.932 | 0.351 |
| CG | 14.40±1.45 | 15.20±1.01 | –2.414 | 0.016* | 0.80±1.14 | ||
| Grip strength | |||||||
| EG | 5.33±0.48 | 5.87±0.35 | –2.530 | 0.011* | 0.67±0.48 | –2.159 | 0.031* |
| CG | 5.47±0.51 | 5.73±0.45 | –2.000 | 0.046* | 0.27±0.45 | ||
| Finger manipulation | |||||||
| EG | 4.60±0.91 | 6.20±1.08 | –3.520 | 0.000** | 1.60±0.50 | –2.361 | 0.018* |
| CG | 4.60±0.82 | 5.53±0.99 | –2.889 | 0.004** | 0.93±0.79 | ||
| Total score | |||||||
| EG | 24.53±1.99 | 27.73±1.58 | –3.438 | 0.001** | 3.20±1.52 | –2.430 | 0.015* |
| CG | 24.47±2.06 | 26.40±1.95 | –3.088 | 0.002** | 1.93±1.79 | ||
| Variable |
Intervention with groups |
Difference between groups |
|||||
|---|---|---|---|---|---|---|---|
| Before (mean±SD) | After (mean±SD) | Z | p | Mean±SD | Z | p | |
| DST-Forward | |||||||
| EG | 5.27±0.88 | 6.93±0.88 | –3.542 | 0.000** | 1.67±0.48 | –3.181 | 0.001** |
| CG | 5.20±1.08 | 6.07±1.10 | –3.127 | 0.002** | 0.87±0.64 | ||
| DST-Backward | |||||||
| EG | 2.60±0.73 | 3.93±0.45 | –3.397 | 0.001** | 1.33±0.61 | –3.500 | 0.000** |
| CG | 3.00±0.75 | 3.40±0.73 | –2.449 | 0.0141* | 0.40±0.50 | ||
| EFPT-K | |||||||
| EG | 12.70±2.51 | 9.96±1.30 | –3.413 | 0.001** | –2.74±1.29 | –4.720 | 0.000** |
| CG | 12.70±2.63 | 11.94±2.58 | –3.474 | 0.001** | –0.77±0.19 | ||
| K-TMT-e B | |||||||
| EG | 89.13±10.85 | 67.00±12.16 | –3.411 | 0.001** | –22.13±4.86 | –3.199 | 0.001** |
| CG | 89.60±12.33 | 77.00±13.26 | –3.412 | 0.001** | –12.60±7.83 | ||
| Variable |
Intervention with groups |
Difference between groups |
|||||
|---|---|---|---|---|---|---|---|
| Before (mean±SD) | After (mean±SD) | Z | p | Mean±SD | Z | p | |
| Physical health | |||||||
| EG | 19.47±3.50 | 26.00±2.59 | –3.391 | 0.001** | 6.53±2.61 | –3.158 | 0.002** |
| CG | 19.93±4.14 | 23.60±4.18 | –3.309 | 0.001** | 3.67±2.09 | ||
| Psychology | |||||||
| EG | 15.60±2.44 | 22.33±3.71 | –3.423 | 0.001** | 6.73±2.86 | –3.617 | 0.000** |
| CG | 15.60±2.92 | 18.47±4.08 | –3.196 | 0.001** | 2.87±1.88 | ||
| Social relations | |||||||
| EG | 8.73±2.21 | 10.87±1.99 | –3.455 | 0.001** | 2.13±0.99 | –3.094 | 0.002** |
| CG | 8.67±1.58 | 9.60±1.76 | –2.913 | 0.004** | 0.93±0.88 | ||
| Environment | |||||||
| EG | 23.53±2.64 | 27.93±3.15 | –3.428 | 0.001** | 4.40±1.95 | –3.524 | 0.000** |
| CG | 23.73±2.28 | 25.20±2.65 | –2.842 | 0.004** | 1.47±1.72 | ||
| Total score | |||||||
| EG | 68.13±8.55 | 86.73±9.52 | –3.411 | 0.001** | 18.60±4.05 | –3.596 | 0.000** |
| CG | 66.93±9.27 | 76.87±11.74 | –3.414 | 0.001** | 9.93±5.68 | ||
- 1. O'Sullivan SB, Schmitz TJ. Physical rehabilitation: assessment and treatment. 4th ed. Philadelpia: FA Davis; 2001.
