Articles
- Page Path
- HOME > Osong Public Health Res Perspect > Volume 3(1); 2012 > Article
-
Articles
Seroepidemiology of Hepatitis A Infection in Northeastern China, Korea, and Japan - Haesun Yuna, Hyeok-Jin Leea, Youngsil Yoona, Kisang Kima, Sungsoo Kimb, Myung-Hee Shinc, Miyuki Taniguchid, Soo Ryang Kimd, Mi Kyung Kime
-
Osong Public Health and Research Perspectives 2011;3(1):31-35.
DOI: https://doi.org/10.1016/j.phrp.2012.01.005
Published online: December 31, 2011
aDivision of Enteric and Hepatitis Viruses, Korea National Institute of Health, Osong, Korea.
bDivision of Epidemiology and Health Index, Korea Centers for Disease Control and Prevention, Osong, Korea.
cDepartment of Social & Preventive Medicine, Sungkyunkwan University School of Medicine, Suwon, Korea.
dDepartment of Gastroenterology, Kobe Asahi Hospital, Kobe, Japan.
eDepartment of Preventive Medicine, College of Medicine, Hanyang University, Seoul, Korea.
- Corresponding author. E-mail: suni93@hanmail.net
Copyright ©2012, Korea Centers for Disease Control and Prevention
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License () which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
-
Objectives
- The epidemiological patterns of endemic hepatitis A virus (HAV) are unclear in northeastern Asia depending on the ethnicity of the country in question. The purpose of this study was to investigate the seroprevalence of HAV in northeastern China, South Korea, and Japan.
-
Methods
- A total of 1,500 serum samples were collected from five groups of inhabitants (300 each) who were over 40 years of age (Korean Chinese, indigenous Chinese, South Korean, Korean living in Japan, and indigenous Japanese). The samples were screened for antibodies to HAV using an enzyme-linked immunosorbent assay.
-
Results
- Positivity for HAV antibodies was 93.7% (95% confidence interval [CI]: 90.9–96.4) in Koreans living in northeastern China, 99.7% (95% CI: 99.0–100.3) in indigenous Chinese, 98.0% (95% CI: 96.4–99.6) in indigenous Koreans, 33.3% (95% CI: 28.0–38.7) in Koreans living in Japan, and 20.4% (95% CI: 15.8–25.0) in indigenous Japanese persons. The overall anti-HAV prevalence was not significantly different between northeastern China and South Korea, but it was different in Japan.
-
Conclusions
- These results indicate that differences in seroprevalence can be attributed to geological, environmental, and socioeconomic conditions rather than ethnicity.
- Hepatitis A virus (HAV) is transmitted via the oralfecal route, mainly by the consumption of contaminated water, and is found worldwide. The epidemiologic patterns (e.g., low, intermediate, and high) of endemicity are dependent on age and the level of hygiene [1-3]. Even within a designated country, each pattern is reflective of the variable infection rate, prevailing age of the population, and mode of transmission [4,5]. Although the seroprevalence of HAV is low in children in industrialized countries with low levels of endemicity, the age group of the most susceptible population will change from children to older children and adults in these countries [6-8]. Recently, severe cases of HAV infection in nonimmune and nonimmunized adults have been on the rise [2,8,9].
- In developing countries, low economic status, high population density, and inadequate water treatment might contribute to higher levels of endemicity; more than 90% of the population acquires natural immunity before 10 years of age [5,10]. Due to improved standards of hygiene, sanitation, and socioeconomic conditions, the epidemiological pattern of HAV infection and other infectious diseases are currently undergoing changes in many developing countries [4,10,11]. Studies conducted in emerging countries have reported epidemiological changes over the last several decades, indicating that HAV affects the population at a later age with an increased risk of manifesting in its symptomatic, potentially more severe form [8,9,12].
- This study was conducted in order to improve our understanding of the comparative epidemiology of HAV in northeastern China, South Korea, and Japan.
1. Introduction
- 2.1. Study design and population
- This study is part of the Korean Emigrant Study supported by the Korea Centers for Disease Control and Prevention (KCDC). This study was initiated to elucidate the effects of environmental change, genetic susceptibility, and their interaction of hypertension, diabetes, and metabolic syndrome by comparing Korean emigrants, their host country residents, and Koreans living in Korea. The ratio between the two ethnic groups was 1:1. From May 2005 to February 2008, a total of 3,142 men and women aged 40 years or over participated in the Korean Emigrant Study.
