Articles
- Page Path
- HOME > Osong Public Health Res Perspect > Volume 10(3); 2019 > Article
-
Original Article
Multilevel Analysis of Socio-Demographic Disparities in Adulthood Obesity Across the United States Geographic Regions - Baksun Sung, Amin Etemadifar
-
Osong Public Health and Research Perspectives 2019;10(3):137-144.
DOI: https://doi.org/10.24171/j.phrp.2019.10.3.04
Published online: June 30, 2019
Department of Sociology, Social Work, and Anthropology, Utah State University, United States
- *Corresponding author: Baksun Sung, Department of Sociology, Social Work and Anthropology, Utah State University, 0730 Old Main Hill Logan, Utah, UT 84322-0730, United States, E-mail: baksun777@gmail.com
• Received: December 22, 2018 • Revised: May 12, 2019 • Accepted: May 17, 2019
Copyright ©2019, Korea Centers for Disease Control and Prevention
This is an open access article under the CC BY-NC-ND license (http://creativecommons.org/licenses/by-nc-nd/4.0/).
Abstract
-
Objectives
- The objective of this study was to examine the socio-demographic disparities in obesity among US adults across 130 metropolitan and micropolitan statistical areas.
-
Methods
- This study used data from the 2015 Behavioral Risk Factor Surveillance System and Selected Metropolitan/Micropolitan Area Risk Trend of 159,827 US adults aged 18 years and older. Data were analyzed using the multilevel linear regression models.
-
Results
- According to individual level analyses, socio-demographic disparities in obesity exist in the United States. Individuals with low socioeconomic status were associated with a higher body mass index. The participants from the Midwest United States tend to have higher body mass index than those who from the South. According to metropolitan and micropolitan statistical area level analyses, secondly, there were significant differences in obesity status between different areas and the relation of obesity with 5 socio-demographic factors varied across different areas. According to geospatial mapping analyses, even though obesity status by metropolitan and micropolitan statistical area level has improved overtime, differences in body mass index between United States regions are increasing from 2007 to 2015.
-
Conclusion
- Socio-demographic and regional disparities in obesity status persist among US adults. Hence, these findings underscore the need to take socio-environmental factors into account when planning obesity prevention on vulnerable populations and areas.
- Obesity has become a nationwide epidemic in the United States. The prevalence of obesity among adults (> 20 years) has consistently increased from 2001 to 2014 [1]. Obesity is linked to increased risk for non-communicable diseases including cancer, difficulty with physical movement, heart disease, mental illness, osteoarthritis, sleep apnea, stroke, and Type 2 diabetes [2–5]. Obesity and overweight together are the second leading cause of preventable death (approximately 300,000 deaths per year) in the United States, right after cigarette smoking [6,7].
- Previous studies have reported that obesity rates vary greatly between socio-demographic groups in the United States. Specifically, a larger ratio of individuals are overweight or obese among lower income groups, lower-educated groups, Non-White or Hispanics than among other socio-demographic groups [8–10]. Women have lower obesity rates than men for self-reported height and weight [8,11–13]. However, other studies have shown that even though the mean body mass index (BMI) is lower for women than men, women are gaining weight quicker than men [14]. There may no longer be a difference between men and women based on measured height and weight [9]. According to the National Health and Nutrition Examination Survey 2015–2016, the prevalence of obesity was 35.7% among young adults aged 20–39 years, 42.8% among adults aged 40–59 years, and 41.0% among adults older than 60 years of age showing that middle age and older groups had higher obesity rates than young adult groups in the United States [15]. It has been reported that there are geographical disparities in obesity in the United States [16–20]. According to national statistics, the Southern states have higher prevalence of obesity compared to other states [21,22].
- The social cognitive model of reciprocal determinism proposes that environmental factors influence individuals, groups, and their behaviors [23]. In other words, regional differences in health behavior caused by various environmental factors could lead to different health outcomes according to geographical areas. Specifically, social epidemiological research has reported that the geographical context in which people live is related to health disparities [24–28]. In terms of obesity, regional difference in lifestyle factors, environmental factors, health care resources, and socioeconomic status have been found to affect disparities in risk factors for obesity in the United States [29–34].
- Previous studies have focused on county levels to determine adulthood obesity, but little is known about geographical disparities in adulthood obesity by metropolitan and micropolitan statistical area (MMSAs) levels in the United States. Thus, the objective of this study was to examine the socio-demographic disparities in adulthood obesity and examine how this relationship is affected by geographic areas (130 MMSAs). The following associated hypotheses were examined in this study:
Introduction
- This study used data from the 2015 Behavioral Risk Factor Surveillance System (BRFSS) and Selected Metropolitan/Micropolitan Area Risk Trends (SMART). The BRFSS is the nation’s premier system of health-related telephone surveys that collected state data on US residents regarding their health-related risk behaviors, chronic health conditions, and use of preventive services. Established in 1984 in 15 states, BRFSS now collects data in 50 states as well as the District of Columbia and 3 United States territories. BRFSS completes more than 400,000 adult interviews each year, making it the largest continuously conducted health survey system in the world. BRFSS data are generally used to provide state-level estimates. BRFSS and SMART data are used to provide small area-level estimates for MMSAs which were determined by the Office of Management and Budgets. Hence, in order to create localized health information that can help public health practitioners identify local emerging health problems, plan and assess local responses, the Centers for Disease Control and Prevention analyzes BRFSS and SMART data. This specific data selected for this study was from 2015 and was city and countywide including 159,827 US adults aged 18 years and older [35]. This study did not require approval from the institutional review board because the BRFSS data was secondary data that did not include personal information.
- 1. Why MMSAs selected rather than another type of local administrative unit?
- MMSAs represent geographic areas that satisfy standard definitions determined by the United States Office of Management and Budget (OMB), which are used by the Census Bureau and other federal, state, and local governmental entities. MMSAs consist of counties and the BRFSS collects data about county of residence. This county information allows the reporting of information by MMSAs. Some cities and counties were excluded from SMART and BRFSS. In order for an MMSA to be included in SMART BRFSS there must be at least 500 respondents within the MMSA and the weighting criteria must be applicable. In order for a county to be included, the county must be within a selected MMSA and the weighting criteria must be applicable at the county level. The State’s BRFSS Coordinator handles these cases [35].
