Articles
- Page Path
- HOME > Osong Public Health Res Perspect > Volume 13(4); 2022 > Article
-
Original Article
Clinical epidemiological applicability of real-time polymerase chain reaction for COVID-19 -
Geehyuk Kim1
 , Jun-Kyu Kang2
, Jun-Kyu Kang2 , Jungho Kim3
, Jungho Kim3 , Jiyoung Lee3
, Jiyoung Lee3 , Jin Gwack1
, Jin Gwack1
-
Osong Public Health and Research Perspectives 2022;13(4):252-262.
DOI: https://doi.org/10.24171/j.phrp.2022.0135
Published online: July 27, 2022
1Central Disease Control Headquarters, Korea Disease Control and Prevention Agency, Cheongju, Korea
2Department of Molecular Medicine and Biopharmaceutical Sciences, Graduate School of Convergence Science and Technology, Seoul National University, Seoul, Korea
3Department of Clinical Laboratory Science, College of Health Sciences, Catholic University of Pusan, Busan, Korea
- Corresponding author: Jin Gwack Central Disease Control Headquarters, Korea Disease Control and Prevention Agency, 187 Osongsaengmyeong 2-ro, Osong-eup, Heungdeok-gu, Cheongju 28159, Korea E-mail: gwackjin@korea.kr
© 2022 Korea Disease Control and Prevention Agency.
This is an open access article under the CC BY-NC-ND license (http://creativecommons.org/licenses/by-nc-nd/4.0/).
- 3,256 Views
- 159 Download
Abstract
-
Objectives
- Real-time polymerase chain reaction is currently used as a confirmatory test for coronavirus disease 2019 (COVID-19). The test results are interpreted as positive, negative, or inconclusive, and are used only for a qualitative classification of patients. However, the test results can be quantitated using threshold count (Ct) values to determine the amount of virus present in the sample. Therefore, this study investigated the diagnostic usefulness of Ct results through various quantitative analyzes, along with an analysis of clinical and epidemiological characteristics.
-
Methods
- Clinical and epidemiological data from 4,642 COVID-19 patients in April 2021 were analyzed, including the Ct values of the RNA-dependent RNA polymerase (RdRp), envelope (E), and nucleocapsid (N) genes. Clinical and epidemiological data (sex, age, underlying diseases, and early symptoms) were collected through a structured questionnaire. A correlation analysis was used to examine the relationships between variables.
-
Results
- All 3 genes showed statistically significant relationships with symptoms and severity levels. The Ct values of the RdRp gene decreased as the severity of the patients increased. Moreover, statistical significance was observed for the presence of underlying diseases and dyspnea.
-
Conclusion
- Ct values were found to be related to patients’ clinical and epidemiological characteristics. In particular, since these factors are closely related to symptoms and severity, Ct values can be used as primary data for predicting patients’ disease prognosis despite the limitations of this method. Conducting follow-up studies to validate this approach might enable using the data from this study to establish policies for preventing COVID-19 infection and spread.
- Coronavirus disease 2019 (COVID-19) has spread worldwide, starting with a cluster infection of pneumonia of unknown cause in Wuhan, China, in December 2019. On January 31, 2020, the World Health Organization (WHO) confirmed that COVID-19 had spread rapidly from person to person and declared a public health emergency [1–4]. A global pandemic was declared on March 11, 2020. Countries thereafter strengthened their quarantine and healthcare measures. As the number of COVID-19 patients and deaths increased rapidly in Korea, the national crisis alert level (for infectious disease) was raised to the highest level, “serious,” on February 23, 2020, and prompt action was taken [5]. Despite global efforts, there were 239 million confirmed cases and 4 million deaths worldwide as of October 2021, and 340,000 confirmed cases and 2,000 deaths occurred in Korea [6]. Research is ongoing in various fields to prevent the spread of COVID-19 domestically and worldwide. Most research has analyzed factors affecting disease severity and clinical outcomes [7–9]. Relationships between demographic characteristics such as weight [10,11], underlying diseases [12,13], symptoms, age [14], race [15], sex [16,17], lifestyle [18–20] and epidemiological factors have been analyzed [21–23].
- Real-time reverse-transcription quantitative polymerase chain reaction (RT-qPCR) has advantages and disadvantages due to the test itself and the sampling method [24–27]; nonetheless, it is used as a confirmatory method for diagnosing COVID-19. It is used primarily as a qualitative analysis to determine positive or negative status. However, numerical experimental values have been used in publications for quantitative analysis to interpret the test results (e.g., false-positive and false-negative) [28–32] and to identify the most appropriate sampling time or site to obtain accurate test results [33].
- Combining the above features and experimental values and qRT-PCR with clinical epidemiological analyzes enables various interpretations and analyzes. Therefore, this paper aimed to utilize experimental values for epidemiological investigations through a clinical and epidemiological analysis of confirmed COVID-19 patients.
Introduction
- Study Subjects
- The subjects were those who had complete records of clinical and epidemiological information among 18,927 confirmed COVID-19 cases from April 1 to April 30, 2021. The period of analysis was limited to ensure the fidelity of the data and to enable a thorough verification of typos/errors. Patients with inaccurate or missing information were excluded. In addition, only confirmed patients whose outcomes were certain (removed from quarantine or confirmed as dead) were included. The clinical and epidemiological data included age, sex, the presence or absence of symptoms, initial symptoms, underlying diseases and diagnostic tests (cycle threshold [Ct] values). All data were collected through epidemiological investigation reports registered in the COVID-19 information management system, supplemented, and verified through in-depth epidemiological investigation reports and electronic case report forms for information such as the severity classification. The data were reconfirmed using patient monitoring data conducted by the Patient Management Team of the Central Quarantine Countermeasures Headquarters. As a result, a total of 4,642 confirmed cases were analyzed.