- For this study, we randomly selected 300 Korean emigrants, 300 Chinese in Yanbian, 300 Korean emigrants, and 300 Japanese from the Kinki area (western Japan). We also randomly selected 300 Koreans living in Korea who were matched in terms of age and sex to the Chinese and Japanese sample populations.
- 2.2. Serologic tests and statistical analysis
- To determine the seroprevalence in our study populations, the presence of anti-HAV immunoglobulin (IgG) in human sera was determined using Axsym Abbott assays according to the manufacturer’s instructions (Abbott Diagnostics Division, Wiesbaden, Germany). We calculated the proportion of the HAV antibody-positive persons and achieved a 95% confidence interval (CI) using a modification of the Wald method. We used the χ2 test to compare proportions between two groups. A p value <0.05 was considered significant.
2. Materials and Methods
- The overall prevalence of HAV was 96.7% among the inhabitants of northeastern China, 99.7% (95% CI: 99.0–100.3) among the population of indigenous Chinese, and 93.7% (95% CI: 90.9–96.4) among Koreans living in China. In the former, the prevalence of HAV was 99.2% (124/125) in men and 100.0% (175/175) in women with no significant difference between the two. In terms of age, the ratios were 99.4% (among individuals in their 40s), 100.0% (50s), and 100.0% (over 60 years of age) with no significant differences between age groups. Among Koreans living in China, the prevalence was 94.6% (123/130) in men and 92.9% (158/170) in women with no significant difference between the two; in terms of age, the ratios were 93.1% (among individuals in their 40s), 91.3% (50s), and 100% (over 60 years of age) with no significant differences between age groups.
- The overall prevalence of HAV was 98.0% (95% CI: 96.4–99.6) among the inhabitants of South Korea: 98.2% (111/113) in men and 97.9% (183/187) in women. The age ratios were 95.8% (among individuals in their 40s), 99.1% (50s), and 100.0% (over 60 years of age).
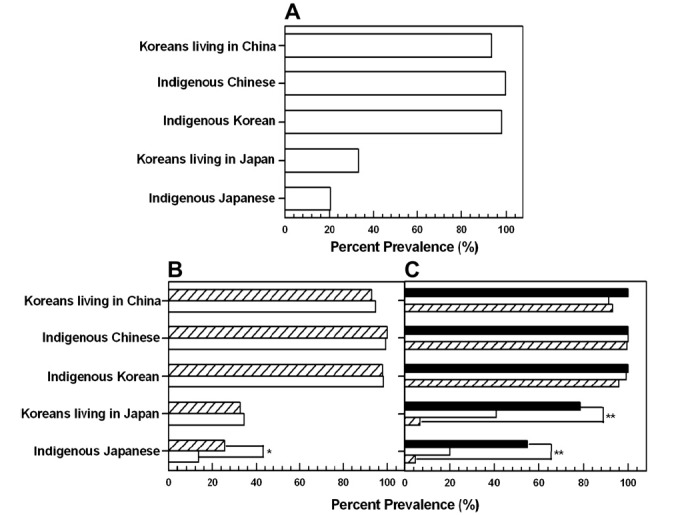
- The overall prevalence of HAV was 26.9% among inhabitants of Japan: 20.4% (95% CI: 15.8–25.0) among indigenous Japanese and 33.3% (95% CI: 28.0–38.7) among Koreans living in Japan. Among indigenous Japanese, the prevalence was 13.4% (17/127) in men and 25.6% (44/172) in women with a significant difference (p = 0.010) between the two; the age ratios were 4.7% (among individuals in their 40s), 20.0% (50s), and 55.0% (over 60 years of age) with a significant and gradual increase noted with increasing age (p < 0.00004). Among Koreans living in Japan, the prevalence was 34.4% (44/128) in men and 32.6% (56/172) in women with no significant difference between the two; the age ratios were 6.8% (among individuals in their 40s), 40.7% (50s), and 78.3% (over 60 years of age) with a significant and gradual increase noted with increasing age (p < 0.00004) (Figure. 1A–C) (Table 1).