- 2. Measures
- BMI was used as a measure of obesity and it was computed by dividing an individual’s weight by their height squared. BMI is closely linked with percentage body fat and total body fat [36]. Individuals with a BMI of 25 kg/m2 to 29 kg/m2 were regarded as overweight, and individuals with a BMI of 30 kg/m2 or more were considered obese [37].
- Gender was categorized into males and females. Age was categorized into 18–44 years and ≥ 45 years. The education level was categorized into higher education (≥ college diploma) and lower education (< college diploma). Race was categorized into Non-White or Hispanic and Non-Hispanic White. The household income level was categorized into ≥ $50,000 and < $50,000. Regions were categorized into 5 groups (South, Northeast, Midwest, West, Puerto Rico).
- Physical activity was categorized into yes and no. Fruit consumption was categorized into ≤ 1 time per month and ≥ 1 time per week.
- 3. Statistical Analysis
- Descriptive statistics with using chi-square (Table 1) and line graph analysis are presented in Figure 1. All descriptive analyses were carried out using STATA (version 15.0, StataCorp LLC., College Station, TX).
- A mainland United States map of average adult BMI (≥ 18 years) by MMSAs levels in 2007, 2011, and 2015 was created using Arc GIS 10.6 with R (Figure 2).
- To examine the socio-demographic and regional disparities in adulthood obesity among US adults across 130 MMSAs, 3 multilevel linear regression models of BMI were conducted using STATA. Firstly, the null hypothesis model was implemented (Model I) to determine whether there was a difference in obesity status and these statistical areas. Secondly, the random-intercepts model (Model II) was implemented which considers individual-level predictors in the fixed part to examine how the 6 socio-demographic variables affect obesity status after adjusting for obesity-related health behaviors such as physical activity and fruit consumption. Finally, the random-slope model (Model III) was implemented to examine whether or not obesity status and with the 5 socio-demographic variables varied across the 130 MMSAs.
Materials and Methods
2.1. Dependent variable: obesity
2.2. Independent variables: socio-demographic variables
2.3. Control variables
- Table 1 shows the percentages of obesity rate among US adults ≥ 18 years (N = 159,827). The average percentage of obese people (BMI ≥ 30) in the 130 MMSAs was 29.06% (SD = 4.44). Men were slightly more likely to be obese than women (29.41% versus 29.15%). Participants who were ≥ 45 years were more likely to be obese than those aged 18–44 years (30.60% versus 25.87%). Participants with a higher education (≥ college diploma) were less likely to be obese than those who had a lower education (< college diploma) (24.05% versus 33.45%). Non-White or Hispanic participants were more likely to be obese than Non-Hispanic White participants (33.38% versus 28.03%). Participants with a higher income (≥ $50,000) were less likely to be obese than those with lower income (< $50,000) (26.05% versus 33.05%). Participants from the South and the Midwest were more likely to be obese than those from the Northeast and the West (31.08% and 31.65% versus 29.96% and 25.72%).
- Table 2 shows the results of multilevel linear regression of socio-demographic status and BMI among US adults (≥ 18 years) in 130 MMSAs (N = 159,827). The average coefficient of Model I was 28.147. The metropolitan and micropolitan statistical area level residual variance at Model I was significant at the 0.001 level, which means that there were significant differences in obesity status between the 130 MMSAs. Model II, III show the unstandardized coefficients from the multilevel linear regression model of the association between socio-demographic variables and obesity status among US adults. According to full model (Model III), firstly, men were associated with higher BMI than women (B = 0.592, p < 0.001). Secondly, participants who were ≥ 45 years were associated with higher BMI than those aged 18–44 years (B = 0.709, p < 0.001). Thirdly, participants with higher education (≥ college diploma) were associated with lower BMI than those who with lower education (< college diploma) (B = −0.743, p < 0.001). Fourthly, Non-White or Hispanic participants were associated with higher BMI than Non-Hispanic white (B = 1.008, p < 0.001). Fifthly, participants with higher income (≥ $50,000) were associated with lower BMI than those who with lower income (< $50,000) (B = −0.292, p < 0.001). Finally, participants from the Midwest MMSAs areas were associated with higher BMI than those who from the South MMSAs areas (B = 0.504, p < 0.01). On the other hand, participants from the West MMSAs areas were associated with lower BMI than those who from South MMSAs areas (B = −0.576, p < 0.01).
- Random slope model (Model III) analysis shows that the metropolitan and MMSA-level residuals were all significant at the 0.001 level. It means that the obesity status relationship with the 6 socio-demographic variables varies across the 130 MMSAs.
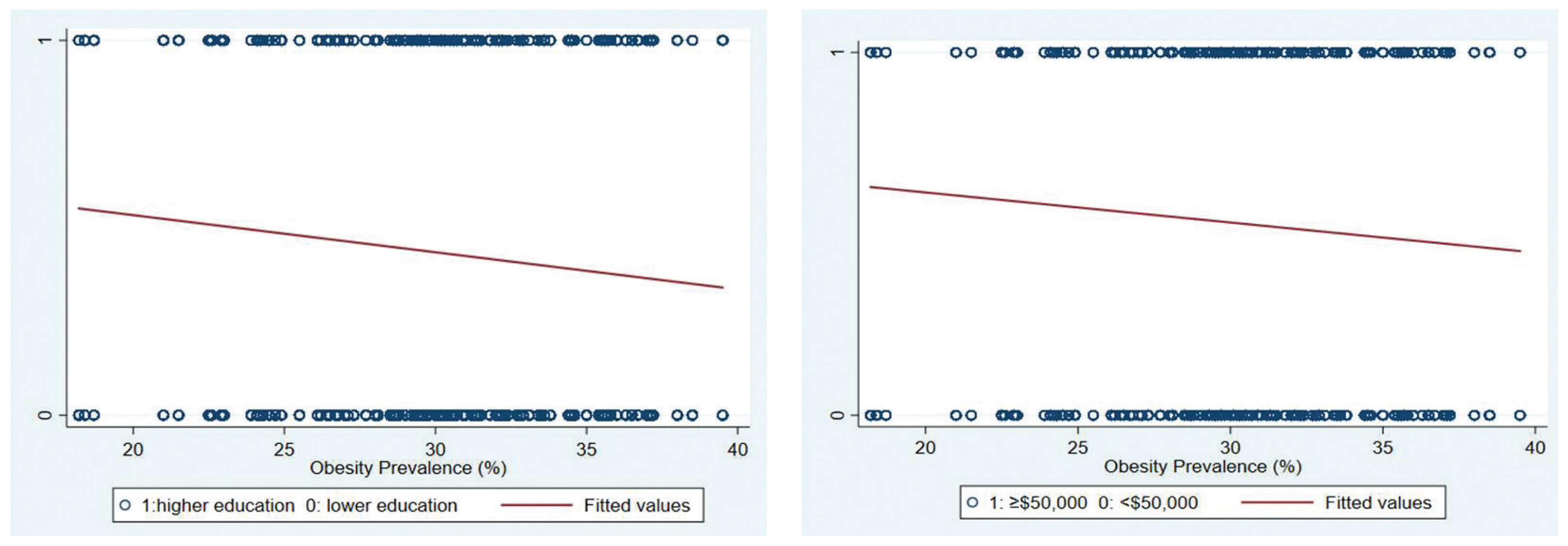
- Figure 1 displays the association between prevalence of obesity according to the areas (130 MMSAs) and socioeconomic status such as education levels and household income levels. As shown in Figure 1, areas with a higher prevalence of obesity tended to have a higher proportion of people with a lower level of education and a lower household income.