- The initial symptoms were classified as fever, respiratory symptoms (cough, phlegm, sore throat, dyspnea), non-respiratory symptoms (muscle pain, headache, chills, loss of taste, loss of smell), and pneumonia (including whether pneumonia was confirmed on a chest X-ray) according to the classification of the basic epidemiological survey. Severe cases followed the classification given in the 10th edition of the COVID-19 response guidelines (Table 1).
- The experimental values used for analysis were the Ct values of RT-qPCR for the RNA-dependent RNA polymerase (RdRP), envelope (E) gene, and nucleocapsid (N) genes, as recommended by the Korea Disease Control and Prevention Agency and the Korean Society of Diagnostic Laboratory Medicine and currently used to diagnose confirmed patients [34–38]. The Korean Society of Diagnostic Laboratory Medicine and the Korea Disease Control and Prevention Agency recommend using RT-qPCR to detect 2 or more specific genes and to classify the results as positive when all genes are positive [39–41]. Diagnostic reagents and kits approved for emergency use or formally approved by the Ministry of Food and Drug Safety containing 2 or more genes were used [42].
- Unlike in other studies, control variables were considered in the above analysis. RT-qPCR is the method with the highest sensitivity and specificity and is used as a standard test for COVID-19 infection worldwide. However, it has some limitations, including the need for dedicated equipment, reagents, and skilled professionals. The equipment and reagents must undergo accurate calibration, verification, validation, and quality control. In addition, the Ct value should be read along with waveform analysis to determine whether gene amplification was performed correctly. Furthermore, RT-qPCR diagnostic kit manufacturers have small differences in the target region of the gene, from 1 to 2 nucleotide sequences to 1 to 2 codons (3 to 6 base sequences) to avoid patent infringements. Since the cut-offs of the Ct values are different for each manufacturer, errors could occur when comparing the Ct values. Hence, the analysis was limited to a single manufacturer’s diagnostic kit that went through domestic and foreign gene-related certification procedures (CAP; College of American, ISO 9001, CLIA; Clinical Laboratory Improvement Amendments) to minimize differences in these variables. In fact, when the analysis was expanded to several diagnostic kits, the results were different. In addition, since the viral load changes in a time-dependent manner after infection with COVID-19, the samples were limited to 2 days from the onset of symptoms to the date of confirmation [43–47].
- Analysis
- Data were analyzed using GraphPad Prism software ver. 5.02 (GraphPad, La Jolla, CA, USA) and PASW Statistics for Windows ver. 18.0 (SPSS Inc., Chicago, IL, USA) together with Microsoft Excel 2016 (Microsoft Corp., Redmond, WA, USA). For the normality test, the Kolmogorov-Smirnov test and Shapiro-Wilk test were performed. The statistical significance of differences in parametric and nonparametric variables was analyzed using the Student t-test and Mann-Whitney U-test. The Spearman rho and Kendall tau-b coefficients were used to analyze the correlations between variables. All statistical analyzes were considered to have statistical significance when the p-value was <0.05, presented as follows in the tables and figures: p<0.05, p<0.01, or p<0.001.
- IRB/IACUC Approval
- The study protocol was approved by the Institutional Review Board of the Korea Disease Control and Prevention Agency (IRB No: 2022-03-08-PE-A). The requirement for informed consent was waived because of the retrospective nature of this study and the Infectious Disease Control and Prevention Act..
Materials and Methods
- Demographic Characteristics
- A total of 4,642 confirmed patients were included in the study; 2,288 were males (49.3%), and 2,354 were females (50.7%), with an even male-to-female ratio (Table 2). The average age was 43.7±0.58 years. Slightly more than one-fifth of the patients (n=949, 20.4%) were in their 50s, while 753 were in their 40s (16.2%), 694 in their 60s (15.0%), 586 in their 30s (12.6%), 501 in their 20s (10.8%), 480 were 10 to 19 years old (10.3%), 276 were under 10 years old (5.9%), 236 were in their 70s (5.1%), and 164 were over 80 years or older (3.5%). Approximately one-third of patients had underlying diseases (n=1,541, 33.2%). There were 3,301 (71.1%) patients with symptoms. All patients with symptoms had fever (n=3,301, 71.1%), followed by cough (n=1,389, 29.9%), sore throat (n=1,133, 24.4%), myalgia (n=952, 20.5%), other symptoms (n=840, 18.1%), headache (n=721, 15.5%), chills (n=701, 15.1%), phlegm (n=697, 15.0%), loss of smell (n=205, 4.4%), loss of taste n=181, 3.9%), dyspnea (n=44, 0.9%), and pneumonia (n=33, 0.7%). Other symptoms included chest pain, body aches, diarrhea, runny nose, stuffy nose, and fatigue.