3. Results
Prevalence of HAV. Prevalence among Koreans living in northeastern China, indigenous Chinese, indigenous Koreans, Koreans living in Japan, and indigenous Japanese (A). Prevalence by sex (B) and age (C) among the five population groups. Men: open bar; women: hatched bar. *p = 0.010; ** p < 0.00004. Ages are indicated as follow: 0–49 years of age, hatched bar; 50–59 years, open bar; > 60 years, closed bar.
- Since 2001, Korea has experienced a nationwide outbreak of HAV, as reported in the nationwide surveillance report on acute HAV published by KCDC-Korea. The number of annual reported cases of HAV in 2005 was 798, which increased to 2081 in 2006 and 2233 in 2007. The number of cases exhibited an abrupt increase from 2008 (n = 7,895) to 2009 (n = 15, 231), but appeared to be declining in 2010 (n = 6,794 through Oct 2010). As a result of improved standards of hygiene and sanitation, HAV epidemiology has rapidly shifted in Korea. At present, adolescents and young adult are the most susceptible to HAV infection because they were not naturally infected with HAV during childhood, nor have they been immunized against HAV [13-18].
- In the past, HAV was endemic in South Korea (especially in the 1980s), and most adults acquired natural immunity through asymptomatic infection [13,14]. Due to improved socioeconomic and sanitation conditions, the epidemiological pattern of HAV has rapidly improved in Korea; the seroprevalence has decreased in children, teenagers, and young adults in their 20s, though there has been an abrupt increase in patients aged 20–30 years [16,19,20]. The seroprevalence is now very low in teenagers or those in their 20s, higher among people in their 30s, and >90% among older patients [18,19]. Patients with HAV are mostly in their 20s (57.5%) and 30s (31.5%). The number of patients in the age groups (≤20 or >40 years) is relatively lower (5.2 and 5.7 %, respectively) [19].
- In 2007, Lu et al reported the serological prevalence of viral HAV, B, C, and E in 8762 randomly selected Chinese subjects in six areas of China in a cross-sectional study. The overall prevalence of the anti-HAV antibody was as high as 72.87% [21]. Anti-HAV prevalence in the ≤5, ≤10, ≤20, ≤30, ≤40, ≤50, ≤60, and > 60 years age groups was 44.7%, 51.9%, 57.6%, 73.5%, 88.3%, 91.1%, 93.5%, and 97.3%, respectively [21]. In Heilongjiang, which is located in northeastern China, the prevalence of anti-HAV was over 95% in the population > 40 years of age. Yanbian is also located in Northeastern China, and the seroprevalence in our study is consistent with previously published studies on China [21-25]. In this region there are significant differences between the two ethnic groups (i.e., Koreans living in China and indigenous Chinese). The rate of HAV seroprevalence was also found to be over 95% in Koreans > 40 years of age. These results suggest that the northeast region of China and South Korea might be highly endemic to HAV.
- According to the current age-specific rates of immunity to HAV in various regions around the world that were obtained by conducting a systematic review
- Prevalence of HAV among indigenous Japanese, Koreans living in Japan, indigenous Chinese, Koreans living in northeastern China, and indigenous Koreans
- and meta-analysis of published data, in Japan, South Korea, and Singapore the estimated level of endemicity “very low,” which means <50% of the populations has immunity by age 30 [3]. A study of the shifting seroepidemiological patterns of HAV found an association with improved sanitary conditions in Japan. The overall seroprevalence was 12.2% in 2,430 serum specimens obtained during 2003. Anti-HAV antibodies are rarely detected in individuals between 0–44 years of age, although the prevalence in individuals >50 years was 50.3% in 2003 [26]. These results were significantly lower than those of corresponding studies conducted in 1994 (74.3%), 1984 (96.9%) and 1973 (96.9%) [26,27].
- In our study, the samples obtained from a total of 1,500 men and women aged >40 years were collected from May 2005 through February 2008. The overall prevalence of HAV was 26.9% among the inhabitants of Japan: 20.4% (95% CI: 15.8–25.0) of indigenous Japanese and 33.3% (95% CI: 28.0–38.7) of Koreans living in Japan. The decline in the prevalence of anti-HAV is consistent with previous studies conducted in Japan [26,27].