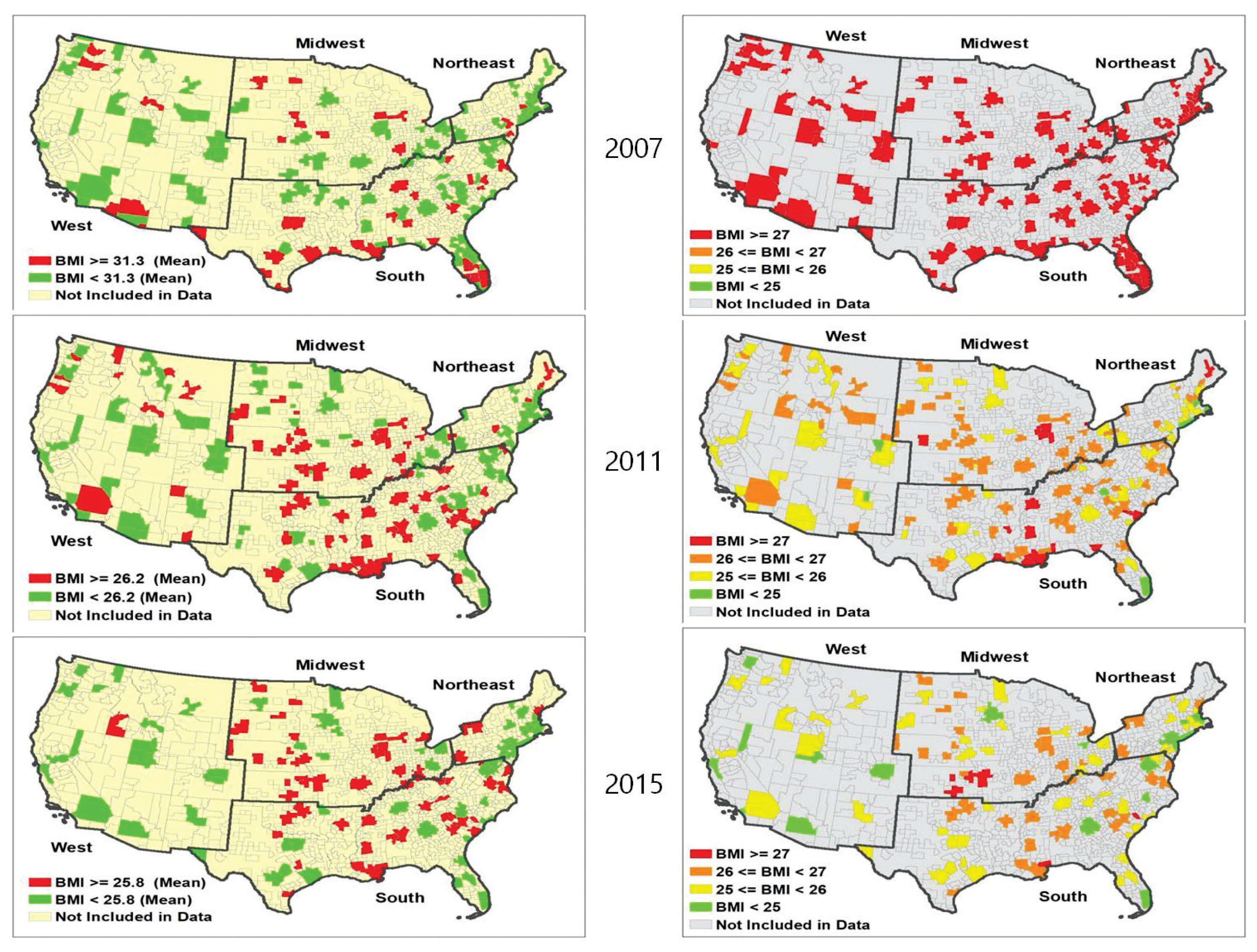
- Figure 2 displays a mainland United States map of the average adult BMI (≥18 years) by MMSAs levels in 2007, 2011, and 2015. As shown in maps on the left, the mean BMI of all MMSAs has decreased overtime. As shown in both maps, there were no significant differences in BMI according to regions in 2007. However, over time, differences in BMI between the regions widened.
Results
- This study is one of the first studies in the United States to examine socio-demographic and regional disparities in adulthood obesity by MMSAs. Multilevel analysis was used to examine the socio-demographic disparities in obesity and examine how this relationship is affected by the geographic areas (130, MMSAs).