- Distribution of the Ct Values of the RdRp, E, and N genes
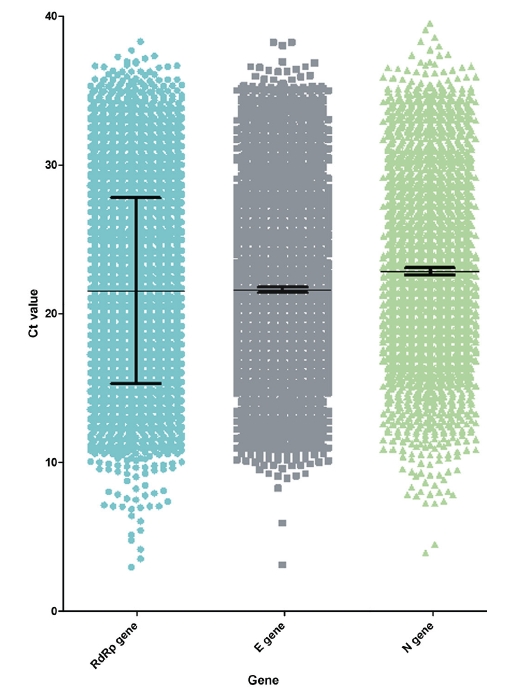
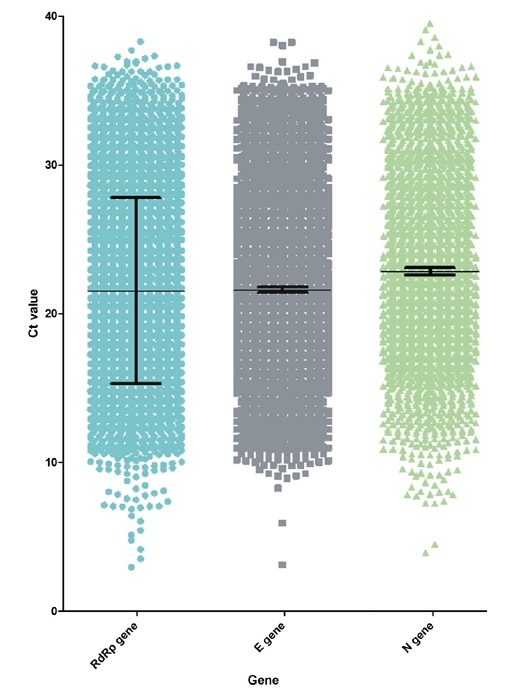
- Patients who had experimental values for all 3 genes were included in this study. The mean Ct values of the RdRp, E, and N genes were 21.5, 21.6, and 22.9, respectively (Figure 1). The minimum and maximum values were 2.9 and 38.3 for the RdRp gene, 3.1 and 38.3 for the E gene, and 3.9 and 51.5 for the N gene, respectively. The Korean Society of Diagnostic Laboratory Medicine and the Korea Disease Control and Prevention Agency recommend interpreting the results as positive when 2 or more of the 3 genes are positive [44–46]. The standard deviations were 6.3, 6,1, and 6,2, respectively.
- Ct Distribution of the RdRp, E, and N Genes according to the Presence of Symptoms
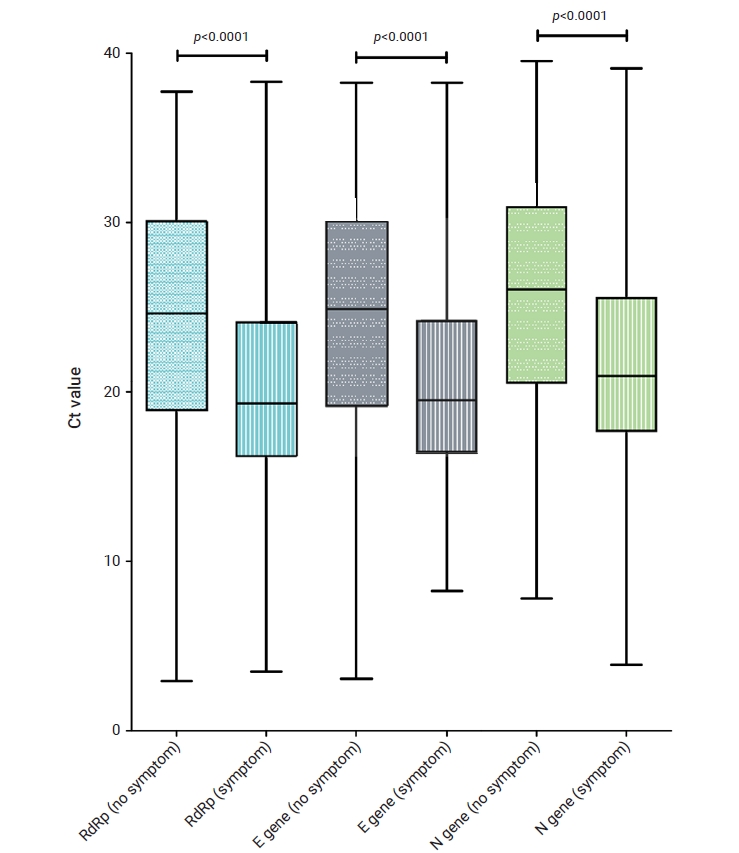
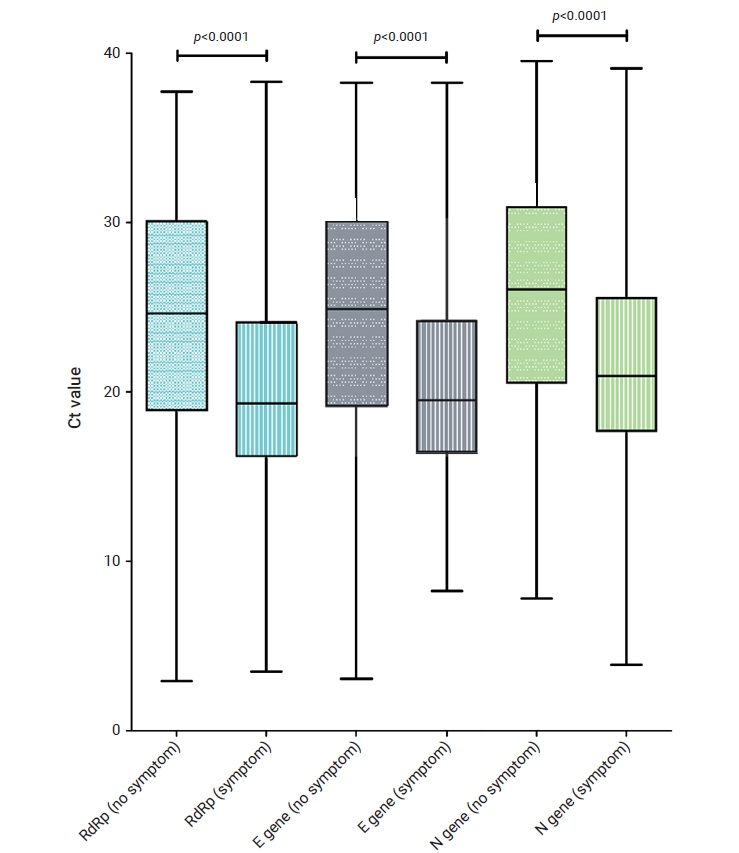
- As shown in Table 2, among the 4,642 confirmed patients, 3,301 (71.1%) had initial symptoms, which was a high proportion. When comparing the Ct values according to the presence or absence of symptoms, the RdRp, E, and N genes all showed a significant difference (p<0.001) in the distribution of Ct values between asymptomatic and symptomatic individuals (Figure 2). The median Ct values of the RdRp gene in symptomatic and asymptomatic patients were 24.6 and 19.3, respectively. For the E gene, the median Ct values were 24.5 and 20.5, respectively. For the N gene, the median Ct values were 25.6 and 21.7, respectively.