- Although further efforts are needed to clarify the prevalence of HAV in younger generations (i.e., those younger than 30 years of age) and the mode of transmission mode, this study does provide certain important information concerning the prevalence of HAV in northeastern China, South Korea, and Japan based on socioeconomic status, environmental conditions, and ethnicity. Our data show that among people > 40 years of age, the prevalence of anti-HAV is not significantly different between northeastern China and South Korea; however, this prevalence is different in Japan. These results suggest that differences in seroprevalence could be attributed to geological, environmental, and socioeconomic changes rather than ethnicity.
4. Discussion
-
Acknowledgements
- This work was supported by an intramural fund of Korea National Institute of Health (No. 4800-4863-300).
- 1. Jacobsen KH Koopman JS. . Declining hepatitis A seroprevalence: a global review and analysis. Epidemiol Infect 12;2004;132(6). 1005−22. PMID: 15635957.ArticlePubMedPMC
- 2. FitzSimons D Hendrickx G Vorsters A et al.. Hepatitis A and E: update on prevention and epidemiology. Vaccine 1;2010;28(3). 583−8. PMID: 19925903.ArticlePubMed
- 3. Jacobsen KH Wiersma ST. . Hepatitis A virus seroprevalence by age and world region, 1990 and 2005. Vaccine 9;2010;28(41). 6653−7. PMID: 20723630.ArticlePubMed
- 4. Jacobsen KH Koopman JS. . The effects of socioeconomic development on worldwide hepatitis A virus seroprevalence patterns. Int J Epidemiol 6;2005;34(3). 600−9. PMID: 15831565.ArticlePubMed
- 5. Letaief A Kaabia N Gaha R et al.. Age-specific seroprevalence of hepatitis a among school children in central Tunisia. Am J Trop Med Hyg 7;2005;73(1). 40−3. PMID: 16014829.ArticlePubMed
- 6. Hepatitis. A vaccines. Wkly Epidemiol Rec 2;2000;75(5). 38−44. PMID: 10693358.PubMed
- 7. Berge JJ Drennan DP Jacobs RJ et al.. The cost of hepatitis A infections in American adolescents and adults in 1997. Hepatology 2;2000;31(2). 469−73. PMID: 10655272.ArticlePubMed
- 8. Hendrickx G Van Herck K Vorsters A et al.. Has the time come to control hepatitis A globally? Matching prevention to the changing epidemiology. J Viral Hepat 10;2008;15(Suppl 2). 1−15. PMID: 18837827.Article
- 9. Wasley A Fiore A Bell BP. . Hepatitis A in the era of vaccination. Epidemiol Rev 2006;28:101−11. PMID: 16775039.ArticlePubMed
- 10. Melnick JL. . History and epidemiology of hepatitis A virus. J Infect Dis 3;1995;171(Suppl 1). S2−8. PMID: 7876643.ArticlePubMed
- 11. Almasio PL Amoroso P. . HAV infection in chronic liver disease: a rationale for vaccination. Vaccine 6;2003;21(19–20). 2238−41. PMID: 12744849.ArticlePubMed
- 12. Wang SM Liu CC Huang YS et al.. Change in hepatitis A virus seroepidemiology in southern Taiwan: a large percentage of the population lack protective antibody. J Med Virol 6;2001;64(2). 104−8. PMID: 11360241.ArticlePubMed
- 13. Hong WS Kim JY. . Seroepidemiology of Hepaitis A and B infections in Seoul. J Korean Soc Intern Med 1982;25:19−26.
- 14. Song HJ Kim TH Song JH et al.. Emerging need for vaccination against hepatitis A virus in patients with chronic liver disease in Korea. J Korean Med Sci 4;2007;22(2). 218−22. PMID: 17449927.ArticlePubMedPMC
- 15. Jeong SH Lee HS. . Hepatitis A: clinical manifestations and management. Intervirology 2010;53(1). 15−9. PMID: 20068336.ArticlePubMed
- 16. Sohn YM Rho HO Park MS et al.. The changing epidemiology of hepatitis A in children and the consideration of active immunization in Korea. Yonsei Med J 2;2000;41(1). 34−9. PMID: 10731917.ArticlePubMed
- 17. Park SH Song JW. . Molecular epidemiology of Korean strains of hepatitis A virus. Korean J Hepatol 2000;6:276−86.