- 2. Sullivan KJ, Brown DA, Klassen T, et al. Effects of task-specific locomotor and strength training in adults who were ambulatory after stroke: results of the STEPS randomized clinical trial. Phys Ther 2007;87:1580−602.ArticlePubMedPDF
- 3. Sohlberg MM, Mateer CA. Cognitive rehabilitation: an integrative neuropsychological approach. New York: Guilford Press; 2001.
- 4. Braun SM, Beurskens AJ, van Kroonenburgh SM, et al. Effects of mental practice embedded in daily therapy compared to therapy as usual in adult stroke patients in Dutch nursing homes: design of a randomized controlled trial. BMC Neurol 2007;7:34. PubMedPMC
- 5. Oros RI, Popescu CA, Iova CA, et al. The impact of cognitive impairment after stroke on activities of daily living. Hum Vet Med 2016;8:41−4.
- 6. Caliandro P, Celletti C, Padua L, et al. Focal muscle vibration in the treatment of upper limb spasticity: a pilot randomized controlled trial in patients with chronic stroke. Arch Phys Med Rehabil 2012;93:1656−61.ArticlePubMedPDF
- 7. Kwakkel G, Kollen BJ, van der Grond J, et al. Probability of regaining dexterity in the flaccid upper limb: impact of severity of paresis and time since onset in acute stroke. Stroke 2003;34:2181−6.ArticlePubMedPDF
- 8. Tavernese E, Paoloni M, Mangone M, et al. Segmental muscle vibration improves reaching movement in patients with chronic stroke: a randomized controlled trial. NeuroRehabilitation 2013;32:591−9.ArticlePubMedPDF
- 9. Appelros P, Andersson AG. Changes in Mini Mental State Examination score after stroke: lacunar infarction predicts cognitive decline. Eur J Neurol 2006;13:491−5.ArticlePubMedPDF
- 10. Shin MJ, Park JE, Kim DR, et al. The effect of computerized cognitive rehabilitation on cognitive function, activities of daily living and self-efficacy in brain injury patients. Korean J Rehabil 2015;4:5−23. Korean.
- 11. Kim EK. The effects of depression and cognitive functions on the degree of daily life performance in stroke patients [dissertation] Seoul, Seoul National University. 2006;Korean.
- 12. Kwon JS, Kim YG, Kim JY, et al. Cognitive rehabilitation of occupational therapist. Seoul: Pacific Books; 2008. Korean.
- 13. Van Zomeren AH, Brouwer WH. Clinical neuropsychology of attention. New York: Oxford University Press; 1994.
- 14. Ha KS, Kwon JS, Lyoo IK. Development and standardization of the computerized attention assessment for Korean adults. J Korean Neuropsychiatr Assoc 2002;41:335−46. Korean.
- 15. Jung HY, Kwon HK, Oh CH. The study on the initial evaluation in the beginning of rehabilitation and the functional outcome in stroke. J Korean Acad Rehabil Med 1991;15:398−404. Korean.
- 16. Baum CM, Connor LT, Morrison T, et al. Reliability, validity, and clinical utility of the Executive Function Performance Test: a measure of executive function in a sample of people with stroke. Am J Occup Ther 2008;62:446−55.ArticlePubMedPDF
- 17. Etnier JL, Chang YK. The effect of physical activity on executive function: a brief commentary on definitions, measurement issues, and the current state of the literature. J Sport Exerc Psychol 2009;31:469−83.ArticlePubMedPDF
- 18. Poulin V, Korner-Bitensky N, Dawson DR, et al. Efficacy of executive function interventions after stroke: a systematic review. Top Stroke Rehabil 2012;19:158−71.ArticlePubMedPDF
- 19. Chen AJ, Abrams GM, D’Esposito M. Functional reintegration of prefrontal neural networks for enhancing recovery after brain injury. J Head Trauma Rehabil 2006;21:107−18.ArticlePubMedPDF
- 20. Elliott R. Executive functions and their disorders. Br Med Bull 2003;65:49−59.ArticlePubMedPDF
- 21. Katz N, Hartman-Maeir A. Higher-level cognitive functions: awareness and executive functions enabling engagement in occupation. Washington (DC): American Psychological Association; 2011.