- Correlations between Severity and Ct Values of the RdRp, E, and N Genes
- Prior to conducting several other correlational analyzes, the effect of age on Ct values was investigated. When the Ct values were compared by each age group (under 10, 10−19, 20s, 30s, 40s, 50s, 60s, 70s, and over 80), none of the p-values were significant (p>0.05 for all). After confirming the absence of a correlation between age and Ct value distribution, the analysis was conducted without further consideration of age.
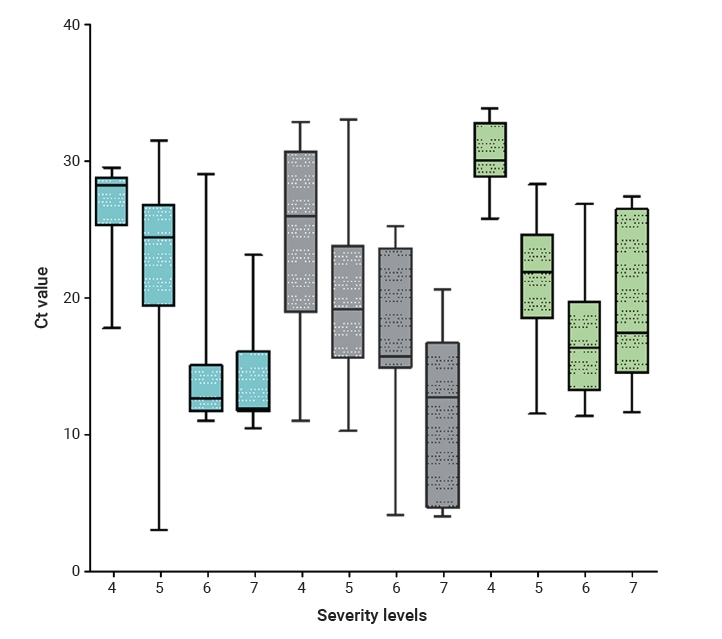
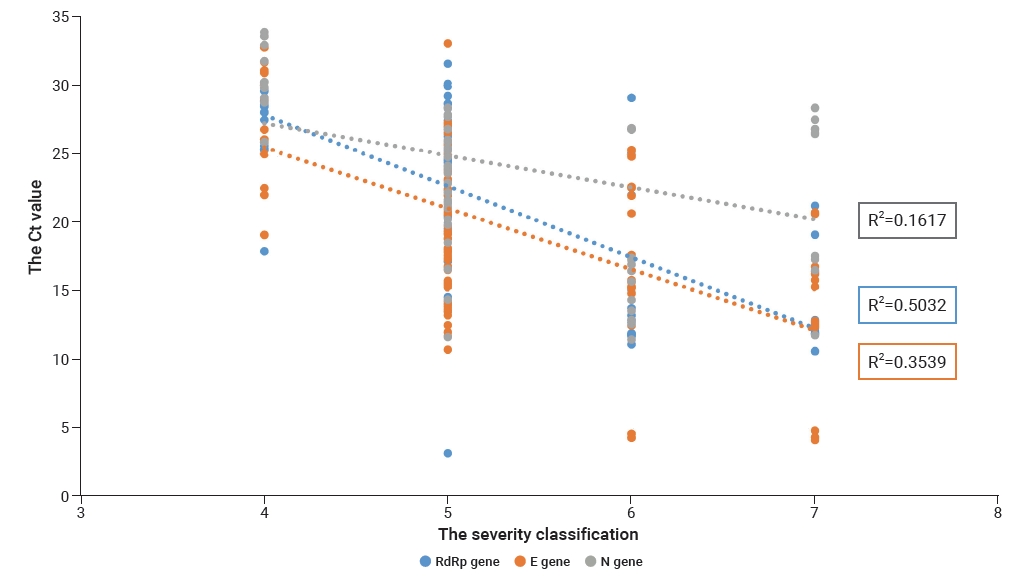
- The correlations between Ct values and symptom severity were analyzed in symptomatic subjects. The severity classification followed the 8-level classification according to the COVID-19 Response Guidelines (10th edition). In this study, analysis was limited to levels 4 to 7, since they were monitored for patient management in real time. Nonparametric analysis was performed using the Spearman rho coefficient. All statistical analyzes showed statistical significance (p<0.05), and the R2 values were 0.5, 0.4, and 0.2 for RdRp, E, and N, respectively (Figures 3, 4). The R2 value for the RdRp gene was higher than 0.5, showing a correlation between severity and the Ct value.
- Correlations and Associations between RdRp, E, and N genes and Clinical and Epidemiological Characteristics
- To examine the correlations between each gene and clinical and epidemiological characteristics, statistical significance was analyzed using the Mann-Whitney U-test (nonparametric statistical analysis when normality was not satisfied) when the independent variable was nominal (e.g., sex or the presence of underlying diseases). When the independent variable was continuous, such as age, the trend was analyzed through rank correlation analysis using Spearman coefficients (nonparametric statistical analysis when normality was not satisfied). Correlations (Table 3) were analyzed with sex and the presence of underlying diseases. Statistical significance was found for the presence of underlying diseases, but not for sex. The average Ct value of the RdRp gene in subjects without underlying diseases was 21.76, while it was 21.11 in subjects with underlying diseases, showing a slight difference. For the E gene, the average Ct value in subjects without underlying diseases was 21.80, whereas it was 21.22 in subjects with underlying diseases, likewise showing a slight difference. The analysis of associations between Ct values and each underlying disease showed statistical significance for the N gene in dementia patients (Table 4).