- 1. The association between socio-demographic factors and obesity status
- This study observed that men, ≥ 45 years, with a low level of education (< college diploma), who are Non-White or Hispanic, with a low income (< $50,000) were more likely to have higher BMI than other socio-demographic groups. This finding was consistent with the hypothesis that socio-demographic disparities in obesity status persist among US adults. The findings are similar to those reported in previous studies [8–13,15]. In addition, participants from the Midwest MMSAs areas were more likely to have a higher BMI than those from the South MMSAs areas. This finding was inconsistent with the hypothesis that participants from the South MMSAs areas have higher BMI compared to those from other MMSAs areas.
- This finding is different from those reported in previous studies [21,22]. Public health authorities need to increase their efforts to reduce obesity rate targeting residents in the Midwest, although it is possible that the difference between county level analysis and MMSAs level analysis caused different results.
- 2. How socio-demographic factors and obesity status are affected by the geographic areas
- This study observed firstly that there were statistically significant differences in obesity status between different areas (130 MMSAs). Secondly, the relationship between obesity and 5 socio-demographic factors varied across different areas (130 MMSAs). Thirdly, areas with a higher prevalence of obesity tended to have a higher proportion of individuals with a low socioeconomic status (Figure 1). Fourthly, as shown in Figure 2, even though obesity status by MMSA levels has improved overtime, BMI differences between United States regions are increasing (2007 to 2015). There were no significant regional differences in BMI in 2007, but a higher BMI was more prevalent in the Midwest and the South MMSAs areas in 2015. Specifically, the highest BMIs are concentrated in MMSAs in the Midwest such as Wichita (State of Kansas), Topeka (State of Kansas), and Kansas City (State of Missouri). This finding was consistent with the hypothesis that obesity among US adults and socio-demographic status are influenced by geographic areas (130 MMSAs). La Veist [38] in 2003 and Williams and Collins [39] in 2001 reported that individuals from vulnerable groups generally live in geographically separate communities in the United States and this residential segregation can cause different environmental and social risk exposures [38,39]. In terms of obesity, socio-environmental factors are potential influential factors for the prevalence of obesity in the United States [29–34]. Hence, individual characteristics are not likely to be the major cause of the obesity epidemic in the US, whereas socio-environmental factors play a leading role. Furthermore, individuals from low socioeconomic status communities in the United States were associated with high obesity rates caused by inactive lifestyles, easy access to energy-dense food, and limited access to healthy food [40–43]. This is supported by observations presented in table 2 (Model II and Model III) and Figure 1. Regionally, in 2017, the median income in the West was $67,517, the Northeast, $66,450, the Midwest, $61,136, and the South, $55,709. Therefore, the Midwest and the South have a lower median household income compared with the West and the Northeast [44]. In 2018, 39.8% of residents in the West, 42.8% in the Northeast, 35.9% in the South, and 37.9% in the Midwest had a higher degree (post-secondary degree). This indicated that the Midwest and the South had a lower levels of educational attainment than the West and the Northeast [45]. Hence, it is possible that lower socioeconomic status could increase the risk of obesity among residents in the South and the Midwest of the United States.
- In this situation, developing policies that concentrate on revising social aspects of the environment such as promoting active lifestyles, controlling access to unhealthy food, and improving access to healthy food may decrease disparities in obesity among socio-demographic groups living in different areas. Lin et al in 2011 observed that a hypothetical 0.5 cent-per-ounce tax on sugar drink could reduce consumption of about 40–51 calories per day among children and 34–47 calories per day among adults [46]. Han et al in 2012 reported that subsidizing to healthy food resulted in a larger decrease in BMI among The Supplemental Nutrition Assistance Program (SNAP) participants [47]. Policies are guided by the social cognitive model of reciprocal determinism. Specifically, reciprocal determinism emphasizes the interaction between people and their environments [23,48]. It means that environmental factors influence individuals, groups, and their behavior, but individuals and groups can also influence their environments and regulate their own behavior. Therefore, this theory highlights disease prevention policies and promotion of public health by changing environmental factors that can have positive effects on human health and behavior [23,48].
- Adult obesity rates have continued to increase in the United States [1]. Obesity is connected to an elevated risk of non-communicable diseases including cancer, difficulty with physical movement, heart disease, mental illness, osteoarthritis, sleep apnea, stroke, and Type 2 diabetes [2–5]. With these health complications, obese people are facing a huge economic burden related to higher medical costs [49–51]. Due to the social and health implications of obesity, it is necessary to develop tailored and effective obesity prevention programs for US adults that consider socio-environmental factors.
- The observations of this study should be considered in light of several limitations. Firstly, the temporal causal relationship between 5 socio-demographic variables and the obesity status cannot be determined because the study design was cross-sectional. Therefore, follow-up studies that are a prospective longitudinal design are needed to verify the findings of this study. Secondly, this study was based on self-reported socio-demographic and obesity status. It is possible that participants could not answer their socio-demographic and obesity status precisely, which might lead to inaccurate estimations of socio-demographic and obesity status. Thirdly, this study could not address the specific causes of regional disparities in obesity in the United States. Hence, follow-up studies are needed.
Discussion
- Despite the limitations of this study, identifying the socio-demographic and regional disparities in adulthood obesity using large sample size data, provided meaningful results. This study’s finding also provides socio-environmental implications to prevent and reduce obesity US adults. Methodologically, this study was significant in the sense that it was one of the first attempts to apply MMSAs level data to analyze socio-demographic and regional disparities in adulthood obesity in the United States. The MMSAs level data-method employed in this study yielded a more specific estimate of the obesity status in adults in the US metropolitan and micropolitan areas.
- In conclusion, socio-demographic and regional disparities in obesity status persist among US adults. Hence, these findings underscore the need to take socio-environmental factors into account when planning obesity prevention interventions in vulnerable populations and areas. For example, policies that improve social aspects of the environment such as promoting active lifestyles and securing access to healthy food may reduce socio-demographic and regional disparities in obesity.
Conclusion
-
Conflicts of Interest
The authors declared no potential conflicts of interest with respect to this research, authorship, and/or publication of this article.
Article information
- 1. The state of obesity [Internet]. Obesity rates & trends overview 2018 [cited 2018 Nov 2]. Available from: https://stateofobesity.org/obesity-rates-trends-overview/.