- 22. Lezak MD. The problem of assessing executive functions. Int J Psychol 1982;17:281−97.Article
- 23. Yagura H, Miyai I, Seike Y, et al. Benefit of inpatient multidisciplinary rehabilitation up to 1 year after stroke. Arch Phys Med Rehabil 2003;84:1687−91.ArticlePubMed
- 24. Kim JY. Analysis of cognitive factors affecting stroke patient's activity of daily living performance: using the computerized neurocognitive function test. J Korea Acad Ind Coop Soc 2011;12:5715−21.Article
- 25. Plummer-D’Amato P, Altmann LJ, Saracino D, et al. Interactions between cognitive tasks and gait after stroke: a dual task study. Gait Posture 2008;27:683−8.ArticlePubMedPMC
- 26. Lee YJ, Jung MY. A systematic review of the dual-task training for stroke with hemiplegia. Ther Sci Rehabil 2016;5:23−32. Korean.
- 27. Kim Y, Lee BH. Clinical usefulness of child-centered task-oriented training on balance ability in cerebral palsy. J Phys Ther Sci 2013;25:947−51. Korean.ArticlePubMedPMC
- 28. Yang YR, Chen YC, Lee CS, et al. Dual-task-related gait changes in individuals with stroke. Gait Posture 2007;25:185−90.ArticlePubMed
- 29. Bowen A, Wenman R, Mickelborough J, et al. Dual-task effects of talking while walking on velocity and balance following a stroke. Age Ageing 2001;30:319−23.ArticlePubMed
- 30. Yang YR, Wang RY, Chen YC, et al. Dual-task exercise improves walking ability in chronic stroke: a randomized controlled trial. Arch Phys Med Rehabil 2007;88:1236−40.ArticlePubMed
- 31. Kim YJ, Son HH, Oh JL, et al. Effects of dual task balance training on balance and activities of daily living in stroke patient. J Korean Soc Phys Med 2011;6:19−29. Korean.
- 32. Liepert J, Bauder H, Wolfgang HR, et al. Treatment-induced cortical reorganization after stroke in humans. Stroke 2000;31:1210−6.ArticlePubMed
- 33. Park HK, Cho KH, Lee WH. The effects of dual task training on postural stability and balance in chronic stroke. J Korea Acad Ind Coop Soc 2011;12:3555−62. Korean.Article
- 34. Sim SM, Oh DW. Effect of dual-task training with cognitive motor task on walking and balance functions in patients with chronic stroke: randomized controlled pilot study. Phys Ther Korea 2015;22:11−20. Korean.Article
- 35. Yu EY. The effects of single and dual task balance training on stable and unstable surfaces on balance and walking ability in stroke patients [dissertation]. Yongin: Yongin University; 2016. Korean.
- 36. Lee TY, Kim JH. Factor analysis of element affecting activities of daily living in stroke patients. J Korean Soc Occup Ther 2001;9:25−36. Korean.
- 37. Kim MY. A study of manual functional test for CVA. J Korean Acad Occup Ther 1994;2:19−26. Korean.
- 38. Chai KJ, Lee HS. Assessment of upper extremity function in normal Korean adults by manual function test. J Korean Soc Occup Ther 1997;5:52−7. Korean.
- 39. Kang Y, Na DL, Hahn S. Seoul neuropsychological screening battery. Incheon: Human Brain Research & Consulting Co.; 2003. Korean.
- 40. Kim H, Lee YN, Jo EM, et al. Reliability and validity of culturally adapted executive function performance test for Koreans with stroke. J Stroke Cerebrovasc Dis 2017;26:1033−40.ArticlePubMed
- 41. Lee H. Development and validation of Korean version of trail making test for elderly persons [dissertation]. Seoul: Sungkyunkwan University; 2006. Korean.