- Correlational Analysis between the RdRp, E, and N Genes and Symptoms
- Since the Ct values showed statistically significant relationships with the presence of symptoms (Figure 2), an additional correlational analysis was performed for each type of symptom (Table 5). Statistical significance was found for the Ct count of the RdRp gene and dyspnea, a respiratory symptom.
Results
- This study analyzed correlations and associations between the RdRp, E, and N genes and various clinical and epidemiological characteristics. Quantitatively analyzing the Ct values of these genes led to various interpretations. First, the distribution of each variable was identified (Table 2). The male-to-female ratio (49.3% vs. 50.7%) of the study subjects was similar to the male-to-female ratio (50.9% vs. 49.1%) of all confirmed cases in Korea [48]. Instead, other characteristics showed skewed ratios, different from the ratios of all confirmed cases in Korea. The distribution did not follow the normal distribution of the population. Thus, nonparametric methods (the Mann-Whitney U-test and Spearman rho coefficient) were used. Before comparing several clinical and epidemiological characteristics, the distribution of experimental values for each gene was presented (Figure 1). Similar distributions were shown for the median, mean, standard deviation, and percentile.
- In this study, symptomatic patients accounted for a high proportion (71.1%) of confirmed patients, and the experimental values showed a significant difference between the asymptomatic and symptomatic groups (Figure 2). The Ct value does not represent the exact viral load, but a higher value corresponds to a relatively low viral load [49]. For all 3 genes, the average Ct value of symptomatic subjects was lower than the average Ct value of asymptomatic subjects, with all differences being statistically significant (p<0.0001). In other words, more virus was detected in patients with symptoms. In particular, the difference in the average Ct value between symptomatic and asymptomatic patients was 4.09 for the RdRp gene, whereas smaller differences were reported for the other genes (E gene, 4.05; N gene, 3.85). Somewhat contradictory data have been published regarding these relationships [50]. As the Ct values of symptomatic and asymptomatic patients were similar in that study, it was concluded that the amounts of virus were also similar. However, it is difficult to compare the results because the age group (median age, 25 years) and the percentage of underlying diseases (3%) of the subjects of that study differed from the distribution of confirmed patients in Korea and in our study. A study [50] reporting no difference in Ct between asymptomatic and symptomatic patients did not find statistical significance in the E and N genes but, consistent with our study results, showed a significant difference (p=0.048) in the RdRp gene. This suggests that there is a difference in viral load between asymptomatic and symptomatic patients.
- The distribution of Ct values was also examined for each severity level, and significant differences were found (Figures 3, 4). The RdRp gene showed the highest correlation, as evaluated using the Spearman rho coefficient. Therefore, this finding can be interpreted as indicating that patients with lower Ct values are more likely to progress to critical severity. Reflecting this finding in policy [51] could reduce the fatality rate, since high-risk patients such as those with low Ct values could be allocated for intensive management.
- The RdRp gene yielded consistent results in various correlational analyzes, possibly reflecting the gene’s characteristics. The RdRp gene is relevant to severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the causative agent of COVID-19, as an RNA polymerase (RdRP) involved in viral replication [38]. In particular, this gene has high sensitivity and specificity in diagnosing COVID-19 and is included in most commercially available PCR diagnostic kits [47]. The E gene encodes the coat protein of the coronavirus. It is a gene detected in all beta coronaviruses (SARS-CoV, Middle East respiratory syndrome coronavirus, and SARS-CoV-2), with relatively low specificity for diagnosing COVID-19. The N gene protects the viral nucleic acid and promotes adhesion to the host cell by forming a COVID-19-specific nucleocapsid. Compared to the E gene, the N gene is specific to COVID-19, but relatively less relevant to pathogenicity than the RdRp gene, which is directly responsible for synthesizing SARS-CoV-2 viral material. For this reason, the Korea Disease Control and Prevention Agency and the WHO have recommended using the RdRp gene for confirmatory testing from the beginning of the outbreak [39,40]. This seems to be reflected in the clinical epidemiological results. In addition to symptoms and severity, the associations of Ct values with clinical and epidemiological characteristics were also analyzed (Tables 3–5). Statistically significant relationships were found between Ct values and the presence of underlying diseases. Analyzes were also performed for each symptom (Table 5), since statistically significant results were found for asymptomatic versus symptomatic patients. Statistical significance was confirmed only in dyspnea, which reflects an unusual association between Ct values and severity. However, dyspnea is directly related to the development of a severe course of disease that progresses through moderate symptoms requiring non-tubular oxygen treatment and an oxygen mask.
- Several limitations of this study should be noted. An attempt was made to analyze the trend/life cycle of Ct values measured from hospitalization to discharge, but such an analysis was not feasible due to the absence of repeatedly measured Ct values. Above all, a limitation in analyzing Ct values relates to the use of relative quantitative values for measuring the amount of fluorescence. Since this is a relative quantity, the Ct values fluctuate in every measurement, even with the same samples. It is necessary to analyze samples with absolute quantitative values to compare gene expression levels more accurately. To analyze the results, the housekeeping gene (a gene that is always expressed in any cell) is amplified as a reference gene and an internal control gene for each PCR analysis, and an absolute quantitative analysis can be performed through the delta-Ct (ΔCt) formula [52]. However, in the basic epidemiologic survey, the Ct values of the target genes (RdRp, E, and N) could be derived, but the Ct values of a reference gene and internal control gene were not available, making an absolute quantitative analysis impossible. Another limitation was that there was no control group (negative samples) because only the Ct values for positive samples were entered in the basic epidemiological survey. Various follow-up studies using a wide range of variables could be conducted to overcome these limitations. If so, it might be possible to use RT-PCR-derived Ct values as important primary data for policy establishment to prevent COVID-19 and the spread of infection.