- 2. Bhaskaran K, Douglas I, Forbes H, et al. Body-mass index and risk of 22 specific cancers: a population-based cohort study of 5•24 million UK adults. Lancet 2014;384(9945). 755−65. PMID: 10.1016/S0140-6736(14)60892-8. PMID: 25129328. PMID: 4151483.ArticlePubMedPMC
- 3. Centers for Disease Control and Prevention [Internet]. Healthy Weight. The Health Effects of Overweight and Obesity 2015 [cited 2019 May 10]. Available from: https://www.cdc.gov/healthyweight/effects/index.html.
- 4. Kasen S, Cohen P, Chen H, et al. Obesity and psychopathology in women: a three decade prospective study. Int J Obes (Lond) 2008;32(3). 558−66. PMID: 10.1038/sj.ijo.0803736.ArticlePubMedPDF
- 5. Luppino FS, de Wit LM, Bouvy PF, et al. Overweight, obesity, and depression: a systematic review and meta-analysis of longitudinal studies. Arch Gen Psychiatry 2010;67(3). 220−9. PMID: 10.1001/archgenpsychiatry.2010.2. PMID: 20194822.ArticlePubMed
- 6. Satcher D. Surgeon general’s column. Commissioned Corps Bull 2002;16(2). 1−2.
- 7. Allison DB, Fontaine KR, Manson JE, et al. Annual deaths attributable to obesity in the United States. JAMA 1999;282(16). 1530−8. PMID: 10.1001/jama.282.16.1530. PMID: 10546692.ArticlePubMed
- 8. Mokdad AH, Ford ES, Bowman BA, et al. Prevalence of obesity, diabetes, and obesity-related health risk factors, 2001. JAMA 2003;289(1). 76−9. PMID: 10.1001/jama.289.1.76.ArticlePubMedPDF
- 9. Flegal KM, Carroll MD, Ogden CL, et al. Prevalence and trends in obesity among US adults, 1999–2000. JAMA 2002;288(14). 1723−7. PMID: 10.1001/jama.288.14.1723. PMID: 12365955.ArticlePubMed
- 10. Centers for Disease Control and Prevention [Internet]. Overweight & Obesity. Adult Obesity Facts 2018 [cited 2019 May 10]. Available from: https://www.cdc.gov/obesity/data/adult.html.
- 11. Mokdad AL, Serdula MK, Dietz WH, et al. The spread of the obesity epidemic in the United States, 1991–1998. JAMA 1999;282(16). 1519−22. PMID: 10.1001/jama.282.16.1519. PMID: 10546690.ArticlePubMed
- 12. Saelens BE, Sallis JF, Black JB, et al. Neighborhood-based differences in physical activity : an environment scale evaluation. Am J Public Health 2003;93(9). 1552−8. PMID: 10.2105/AJPH.93.9.1552. PMID: 12948979. PMID: 1448009.ArticlePubMedPMC
- 13. Nelson DE, Bland S, Powell-Griner E, et al. State trends in health risk factors and receipt of clinical preventive services among US adults during the 1990s. JAMA 2002;287(20). 2659−67. PMID: 10.1001/jama.287.20.2659. PMID: 12020301.ArticlePubMed
- 14. Truong KD, Sturm R. Weight gain trends across sociodemographic groups in the United States. Am J Public Health 2005;95(9). 1602−6. PMID: 10.2105/AJPH.2004.043935. PMID: 16051939. PMID: 1449404.ArticlePubMedPMC
- 15. Hales CM, Carroll MD, Fryar CD, et al. [Internet]. Prevalence of obesity among adults and youth: United States, 2015–2016. NCHS Data Brief (No. 288) October 2017 [cited 2018 Nov 2]. Available from: https://www.cdc.gov/nchs/data/databriefs/db288.pdf.
- 16. Barker LE, Kirtland KA, Gregg EW, et al. Geographic distribution of diagnosed diabetes in the U.S.: A diabetes belt. Am J Prev Med 2011;40(4). 434−9. PMID: 10.1016/j.amepre.2010.12.019. PMID: 21406277.ArticlePubMed
- 17. Liao Y, Greenlund KJ, Croft JB, et al. Factors explaining excess stroke prevalence in the US Stroke Belt. Stroke 2009;40(10). 3336−41. PMID: 10.1161/STROKEAHA.109.561688. PMID: 19679841.ArticlePubMed
- 18. Michimi A, Wimberly MC. Spatial patterns of obesity and associated risk factors in the conterminous U.S. Am J Prev Med 2010;39(2). el−l2. PMID: 10.1016/j.amepre.2010.04.008.Article
- 19. Gregg EW, Kirtland KA, Cadwell BL, et al. Estimated county-level prevalence of diabetes and obesity - United States, 2007. MMWR 2009;58(45). 1259−63.PubMed
- 20. Shrestha SS, Kirtland KA, Thompson TJ, et al. Spatial clusters of county-level diagnosed diabetes and associated risk factors in the United States. Open Diabetes J 2012;5:29−37. PMID: 10.2174/1876524601205010029.Article
- 21. Slack T, Myers CA, Martin CK, et al. The geographic concentration of U.S adult obesity prevalence and associated social, economic, and environmental factors. Obesity (Silver Spring) 2014;22(3). 868−74. PMID: 10.1002/oby.20502.ArticlePubMed
- 22. Myers CA, Slack T, Martin CK, et al. Regional disparities in obesity prevalence in the United States: A spatial regime analysis. Obesity (Silver Spring) 2015;23(2). 481−7. PMID: 10.1002/oby.20963.ArticlePubMed
- 23. Glanz K, Rimer BK, Viswanath K. Health beahvior and health education: Theory, research and practice. 4th ed. San Francisco (CA): Jossey-Bass; 2008. pp 170−1.