- 42. Min SK, Lee CI, Kim KI, et al. Development of Korean version of WHO quality of life scale abbreviated version (WHOQOL-BREF). J Korean Neuropsychiatr Assoc 2000;39:571−9. Korean.Article
- 43. Woo HM. The effects of task-oriented dual task training on the cognitive function and daily living ability of stroke patients [dissertation]. Gyeongsan: Daegu University; 2008. Korean.
- 44. Han MR. The studies of cognitive and walking ability under dual task training applying cognitive task in stroke patients [dissertation]. Naju: Dongshin University; 2012. Korean.
- 45. Park SS, Kim SK, Yoo DH, et al. The effects of telerehabilitation based occupational therapy on executive function, activities of daily living, and occupation performance of people with stroke. Ther Sci Rehabil 2021;10:115−27. Korean.
- 46. Choi W, Lee G, Lee S. Effect of the cognitive-motor dual-task using auditory cue on balance of surviviors with chronic stroke: a pilot study. Clin Rehabil 2015;29:763−70.ArticlePubMed
- 47. Hollands KL, Agnihotri D, Tyson SF. Effects of dual task on turning ability in stroke survivors and older adults. Gait Posture 2014;40:564−9.ArticlePubMed
- 48. Plummer-D’Amato P, Kyvelidou A, Sternad D, et al. Training dual-task walking in community-dwelling adults within 1 year of stroke: a protocol for a single-blind randomized controlled trial. BMC Neurol 2012;12:129. ArticlePubMedPMC
- 49. Kim JW, Kim SM, Park RJ. The effects of task-oriented functional training on standing balance in stroke patients. J Korean Phys Ther 2003;15:65−81. Korean.
- 50. Jang YS, Baek JY, Oh MH. The effect of dual task performance on the trunk control ability and upper extremity function of patients with stroke. J Rehabil Res 2012;16:311−31. Korean.
- 51. Kim K, Kim O. The effects of exercise-cognitive combined dual-task program on cognitive function and depression in elderly with mild cognitive impairment. Korean J Adult Nurs 2015;27:707−17. Korean.Article
- 52. Mirelman A, Maidan I, Herman T, et al. Virtual reality for gait training: can it induce motor learning to enhance complex walking and reduce fall risk in patients with Parkinson’s disease? J Gerontol A Biol Sci Med Sci 2011;66:234−40.ArticlePubMed
- 53. Meester D, Al-Yahya E, Dennis A, et al. A randomized controlled trial of a walking training with simultaneous cognitive demand (dual-task) in chronic stroke. Eur J Neurol 2019;26:435−41.ArticlePubMedPMC
- 54. McCulloch K. Attention and dual-task conditions: physical therapy implications for individuals with acquired brain injury. J Neurol Phys Ther 2007;31:104−18.ArticlePubMed
References
Figure & Data
References
Citations

- Intervention and assessment of executive dysfunction in patients with stroke: A scoping review
Katsuya Sakai, Yuichiro Hosoi, Junpei Tanabe, Kathleen Bennett
PLOS ONE.2024; 19(2): e0298000. CrossRef - Occupation-based interventions to improve occupational performance and participation in the hospital setting: a systematic review
Gemma Wall, Stephen Isbel, Louise Gustafsson, Claire Pearce
Disability and Rehabilitation.2023; : 1. CrossRef - The effect of five activities daily living on improving cognitive function in ischemic stroke patients
Frana Andrianur, Dwi Prihatin Era, Arifin Hidayat, Ismansyah Ismansyah, Diah Setiani
Healthcare in Low-resource Settings.2023;[Epub] CrossRef - Effect of Upper Limb Motor Rehabilitation on Cognition in Parkinson’s Disease: An Observational Study
Valentina Varalta, Elisa Evangelista, Anna Righetti, Giovanni Morone, Stefano Tamburin, Alessandro Picelli, Cristina Fonte, Michele Tinazzi, Ilaria Antonella Di Vico, Andreas Waldner, Mirko Filippetti, Nicola Smania
Brain Sciences.2022; 12(12): 1684. CrossRef


 PubReader
PubReader ePub Link
ePub Link Cite
Cite