Discussion
-
Ethics Approval
The study protocol was approved by the Institutional Review Board of the Korea Disease Control and Prevention Agency (IRB No. 2022-03-08-PE-A). The requirement for informed consent was waived because of the retrospective nature of this study and the Infectious Disease Control and Prevention Act.
-
Conflicts of Interest
The authors have no conflicts of interest to declare.
-
Funding
None.
-
Availability of Data
The datasets are not publicly available but are available from the first author upon reasonable request.
-
Authors’ Contributions
Conceptualization: GK, JG; Data curation: GK, JK, JL; Formal analysis: GK, JKK; Investigation: GK, JK, JL; Methodology: GK, JKK, JG; Project administration: GK; Resources: GK; Software: GK; Supervision: JG; Validation: JG; Visualization: GK, JKK; Writing–original draft: GK; Writing–review & editing: all authors.
Article information


| Characteristic | Value |
|---|---|
| Sex | |
| Male | 2,288 (49.3) |
| Female | 2,354 (50.7) |
| Age (y), median (range)/mean | 43.7 (0‒97)/46 |
| <10 | 276 (5.9) |
| 10−19 | 480 (10.3) |
| 20−29 | 501 (10.8) |
| 30−39 | 586 (12.6) |
| 40−49 | 753 (16.2) |
| 50−59 | 949 (20.4) |
| 60−69 | 694 (15.0) |
| 70−79 | 236 (5.1) |
| ≥80 | 164 (3.5) |
| Underlying disease | |
| Presence | 1,541 (33.2) |
| Absence | 3,101 (66.8) |
| The presence or absence of symptoms | |
| Presence | 3,301 (71.1) |
| Absence | 1,341 (28.9) |
| Symptomsa) | |
| Fever | 3,301 (71.1) |
| Cough | 1,389 (29.9) |
| Phlegm | 697 (15.0) |
| Sore throat | 1,133 (24.4) |
| Shortness of breath | 44 (0.9) |
| Muscle pain | 952 (20.5) |
| Headache | 721 (15.5) |
| Chills | 701 (15.1) |
| Taste loss | 181 (3.9) |
| Loss of smell | 205 (4.4) |
| Other | 840 (18.1) |
| Pneumonia | 33 (0.7) |
| Characteristic | Sex | Underlying disease |
|---|---|---|
| RdRp gene | 0.181 | <0.001*** |
| E gene | 0.240 | 0.002** |
| N gene | 0.187 | 0.084 |
| Comorbidities | n (%) |
p-value |
||
|---|---|---|---|---|
| RdRp gene | E gene | N gene | ||
| Hypertension | 875 (45.8) | 0.525 | 0.400 | 0.282 |
| Diabetes | 366 (19.2) | 0.272 | 0.771 | 0.383 |
| Asthma | 41 (2.1) | 0.582 | 0.567 | 0.575 |
| COPD | 31 (1.6) | 0.637 | 0.750 | 0.936 |
| Chronic kidney disease | 54 (2.8) | 0.251 | 0.668 | 0.721 |
| Rheumatologic disorder | 87 (4.6) | 0.764 | 0.102 | 0.901 |
| Chronic cardiac disease | 67 (3.5) | 0.978 | 0.107 | 0.014* |
| Liver disease | 35 (1.8) | 0.477 | 0.262 | 0.183 |
| Dementia | 52 (2.7) | 0.192 | 0.280 | <0.001*** |
| Mental disorders | 68 (3.6) | 0.758 | 0.604 | 0.809 |
| Cancer | 70 (3.7) | 0.235 | 0.494 | 0.489 |
| Any comorbidities | 165 (8.6) | 0.662 | 0.690 | 0.503 |
| Characteristic | Category |
p-value |
|||||
|---|---|---|---|---|---|---|---|
| RdRp gene | E gene | N gene | |||||
| Fever | 0.465 | 0.614 | 0.711 | ||||
| Respiratory symptoms | Cough | 0.685 | 0.713 | 0.515 | |||
| Phlegm | 0.218 | 0.311 | 0.063 | ||||
| Sore throat | 0.216 | 0.155 | 0.141 | ||||
| Shortness of breath | 0.042* | 0.070 | 0.883 | ||||
| Non-respiratory symptoms | Muscle pain | 0.208 | 0.162 | 0.582 | |||
| Headache | 0.137 | 0.091 | 0.050 | ||||
| Chills | 0.909 | 0.881 | 0.903 | ||||
| Taste loss | 0.244 | 0.188 | 0.188 | ||||
| Loss of smell | 0.106 | 0.121 | 0.138 | ||||
| Other | 0.113 | 0.078 | 0.220 | ||||
| Pneumonia | Chest imaging confirmation | 0.165 | 0.184 | 0.262 | |||
- 1. Adhikari SP, Meng S, Wu YJ, et al. Epidemiology, causes, clinical manifestation and diagnosis, prevention and control of coronavirus disease (COVID-19) during the early outbreak period: a scoping review. Infect Dis Poverty 2020;9:29. ArticlePubMedPMCPDF
- 2. Bryner J. 1st known case of coronavirus traced back to November in China [Internet]. New York: Live Science; 2020 [cited 2022 Feb 15]. Available from: https://www.livescience.com/first-case-coronavirus-found.html.