- 24. Bleich SN, Thorpe RJ, Sharif-Harris H, et al. Social context explains race disparities in obesity among women. J Epidemiol Community Health 2010;64(5). 465−9. PMID: 10.1136/jech.2009.096297. PMID: 20445215. PMID: 3099623.ArticlePubMedPMC
- 25. Gaskin DJ, Price A, Brandon DT, et al. Segregation and disparities in health services use. Med Care Res Rev 2009;66(5). 578−89. PMID: 10.1177/1077558709336445. PMID: 19460811. PMID: 3099538.ArticlePubMedPMC
- 26. LaVeist TA, Thorpe RJ, Bowen-Reid T, et al. Exploring health disparities in integrated communities: Overview of the EHDIC study. J Urban Health 2008;85(1). 11−21. PMID: 10.1007/s11524-007-9226-y.ArticlePubMedPDF
- 27. LaViest TA, Thorpe RJ, Galarraga JE, et al. Environmental and socio-economic factors as contributors to racial disparities in diabetes prevalence. J Gen Intern Med 2009;24(10). 1144−8. PMID: 10.1007/s11606-009-1085-7.ArticlePubMedPMCPDF
- 28. Thorpe RJ, Wilson-Frederick SM, Bowie JV, et al. Health behaviors and all-cause mortality in African American men. Am J Mens Health 2013;7(4 Suppl). 8S−18S. PMID: 10.1177/1557988313487552. PMID: 23649171. PMID: 4086642.ArticlePubMedPMC
- 29. Berry TR, Spence JC, Blanchard CM, et al. A longitudinal and cross-sectional examination of the relationship between reasons for choosing a neighbourhood, physical activity and body mass index. Int J Behav Nutr Phys Act 2010;7:57PMID: 10.1186/1479-5868-7-57. PMID: 20602776. PMID: 2910030.ArticlePubMedPMC
- 30. Howard G, Prineas R, Moy C, et al. Racial and geographic differences in awareness, treatment, and control of hypertension: The Reasons for Geographic and Racial Differences in Stroke study. Stroke 2006;37(5). 1171−8. PMID: 10.1161/01.STR.0000217222.09978.ce. PMID: 16556884.ArticlePubMed
- 31. Voeks JH, McClure LA, Go RC, et al. Regional differences in diabetes as a possible contributor to the geographic disparity in stroke study. Stroke 2008;39(6). 1675−80. PMID: 10.1161/STROKEAHA.107.507053. PMID: 18388336. PMID: 3725822.ArticlePubMedPMC
- 32. Papas MA, Alberg AJ, Ewing R, et al. The built environment and obesity. Epidemiol Rev 2007;29:129−43. PMID: 10.1093/epirev/mxm009. PMID: 17533172.ArticlePubMedPDF
- 33. Do DP, Dubowitz T, Bird CE, et al. Neighborhood context and ethnicity differences in body mass index: a multilevel analysis using the NHANES III survey (1988–1994). Econ Hum Biol 2007;5(2). 179−203. PMID: 10.1016/j.ehb.2007.03.006. PMID: 17507298. PMID: 2587036.ArticlePubMedPMC
- 34. Zhang Q, Wang Y. Trends in the association between obesity and socioeconomic status in U.S. adults: 1971 to 2000. Obes Res 2004;12(10). 1622−32. PMID: 10.1038/oby.2004.202. PMID: 15536226.ArticlePubMed
- 35. Centers for Disease Control and Prevention [Internet]. Behavioral Risk Factor Surveillance System (BRFSS) 2014 [cited 2018 Nov 2]. Available from: https://www.cdc.gov/brfss/about/index.htm.
- 36. Gray DS, Fujioka K. Use of relative weight and body mass index for the determination of adiposity. J Clin Epidemiol 1991;44(6). 545−50. PMID: 10.1016/0895-4356(91)90218-X. PMID: 2037859.ArticlePubMed
- 37. Centers for Disease Control and Prevention. Healthy Weight. About Adult BMI 2017 [cited 2018 Nov 2]. Available from: https://www.cdc.gov/brfss/about/index.htm.
- 38. LaVeist TA. Racial segregation and longevity among African Americans: an individual-level analysis. Health Serv Res 2003;38(6 Pt 2). 1719−34. PMID: 10.1111/j.1475-6773.2003.00199.x.ArticlePubMedPMC
- 39. Williams DR, Collins C. Racial residential segregation: a fundamental cause of racial disparities in health. Public Health Rep 2001;116(5). 404−16. PMID: 10.1016/S0033-3549(04)50068-7.ArticlePubMedPMC
- 40. Carlson A, Frazão E. Food costs, diet quality and energy balance in the United States. Physiol Behav 2014;134:20−31. PMID: 10.1016/j.physbeh.2014.03.001. PMID: 24631301.ArticlePubMed
- 41. Dressler H, Smith C. Health and eating behavior differs between lean/normal and overweight/obese low-income women living in food-insecure environments. Am J Health Promot 2013;27(6). 358−65. PMID: 10.4278/ajhp.120119-QUAL-55. PMID: 23398131.ArticlePubMed
- 42. Krebs-Smith SM, Cook A, Subar AF, et al. US adults’ fruit and vegetable intakes, 1989 to 1991: a revised baseline for the healthy people 2000 objective. Am J Public Health 1995;85(12). 1623−9. PMID: 10.2105/AJPH.85.12.1623. PMID: 7503335. PMID: 1615724.ArticlePubMedPMC
- 43. Lee JH, Ralston RA, Truby H. Influence of food cost on diet quality and risk factors for chronic disease: A systematic review. Nutr Diet 2011;68(4). 248−61. PMID: 10.1111/j.1747-0080.2011.01554.x.Article
- 44. Fontenot K, Semega J, Kollar M. [Internet]. Income and poverty in the United States: 2017. Current Population Reports Current Population Reports September 2018 [cited 2018 Nov 2]. Available from: https://www.census.gov/content/dam/Census/library/publications/2018/demo/p60-263.pdf.
- 45. Statistical Atlas [Internet]. Educational Attainment 2018 [cited 2019 May 10]. Available from: https://statisticalatlas.com/region/West/Educational-Attainment#top.
- 46. Lin BH, Smith TA, Lee JY, et al. Measuring weight outcomes for obesity intervention strategies: The case of a sugar-sweetened beverage tax. Econ Hum Biol 2011;9(4). 329−41. PMID: 10.1016/j.ehb.2011.08.007. PMID: 21940223.ArticlePubMed
- 47. Han E, Powel LM, Isgor Z. Supplemental nutrition assistance program and body weight outcomes: the role of economic contextual factors. Soc Sci Med 2012;74(12). 1874−81. PMID: 10.1016/j.socscimed.2012.02.032. PMID: 22486839.ArticlePubMed
- 48. Zimmerman BJ, Schunk DH. Self-regulated learning and academic achievement: Theory, research, and practice. New York (NY): Sringer-Verlag; 1989. PMID: 10.1007/978-1-4612-3618-4.