- 18. Lee D Cho YA Park Y et al.. Hepatitis A in Korea: epidemiological shift and call for vaccine strategy. Intervirology 2008;51(2). 70−4. PMID: 18434743.Article
- 19. Moon HW Cho JH Hur M et al.. Laboratory characteristics of recent hepatitis A in Korea: ongoing epidemiological shift. World J Gastroenterol 3;2010;16(9). 1115−8. PMID: 20205283.ArticlePubMedPMC
- 20. Lee CS Kwon KS Koh DH et al.. Declining hepatitis A antibody seroprevalence in the Korean military personnel. Jpn J Infect Dis 5;2010;63(3). 192−4. PMID: 20495272.ArticlePubMed
- 21. Lu J Zhou Y Lin X et al.. General epidemiological parameters of viral hepatitis A, B, C, and E in six regions of China: a cross-sectional study in 2007. PLoS One 2009;4(12). e8467PMID: 20041146.ArticlePubMedPMC
- 22. Purcell RH. . Hepatitis viruses: changing patterns of human disease. Proc Natl Acad Sci U S A 3;1994;91(7). 2401−6. PMID: 8146130.ArticlePubMedPMC
- 23. Geng J Xu D Gong J et al.. Assessing hepatitis A virus epidemic stochastic process in eight cities in China in 1990. Int J Epidemiol 4;1998;27(2). 320−2. PMID: 9602417.ArticlePubMed
- 24. Barzaga BN. . Hepatitis A shifting epidemiology in South-East Asia and China. Vaccine 2;2000;18(Suppl 1). S61−4. PMID: 10683551.ArticlePubMed
- 25. Cao J Wang Y Song H et al.. Hepatitis A outbreaks in China during 2006: application of molecular epidemiology. Hepatol Int 6;2009;3(2). 356−63. PMID: 19669361.ArticlePubMed
- 26. Kiyohara T Sato T Totsuka A et al.. Shifting seroepidemiology of hepatitis A in Japan, 1973-2003. Microbiol Immunol 2007;51(2). 185−91. PMID: 17310086.ArticlePubMed
- 27. Kiyohara T Satoh T Yamamoto H et al.. The latest seroepidemiological pattern of hepatitis A in Japan. Jpn J Med Sci Biol. 6;1997;50(3). 123−31. PMID: 9556753.ArticlePubMed
Figure & Data
References
Citations

- Prevalence of Anti-Hav IgG Antibodies in the Population of the Łódź Macroregion by Age Group
Gabriela Henrykowska, Kornelia Kotecka, Aleksandra Jabłkowska, Andrzej Buczyński, Joanna Woźny
Polish Hyperbaric Research.2021; 76(3): 67. CrossRef - Sero-prevalence of viral hepatitis A in a district of Sri Lanka: a community based cross-sectional study
Nalin Ariyarathna, Chrishantha Abeysena
BMC Infectious Diseases.2019;[Epub] CrossRef - Seroprevalence of Hepatitis A among Children and Young Adults Residing in Tehran, Iran: Implication for HAV Vaccination
Amitis Ramezani, Mohammad Reza Aghasadeghi, Setareh Mamishi, Shahram Sabeti, Farahnaz Bidari - Zerehpoosh, Mohammad Banifazl, Anahita Bavand, Sahar Shadanlou, Arezoo Aghakhani
Hepatitis Monthly.2018;[Epub] CrossRef - Seroepidemiology of Hepatitis Viruses and Hepatitis B Genotypes of Female Marriage Immigrants in Korea
Jae-Cheol Kwon, Hye Young Chang, Oh Young Kwon, Ji Hoon Park, In Soo Oh, Hyung Joon Kim, Jun Hyung Lee, Ha-Jung Roh, Hyun Woong Lee
Yonsei Medical Journal.2018; 59(9): 1072. CrossRef - Seroprevalence of Helicobacter pylori and Hepatitis A Virus among Children in Rural Central Taiwan
Meng-Che Wu, Chia-Hsing Sung, Yu-Chuan Chang, Chi-Lin Ho, Chih-Chiang Wu, Kuei-Hua Wu, Chun-Yi Lee, Kuen-Der Yang
Japanese Journal of Infectious Diseases.2015; 68(6): 494. CrossRef


 PubReader
PubReader Cite
Cite