- 3. Zhu N, Zhang D, Wang W, et al. A novel coronavirus from patients with pneumonia in China, 2019. N Engl J Med 2020;382:727−33.ArticlePubMedPMC
- 4. Chan JF, Yuan S, Kok KH, et al. A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-to-person transmission: a study of a family cluster. Lancet 2020;395:514−23.ArticlePubMedPMC
- 5. Korea Disease Control and Prevention Agency. Infectious disease alert level [Internet]. Cheongju: Korea Disease Control and Prevention Agency; 2021 [cited 2021 Dec 15]. Available from: http://ncov.mohw.go.kr/tcmBoardView.do?brdId=3&brdGubun=31&dataGubun=&ncvContSeq=583&contSeq=583&board_id=311&gubun=AL. Korean.
- 6. Korea Disease Control and Prevention Agency. Infectious disease alert level [Internet]. Cheongju: Korea Disease Control and Prevention Agency; 2021 [cited 2021 Dec 15]. Available from: http://ncov.mohw.go.kr/bdBoardList_Real.do?brdId=1&brdGubun=14&ncvContSeq=&contSeq=&board_id=&gubun=. Korean.
- 7. Nucera G, Chirico F, Raffaelli V, et al. Current challenges in COVID-19 diagnosis: a narrative review and implications for clinical practice. Ital J Med 2021;15:129−34.ArticlePDF
- 8. Rahman A, Sathi NJ. Risk factors of the severity of COVID-19: a meta-analysis. Int J Clin Pract 2021;75:e13916.ArticlePubMedPDF
- 9. Du P, Li D, Wang A, et al. A systematic review and meta-analysis of risk factors associated with severity and death in COVID-19 patients. Can J Infect Dis Med Microbiol 2021;2021:6660930. ArticlePubMedPMCPDF
- 10. Malik VS, Ravindra K, Attri SV, et al. Higher body mass index is an important risk factor in COVID-19 patients: a systematic review and meta-analysis. Environ Sci Pollut Res Int 2020;27:42115−23.ArticlePubMedPMCPDF
- 11. Zhou Y, Chi J, Lv W, et al. Obesity and diabetes as high-risk factors for severe coronavirus disease 2019 (Covid-19). Diabetes Metab Res Rev 2021;37:e3377.PubMed
- 12. Yu W, Rohli KE, Yang S, et al. Impact of obesity on COVID-19 patients. J Diabetes Complications 2021;35:107817. ArticlePubMedPMC
- 13. Stefan N, Birkenfeld AL, Schulze MB. Global pandemics interconnected-obesity, impaired metabolic health and COVID-19. Nat Rev Endocrinol 2021;17:135−49.ArticlePubMedPDF
- 14. Park HY, Lee JH, Lim NK, et al. Presenting characteristics and clinical outcome of patients with COVID-19 in South Korea: a nationwide retrospective observational study. Lancet Reg Health West Pac 2020;5:100061. ArticlePubMedPMC
- 15. Suleyman G, Fadel RA, Malette KM, et al. Clinical characteristics and morbidity associated with coronavirus disease 2019 in a series of patients in metropolitan Detroit. JAMA Netw Open 2020;3:e2012270.ArticlePubMedPMC
- 16. Schurz H, Salie M, Tromp G, et al. The X chromosome and sex-specific effects in infectious disease susceptibility. Hum Genomics 2019;13:2. ArticlePubMedPMCPDF
- 17. Sward P, Edsfeldt A, Reepalu A, et al. Age and sex differences in soluble ACE2 may give insights for COVID-19. Crit Care 2020;24:221. ArticlePubMedPMCPDF
- 18. Lippi G, Henry BM. Active smoking is not associated with severity of coronavirus disease 2019 (COVID-19). Eur J Intern Med 2020;75:107−8.ArticlePubMedPMC
- 19. Patanavanich R, Glantz SA. Smoking is associated with COVID-19 progression: a meta-analysis. Nicotine Tob Res 2020;22:1653−6.ArticlePubMedPMCPDF
- 20. van Westen-Lagerweij NA, Meijer E, Meeuwsen EG, et al. Are smokers protected against SARS-CoV-2 infection (COVID-19)? The origins of the myth. NPJ Prim Care Respir Med 2021;31:10. ArticlePubMedPMCPDF
- 21. Chirico F, Nucera G, Magnavita N. Estimating case fatality ratio during COVID-19 epidemics: pitfalls and alternatives. J Infect Dev Ctries 2020;14:438−9.ArticlePubMedPDF
- 22. Tsui BCH, Deng A, Pan S. COVID-19: epidemiological factors during aerosol-generating medical procedures. Anesth Analg 2020;131:e175−8.ArticlePubMedPMC
- 23. Lechien JR, Saussez S. Importance of epidemiological factors in the evaluation of transmissibility and clinical severity of SARS-CoV-2 variants. Lancet Infect Dis 2022;22:2−3.Article
- 24. Chirico F, Nucera G, Magnavita N. Hospital infection and COVID-19: do not put all your eggs on the "swab" tests. Infect Control Hosp Epidemiol 2021;42:372−3.ArticlePubMedPMC
- 25. Chirico F, Nucera G, Ilesanmi O, et al. Identifying asymptomatic cases during the mass COVID-19 vaccination campaign: insights and implications for policy makers. Future Virol 2022;17:141−4.Article
- 26. Arnaout R, Lee RA, Lee GR, et al. SARS-CoV2 testing: the limit of detection matters [Preprint]. Posted 2020 Jun 4. bioRxiv 2020.06.02.131144. https://doi.org/10.1101/2020.06.02.131144.Article
- 27. Koskinen A, Tolvi M, Jauhiainen M, et al. Complications of COVID-19 nasopharyngeal swab test. JAMA Otolaryngol Head Neck Surg 2021;147:672−4.ArticlePubMedPMC
- 28. Vogels CB, Brito AF, Wyllie AL, et al. Analytical sensitivity and efficiency comparisons of SARS-CoV-2 RT-qPCR primer-probe sets. Nat Microbiol 2020;5:1299−305.ArticlePubMedPMCPDF
- 29. Sule WF, Oluwayelu DO. Real-time RT-PCR for COVID-19 diagnosis: challenges and prospects. Pan Afr Med J 2020;35(Suppl 2):121. Article
- 30. Bustin SA, Benes V, Garson JA, et al. The MIQE guidelines: minimum information for publication of quantitative real-time PCR experiments. Clin Chem 2009;55:611−22.ArticlePubMedPDF
- 31. Rattan A, Ahmad H. Can quantitative RT-PCR for SARS-CoV-2 help in better management of patients and control of coronavirus disease 2019 pandemic. Indian J Med Microbiol 2020;38:284−7.ArticlePubMedPMC
- 32. Sharfstein JM, Becker SJ, Mello MM. Diagnostic Testing for the Novel Coronavirus. JAMA 2020;323:1437−8.ArticlePubMed
- 33. Sethuraman N, Jeremiah SS, Ryo A. Interpreting diagnostic tests for SARS-CoV-2. JAMA 2020;323:2249−51.ArticlePubMed
- 34. Tahamtan A, Ardebili A. Real-time RT-PCR in COVID-19 detection: issues affecting the results. Expert Rev Mol Diagn 2020;20:453−4.ArticlePubMedPMC
- 35. Lee K. Laboratory diagnosis of COVID-19 in Korea. Ewha Med J 2021;44:1−10. Korean.Article
- 36. Kim JS, Kang NK, Park SM, et al. Diagnostic techniques for SARS-CoV-2 detection. J Life Sci 2020;30:731−41. Korean.