- 49. Finkelstein EA, Trogdon JG, Brown DS, et al. The lifetime medical cost burden of overweight and obesity: implications for obesity prevention. Obesity (Silver Spring) 2008;16(8). 1843−8. PMID: 10.1038/oby.2008.290.ArticlePubMed
- 50. Wee CC, Phillips RS, Legedza AT, et al. Health care expenditures associated with overweight and obesity among US adults: importance of age and race. Am J Public Health 2005;95(1). 159−65. PMID: 10.2105/AJPH.2003.027946.ArticlePubMedPMC
- 51. Centers for Disease Control and Prevention [Internet]. Overweight & Obesity. Adult Obesity Causes & Consequences 2017 [cited 2019 May 10]. Available from: https://www.cdc.gov/obesity/adult/causes.html.
References
Figure 1
The association between the prevalence of obesity according to area (130 MMSAs) and socioeconomic status (education level and income level).
MMSA = metropolitan and micropolitan statistical area.
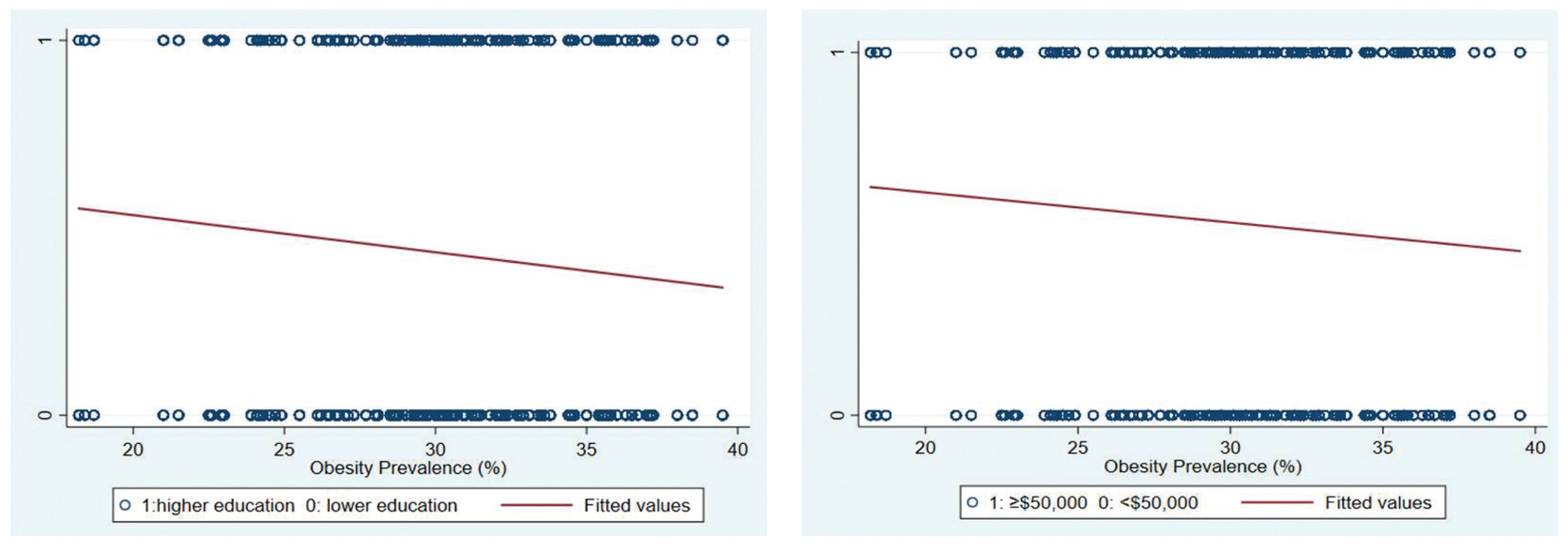

Figure 2
Mainland United States map of average adult BMI (≥ 18 years) by MMSAs levels in 2007, 2011, and 2015: BRFSS, CDC.
BMI = body mass index; BRFSS = behavioral risk factor surveillance system; MMSA = metropolitan and micropolitan statistical area.