- 37. Ministry of Health and Welfare. Korea Centers for Disease Control and Prevention begins to develop a novel coronavirus test method [Internet]. Sejong: Ministry of Health and Welfare; 2020 [cited 2021 Jan 8]. Available from: http://www.mohw.go.kr/react/al/sal0301vw.jsp?PAR_MENU_ID=04&MENU_ID=0403&page=1&CONT_SEQ=352333. Korean.
- 38. Feng W, Newbigging AM, Le C, et al. Molecular diagnosis of COVID-19: challenges and research needs. Anal Chem 2020;92:10196−209.ArticlePubMedPMCPDF
- 39. Sung H, Roh KH, Hong KH, et al. COVID-19 molecular testing in Korea: practical essentials and answers from experts based on experiences of emergency use authorization assays. Ann Lab Med 2020;40:439−47.ArticlePubMedPMCPDF
- 40. Hong KH, Lee SW, Kim TS, et al. Guidelines for laboratory diagnosis of coronavirus disease 2019 (COVID-19) in Korea. Ann Lab Med 2020;40:351−60.ArticlePubMedPMCPDF
- 41. Hur KH, Park K, Lim Y, et al. Evaluation of four commercial kits for SARS-CoV-2 real-time reverse-transcription polymerase chain reaction approved by emergency-use-authorization in Korea. Front Med (Lausanne) 2020;7:521. ArticlePubMedPMC
- 42. COVID-19 Diagnosis Test Management Committee. Guidelines for the laboratory diagnosis of COVID-19 in Korea [Internet]. 4th ed. Seoul: Korean Society for Laboratory Medicine; 2020 [cited 2021 Jan 8]. Available from: https://www.kslm.org/rang_board/list.html?num=16943&code=covid19_press&key=subject_body&keyword=4%ED%8C%90. Korean.
- 43. Cevik M, Tate M, Lloyd O, et al. SARS-CoV-2, SARS-CoV, and MERS-CoV viral load dynamics, duration of viral shedding, and infectiousness: a systematic review and meta-analysis. Lancet Microbe 2021;2:e13−22.ArticlePubMed
- 44. Zou L, Ruan F, Huang M, et al. SARS-CoV-2 viral load in upper respiratory specimens of infected patients. N Engl J Med 2020;382:1177−9.ArticlePubMedPMC
- 45. Walsh KA, Jordan K, Clyne B, et al. SARS-CoV-2 detection, viral load and infectivity over the course of an infection. J Infect 2020;81:357−71.ArticlePubMedPMC
- 46. Stankiewicz Karita HC, Dong TQ, Johnston C, et al. Trajectory of viral RNA load among persons with incident SARS-CoV-2 G614 infection (Wuhan Strain) in association with COVID-19 symptom onset and severity. JAMA Netw Open 2022;5:e2142796.ArticlePubMedPMC
- 47. Kidd M, Richter A, Best A, et al. S-variant SARS-CoV-2 lineage B1.1.7 is associated with significantly higher viral load in samples tested by TaqPath polymerase chain reaction. J Infect Dis 2021;223:1666−70.ArticlePubMedPMCPDF
- 48. Korea Disease Control and Prevention Agency. Coronavirus disease-19, Republic of Korea [Internet]. Cheongju: Korea Disease Control and Prevention Agency; 2021 [cited 2021 May 10]. Available from: http://ncov.mohw.go.kr/. Korean.
- 49. Rao SN, Manissero D, Steele VR, et al. A narrative systematic review of the clinical utility of cycle threshold values in the context of COVID-19. Infect Dis Ther 2020;9:573−86.ArticlePubMedPMCPDF
- 50. Lee S, Kim T, Lee E, et al. Clinical course and molecular viral shedding among asymptomatic and symptomatic patients with SARS-CoV-2 infection in a community treatment center in the Republic of Korea. JAMA Intern Med 2020;180:1447−52.ArticlePubMedPMC
- 51. Peacock FW, Dzieciatkowski T, Chirico F, et al. Self-testing with antigen tests as a method for reduction SARS-CoV-2. Am J Emerg Med 2022;53:274−5.ArticlePubMedPMC
- 52. Rao X, Huang X, Zhou Z, et al. An improvement of the 2ˆ(-delta delta CT) method for quantitative real-time polymerase chain reaction data analysis. Biostat Bioinforma Biomath 2013;3:71−85.PubMedPMC
References
Figure & Data
References
Citations




 Cite
Cite