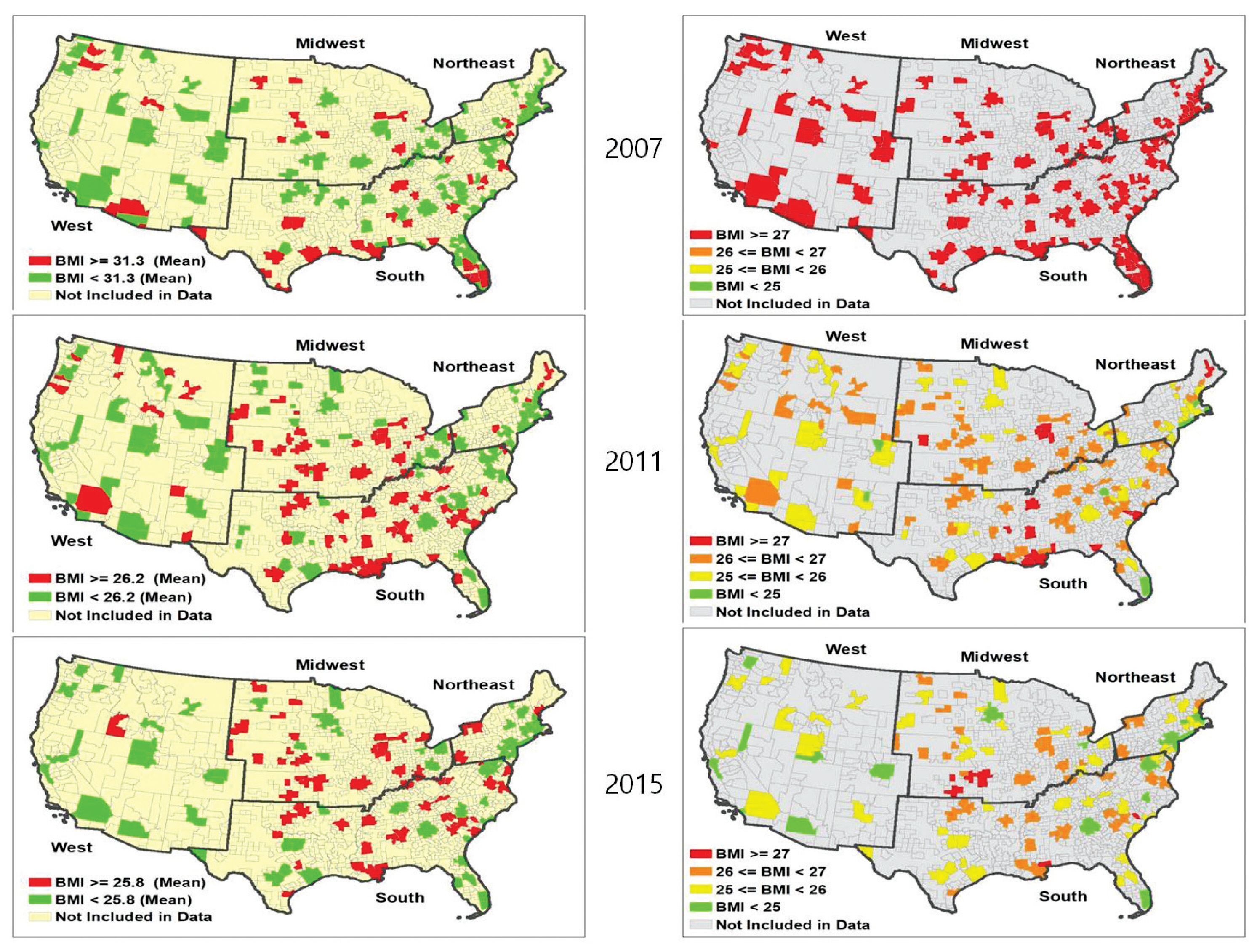

Table 1Demographics and population characteristics (N = 159,827), BRFSS and SMART, 2015.
Table 2Multilevel linear regression of socio-demographic status and BMI among US adults (≥ 18 years) (N = 159,827).
| Model I | Model II | Model III | |||||
|---|---|---|---|---|---|---|---|
| Coef | (SE) | Coef | (SE) | Coef | (SE) | ||
| Fixed effect (individual level) | |||||||
|
|
|||||||
| Intercept | 28.147*** | (0.071) | 27.105*** | (0.103) | 27.058*** | (0.118) | |
|
|
|||||||
| Gender | Male | 0.600*** | (0.033) | 0.592*** | (0.040) | ||
| Female (Ref) | |||||||
|
|
|||||||
| Age (y) | ≥ 45 | 0.721*** | (0.037) | 0.709*** | (0.052) | ||
| 18–44 (Ref) | |||||||
|
|
|||||||
| Education level | ≥ College | −0.790*** | (0.036) | −0.743*** | (0.049) | ||
| < College (Ref) | |||||||
|
|
|||||||
| Race | Non-White or Hispanic | 1.067*** | (0.043) | 1.008*** | (0.079) | ||
| Non-Hispanic White (Ref) | |||||||
|
|
|||||||
| Income level | ≥ $50,000 | −0.295*** | (0.037) | −0.292*** | (0.039) | ||
| < $50,000 (Ref) | |||||||
|
|
|||||||
| Region | Northeast | −0.359* | (0.166) | −0.293 | (0.195) | ||
| Midwest | 0.432** | (0.142) | 0.504** | (0.165) | |||
| West | −0.657*** | (0.160) | −0.576** | (0.187) | |||
| Puerto Rico | −1.468* | (0.618) | −1.227 | (0.927) | |||
| South (Ref) | |||||||
|
|
|||||||
| Physical activity | No | 1.800*** | (0.040) | 1.800*** | (0.040) | ||
| Yes (Ref) | |||||||
|
|
|||||||
| Fruit consumption | ≤ 1 per mo | 0.427*** | (0.036) | 0.422*** | (0.036) | ||
| ≥ 1 per wk (Ref) | |||||||
|
|
|||||||
| Random effect (Between MMSAs) | |||||||
|
|
|||||||
| Intercept | 0.774*** | (0.053) | 0.596*** | (0.043) | 0.653*** | (0.053) | |
|
|
|||||||
| Slopes for gender | 0.192*** | (0.052) | |||||
|
|
|||||||
| Slopes for age | 0.350*** | (0.046) | |||||
|
|
|||||||
| Slopes for education level | 0.324*** | (0.052) | |||||
|
|
|||||||
| Slopes for race | 0.654*** | (0.073) | |||||
|
|
|||||||
| Slopes for income level | 0.106*** | (0.078) | |||||
Figure & Data
References
Citations
Citations to this article as recorded by 

- County‐level socio‐environmental factors and obesity prevalence in the United States
Pedro R. V. O. Salerno, Alice Qian, Weichuan Dong, Salil Deo, Khurram Nasir, Sanjay Rajagopalan, Sadeer Al‐Kindi
Diabetes, Obesity and Metabolism.2024; 26(5): 1766. CrossRef - Supplemental Nutrition Assistance Program (SNAP)-Authorized Grocery, Convenience, Dollar, and Restaurant or Delivery Service Settings Are Associated With Increased Obesity Prevalence in Virginia
Bailey Houghtaling, David Kniola, Sarah Misyak
American Journal of Health Promotion.2021; 35(1): 127. CrossRef - The effects of the built environment on the general health, physical activity and obesity of adults in Queensland, Australia
Siqin Wang, Yan Liu, Jack Lam, Mei-Po Kwan
Spatial and Spatio-temporal Epidemiology.2021; 39: 100456. CrossRef - Exposure to air pollutants and the gut microbiota: a potential link between exposure, obesity, and type 2 diabetes
Maximillian J. Bailey, Noopur N. Naik, Laura E. Wild, William B. Patterson, Tanya L. Alderete
Gut Microbes.2020; 11(5): 1188. CrossRef


 PubReader
PubReader ePub Link
ePub Link Cite
Cite